The Periodontal flap
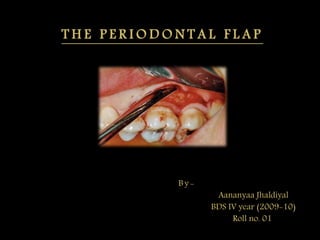
- 1. T H E P E R I O D O N T A L F L A P By- Aananyaa Jhaldiyal BDS IV year (2009-10) Roll no. 01
- 2. A periodontal flap is a section of gingiva &/or mucosa surgically separated from the underlying tissues to provide visibility of and access to the bone and root surface. A flap also allows the gingiva to be displaced to a different location in patients with mucogingival involvement.
- 3. Periodontal flaps can be classified as follows – a) Based on bone exposure after flap reflection - mucoperiosteal or full thickness flap - partial thickness or mucosal flap b) Based on placement of flap after surgery - displaced flap - non displaced flap c) Based on management of papilla - conventional flap - papilla preservation flap
- 4. 1) Full thickness or mucoperiosteal flap- All the soft tissue, including the periosteum, is reflected to expose the bone. Indication- need to view the alveolar bone 2) Partial thickness or mucosal flap- It includes only the epithelium and a layer of underlying connective tissue. The bone remains covered by a layer of connective tissue, including the periosteum. Also known as split thickness flap. Indication- when flap is to be positioned apically, laterally or coronally; or when the operator does not want to expose the bone. A) Based on bone exposure after flap reflection
- 5. Fig :A) internal bevel incision to reflect full thickness flap. B) internal bevel incision to reflect a partial thickness flap.
- 6. 1) Non – displaced flap The flap is returned and sutured in its original position. 2) Displaced flap The flap is placed apically, coronally, or laterally to its original position. 1) Conventional flap In this the interdental papilla is split beneath the contact point of the two approximating teeth to allow reflection of buccal and lingual flaps. B ) B a s e d o n f l a p p l a c e m e n t a f t e r s u r g e r y C ) B a s e d o n m a n a g e m e n t o f p a p i l l a
- 7. The incision is usually scalloped to maintain gingival morphology and retain as much papilla as possible. Indications- 1) When the interdental spaces are too narrow, thereby precluding the possibility of preserving the papilla. 2) When the flap is to be displaced. Examples- modified Widman flap, the undisplaced flap, the apically displaced flap, & the flap for reconstructive procedures. 2) Papilla preservation flap In this the entire papilla is incorporated into one of the flaps by means of crevicular interdental incisions to sever
- 8. the connective tissue attachment and a horizontal incision at the base of the papilla, leaving it connected to one of the flaps. Indications- 1) When there are open interdental spaces 2) When esthetics is of concern 3) When bone regeneration techniques are attempted.
- 9. Dictated by the surgical judgment of the operator. Depend on the objectives of the procedure. Factors to be considered in designing the flap are- 1) Degree of access to the underlying bone and root surfaces 2) Final position of the flap 3) Preservation of good blood supply to the flap Two basic flap designs are used - 1. Conventional flap 2. Papilla preservation flap
- 10. The incisions for the facial, and the lingual or palatal flap reach the tip of the interdental papilla or its vicinity, thereby splitting the papilla into facial half and a lingual or palatal half. Fig: flap design for conventional flap technique. 1 ) C o n v e n t i o n a l f l a p
- 11. papilla is preserved ( not split). The entire surgical procedure should be planned in detail before the procedure is initiated as detailed planning allows for a better clinical result. 2 ) P a p i l l a p r e s e r v a t i o n f l a p
- 12. There are basically two types of periodontal flap incisions- Horizontal incisions Vertical incisions 1) Internal bevel incision 2) Crevicular incision 3) Interdental incision 1) Oblique releasing incision
- 13. Horizontal incisions are directed along the margin of the gingiva in a mesial or a distal direction. Types of horizontal incisions recommended are- It is the incision from which the flap is reflected to expose the underlying bone and root. 1 ) I n t e r n a l b e v e l i n c i s i o n
- 14. Objectives of internal bevel incision are - 1. It removes the pocket lining 2. Conserves the relatively uninvolved outer surface of the gingiva, which when apically positioned, becomes attached gingiva. 3. Produces a sharp, thin flap margin for adaptation to the bone tooth junction. This incision is also termed as the first incision because it is the initial incision in the reflection of a periodontal flap. Also termed as reverse bevel incision because its bevel is in reverse direction from that of the gingivectomy incision.
