Semen Analysis
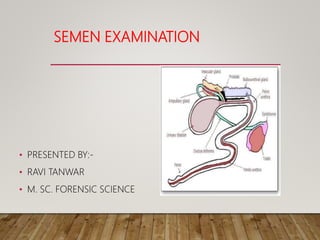
- 1. SEMEN EXAMINATION • PRESENTED BY:- • RAVI TANWAR • M. SC. FORENSIC SCIENCE
- 2. SEMEN: SEMEN IS MALE’S BODY FLUID CONTAINING PROCREATIVE HAPLOID CELLS SPERMATOZOON. - SEMEN IS COMPOSED OF CELLULAR AND FLUID PORTIONS. - TOTAL QUANTITY PER EJACULATE – 2-5 ML
- 3. BIOLOGICAL CHARACTERISTICS OF SEMEN • Typical ejaculation • 2-5 ml of semen, 160 million sperm • Seminal fluid • Medium for ejaculation • Enzymes and other proteins • Acid Phospahatase (AP), Prostate Specific Antigen (PSA), and semenogelin • Sperm cells- Spermatozoa 3
- 4. SEMEN • Semen is a human body fluid present in human males. It is a fluid with faint yellow colour and characteristic odour called seminal odour. • Volume is about 2-5 ml per ejaculate. • No. of Spermatozoa= 50,000 to 3,50,000 per ml. (10% of SP). • It is a suspension of spermatozoa in seminal plasma.
- 5. 5
- 6. BIOLOGICAL CHARACTERISTICS OF SEMEN • Semen is an extremely good source of DNA • Not all semen stains contain sperm • Vasectomy- blocks sperm from being ejaculated • Semen still produced • DNA typing probably not possible • Infertility. 6
- 7. IMPORTANT TERMS • Aspermia - complete lack of semen • (Asthenozoo)spermia - reduced sperm motility • (Azoo)spermia - absence of sperm cells in semen • (Hyper)spermia - large semen volume • (Hypo)spermia - small semen volume • (Oligo)spermia - few spermatozoa in semen • (Necro)spermia - dead or immobile sperms • (Terato)spermia - sperm with abnormal morphology
- 8. • Semen consist of the following • 1. Spermatozoa (10%) • 2. Seminal Plasma (90%) • 3. Epithelial Cell (< 1%)
- 9. SPERM: - Taken from Greek word sperma (means = seed). - About 60 um in length. - Consists of head, neck, and tail. - Head is almost occupied by nucleus. - Tail is longest part and consists of :- Middle piece, Chief piece and End piece.
- 10. SEMINAL FLUID • The seminal plasma is a mixture of secretion derived from the male accessory reproductive organs like epididymis, seminal vesicles, the prostate, vasa-deferantia, bulbourethral & urethral glands. • The seminal plasma contains Citric Acid, Ascorbic Acid, Lactic Acid, Fructose, potassium Choline Phosphate, Proteases, free Amino Acids, Ergothioniene, Zinc, Calcium, Spermine, Lipids, Enzymes like Fibrinogenase, Diastase, Acid & Alkaline Phosphatase, Glysidases, a & ß Mannosidases a & ß Glucosidases, ß Givcouridases.
- 11. PROSTATIC FLUID - ACID PHOSPHATASE - SPERMINE - CHOLESTROL - PHOSPHOLIPIDS - FIBRINOLYSIN - ZINC - THIS CONSTITUTES 30 % OF TOTAL VOLUME OF SEMEN.
- 12. Step of Examination of Seminal stain: 1. Preliminary test - Physical examination - Chemical examination 2. Confirmatory test - Microscopic examination
- 13. PRESUMPTIVE VS CONFIRMATORY TESTS • Presumptive tests • Fast, easy, inexpensive • Great for screening evidence to find possible stains • Usually detect enzymes specific to the body fluid • False positives (hence “presumptive”) • Open to attack in court • Confirmatory tests • Not available for most body fluids • Main exceptions are semen and blood 13
- 14. PHYSICAL EXAMINATION OF STAIN: •Include Visual Examination. •To naked eye seminal stains generally appear translucent or opaque spots, at times with yellowish tint and darker border depending on colour and thickness of substrata, which, if absorbent, also acquire stiffness due to dried semen.
- 15. PRESUMPTIVE TESTS FOR SEMEN • Semen fluoresces under ALS • UV light • long-wave = “Woods Lamp” = 365 nm • Crime Lite (500 nm) • Lots of false positives • Alternative light source
- 16. CHEMICAL EXAMINATION: - Florence test. for detection of choline (seminal origin) - Barberio's test for deletion of spermine (prostates origin) - Acid phosphatase test for deletion of acid phosphate (prostates origin)
- 17. FLORENCE TEST • Basis: Choline is detected in this method. • Procedure: A few drops of watery solution of the stain is extracted and taken on a slide and a drop of Florence reagent (8%) W/V solution of Iodine in water containing 5% W/V of Potassium Iodide) is poured & allowed to mix slowly under a cover slip. Dark brown crystals of choline periodide, generally needle shaped, formed with a few minutes. Non-specifics & false negative results are common.
