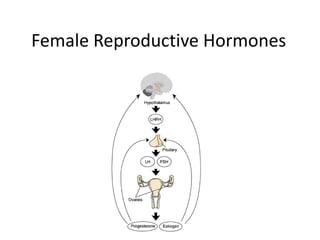
Female reproductive hormones
- 2. Females… The female reproductive system is much more complicated than the male reproductive system. The male produces sperm at a constant rate, whereas the female goes through a complicated cycle in which an egg matures and is released over the course of a month. The hormonal levels of the female fluctuate throughout her reproductive years until menopause.
- 3. The creation of an ovum is called oogenesis: Ovaries contain follicles. Follicles are made up of the primary oocyte and the granulosa cells. The primary oocyte undergoes meiosis and becomes a mature ovum. The granulosa cells provide nutrients for the oocyte. Although the ovary contains around 400 000 follicles, only about 400 or so will develop into mature ovum (from age 12 to about age 50). Since many genetic disorders occur to the offspring of older mothers, it is theorized that as the follicles mature, they become genetically inferior. Menopause signals the end of the female reproductive life as all ovarian hormones, the female sex hormones, cease to be secreted.
- 4. As the primary oocyte goes through meiosis I, one of the cells garners the majority of the cytoplasm and grows to a much larger size... this is the secondary oocyte. The remaining portion is termed a polar body. The secondary oocyte pushes against the ovary wall and eventually bursts through... ovulation. Surrounding follicle cells around the burst form the corpus luteum which secretes hormones essential for pregnancy. If pregnancy does not happen, the corpus luteum degenerates after about 10 days. The secondary oocyte undergoes meiosis II in the oviduct. The one garnering all the cytoplasm this time is the mature ovum. The other is another polar body. As with the male, there is a negative feedback loop that regulates the production of female sex hormones (progesterone and estrogen).
- 6. The Feedback Loop Hypothalamus releases gonadotropic releasing hormone (GnRH) to the pituitary Pituitary releases FSH to stimulate the follicles in the ovary to mature The follicle releases estrogen which causes the endometrial lining of the uterus to thicken This estrogen, at midcycle, also causes the pituitary to release LH and stop secreting FSH.
- 7. The Feedback Loop The rise in LH secretions cause ovulation to occur . LH makes the remaining follicles turn into the corpus luteum. The corpus luteum secretes both progesterone and a small level of estrogen which promote the building up of the endometrium. As progesterone and estrogen build up in the female, they inhibit the release of FSH and LH from the pituitary. This causes the corpus luteum to deteriorate and thus decrease the levels of estrogen and progesterone which causes menstruation.
- 8. Menstrual Cycle The whole thing lasts about 28 days, but can be irregular due to a number of factors. There are 4 phases to the menstrual cycle. Flow Phase: Days 1-5: This is the shedding of the endometrial lining and is the only phase of the female cycle that can be determined externally. It takes about 5 days for the entire lining to be shed. Follicular Phase: Days 6-13: The follicles are developing inside the ovary and as they mature they are releasing estrogen.
- 9. Menstrual Cycle Ovulation: Day 14: The egg bursts from the ovary and is caught by the fimbriae and sent into the oviduct. The corpus luteum is made from the follicles around where the egg burst. Slight dip in estrogen level when the burst occurs. Luteal Phase: Days 15-28:Estrogen and progesterone are secreted by the corpus luteum. Progesterone continues to stimulate the thickening of the uterine lining as well as preventing further ovulation and uterine contractions. If the egg is not fertilized, the concentrations of estrogen and progesterone drop which causes a return to the flow phase. Birth control pills contain high concentrations of progesterone which inhibits ovulation and thereby prevents conception.