- 18. BARBERIO’S TEST • Basis: Detection of Spermine • Procedure: A few drops of Berberio’s reagent when added to spermatic fluid produces crystals of sperm in picrate (needle shaped, rhombic & of yellow colour). • For various valid reasons, like non-specificity and lack of reproducibility, the florence and berberio’s tests have not been accepted universally.
- 19. PRESUMPTIVE TESTS FOR SEMEN • Acid phosphatase enzyme • Advantages • High levels in fresh semen stains • Very fast, inexpensive • Can be done in the field • Limitations • Activity may be weak or absent in older stains • Also present at low levels in vaginal fluid and bacteria • Not species-specific 19
- 20. PRESUMPTIVE TESTS FOR SEMEN • Overlay method • Spray a Whatman paper circle with distilled water • Lay the paper down over the suspected semen stain • Leave in contact with stain 30-60 seconds • Remove paper circle from stain and spray with AP spot solution • Look for a rapid color change to purple 20
- 21. PRESUMPTIVE TESTS FOR SEMEN • Spot test method • Wet sterile cotton swab with distilled water • Roll swab across stain • Saturate swab with AP solution 21
- 22. PRESUMPTIVE TESTS FOR SEMEN • Prostate-specific antigen (PSA) • Major protein in seminal fluid • Also detected in urine, fecal matter, sweat, milk but at much lower levels • Half-life of dried stain: 3 years • Hydrolyzes semenogelins (seminal vesicle specific antigens) • Detected with immunochromatographic test strip assay 22
- 23. PRESUMPTIVE TESTS FOR SEMEN • Semenogelins • Higher concentration in seminal fluid than PSA • Not found in urine, milk, sweat • Greater specificity for semen than PSA • Detected with immunochromatographic test strip assay 23
- 24. Confirmatory tests: Microscopic examination: - Demonstrable sperm in full size and shape is confirmatory test for presence of human semen in sample. Age of sperm. 24 – 48 hours (in vitro). up to 72 hours (in utero)
- 26. • The Microscopic detection of the Seminal stains is based in morphology of spermatozoa. • Microscopic detection of spermatozoa. Cloth pieces from different stains are taken in 0.5 ml of 0.01 N HCL in small test tubes placed in a beaker containing water. After sonication for 5 minutes the extracts and the cloth pieces are transferred to separate micro scope slides and cloth pieces delicately teased with a needle. Threads are removed and the residual liquid is gently evaporated to dryness. Residue obtained is stained haematoxylin and eosin.
- 27. FLUORESCENCE MICROSCOPY: • Is also used for detection of spermatozoa. It is based on the principle that Y Chromo some is fluorescent to quinacrine. With this method it is possible to detect both intact spermatozoa as well as the disconnected heads.
- 28. MEDICOLEGAL SIGNIFICANCE OF DETECTION OF SPERM & SEMEN -RAPE -SODOMY (Anal intercourse) -BESTIALITY Sexual intercourse by a human being with a lower animal like dogs, calves, sheep etc.), -ATTEMPTED RAPE -LUST MURDERS -AZOOSPERMIC ASSAILANTS – CHEMICAL TESTS -In case of FALSE ACCUSATION by a women -INCEST (Sexual intercourse in blood relation) -CIVIL CASES LIKE DISPUTED PATERNITY
- 29. RAPE EVIDENCE • The rape victim must undergo a medical examination as soon as possible after the assault. • At that time the appropriate items of physical evidence including clothing, hairs, and vaginal and rectal swabs can be collected for subsequent laboratory examination. • All outer and undergarments should be carefully removed and packaged separately in paper (not plastic) bags. • Bedding, or the object upon which the assault took place, may also be carefully collected.
- 30. PHYSICAL EVIDENCE FROM THE VICTIM • Pubic combings • Pubic hair standard/reference sample • External genital dry-skin areas • Vaginal swabs and smear • Cervix swab • Rectal swabs and smear • Oral swabs & smear • Head hairs • Blood sample • Fingernail scrapings • All clothing • Urine specimen
- 31. METHOD OF COLLECTION • Handling of articles bearing stains should be done very carefully to avoid damage to spermatozoa. • Vaginal / anal / penile swabs should be sent along with their smears on slides. Swabs should be taken on sterile gauze / cloth and their smears prepared on sterile slides. These should be dried in air at room temperature and swabs dispatched in sterile test tube and slides in clean wrappers.
- 32. RAPE EVIDENCE • If a suspect is apprehended within 24 hours of the assault, it may be possible to detect the victim’s DNA on the male’s underwear or on a penile swab of the suspect. • Items routinely collected from the suspect include all clothing, pubic hair, head hair, penile swab, and a blood sample or buccal swab for DNA typing. • The forceful physical contact between victim and assailant may result in a transfer of such physical evidence of blood, semen, saliva, hairs, and fibers.
- 33. THANK YOU