- 15. Blade used for making this incision - #15C or #15 surgical blade. Fig: Position of the knife in performing internal bevel incision. The internal bevel incision starts from a designated area on the gingiva and is directed to an area at or near the crest of the bone.
- 16. It is made from the base of the pocket to the crest of the bone. The incision together with the initial reverse bevel incision forms a V- shaped wedge ending at or near the crest of bone. This wedge of tissue contains most of the inflamed & granulomatous areas that constitute the lateral wall of the pocket as well as the junctional epithelium & the connective tissue fibers that still persist between the bottom of the pocket & the crest of the bone. 2 ) C r e v i c u l a r i n c i s i o n
- 17. Fig : Position of knife in performing crevicular incision.
- 18. A periosteal elevator is inserted into the initial internal bevel incision, & the flap is separated from the bone . The most apical end of the internal bevel incision is exposed and visible. With this access, the surgeon is able to make the interdental incision. This incision is made to separate the collar of the gingiva that is left around the tooth. Knife used for this incision- Orban knife. 3 ) I n t e r d e n t a l i n c i s i o n
- 19. The incision is made not only around the facial & the lingual radicular area but also interdentally, connecting the facial and the lingual segments to the free the gingiva completely around the tooth. Fig : Three incisions necessary for flap surgery. A) internal bevel incision B) crevicular incision C) interdental incision.
- 20. Vertical or oblique releasing incisions can be used on one or both ends of the horizontal incision, depending on the purpose & design of the flap. Vertical incisions at both the ends are necessary if the flap is to be apically displaced. Vertical incision must extend beyond the mucogingival line, reaching the alveolar mucosa, to allow for the release of the flap to be displaced.
- 21. Vertical incisions are avoided in the lingual or palatal areas. Facial vertical incisions should not be made in the centre of an interdental papilla or over the radicular surface of a tooth. Fig : The incision should be made at the line angles.
- 22. Incisions should be made at the line angles of a tooth either to include the papilla in the flap or to avoid it completely. Vertical incisions should also be designed to avoid short flaps with long, apically directed incisions because this could jeopardize the blood supply of the flap.
- 23. S.no Type of flap Reflection accomplished by Instrument used 1) Full thickness flap or mucoperiosteal flap Blunt dissection Periosteal elevator which separates the mucoperioste um from the bone. 2) Partial thickness flap or mucosal flap Sharp dissection Surgical scalpel (#15)
- 24. Fig : Elevation of flap with periosteal elevator to obtain full thickness flap. Fig: Elevation of flap with BP knife to obtain a split thickness flap.
- 25. The purpose of suturing is to maintain the flap in the desired position until healing has progressed to the point where sutures are no longer needed. Suture materials for periodontal flap are – 1) Non absorbable •Silk: braided •Nylon: monofilament (ethilon) •EPTfe: monofilament (Gore- tex) •Polyester: braided (Ethibond)
- 26. 2) Absorbable • Surgical: gut • Plain gut ; monofilament ( 30 days) • Chromic gut ; monofilament ( 45-60 days) 3) Synthetic • Polyglycolic: braided (16 -20 days) ( vicryl; ethicon) (Dexon; Davis & Geck) • Polyglecaprone: monofilament ( 90- 120 days) (Monocryl; Ethicon) • Polyglyconate: monofilament (Maxon)
- 27. The resorbable sutures have gained popularity because they enhance patient comfort & eliminate suture removal appointments. The non resorbable silk braided suture was the most commonly used in the past due to its ease of use & low cost. The expanded polytetrafluoroethylene synthetic monofilament is an excellent nonresorbable suture widely used today. The most commonly used resorbable sutures are the natural plain gut or the chromic gut. Both are mono-
- 28. filaments and are processed from purified collagen of either sheep or cattle intestine. The chromic gut is a plain gut suture processed with chromic salts to make it resistant to enzymatic resorption, thereby increasing the resorption time. 1) The needle should enter the tissues at right angles and no less than 2 to 3 mm from the incision. 2) The needle is then carried through the tissue, following the needle's curvature. T e c h n i q u e o r p r i n c i p l e s o f s u t u r i n g
- 29. 3) The knot should not be placed over the incision. 4) The periodontal flap is closed either with independent sutures or with continuous, independent sling sutures. 5) Sutures of any type in the interdental papillae should be placed at a point located below the imaginary line that forms the base of the triangle of the interdental papilla as shown in the figure below.
- 30. 6) The location of sutures for closure of a palatal flap depends on the extent of flap elevation that has been performed. The flap is divided in four quadrants as shown in the figure below. If the elevation of the flap is slight or moderate, the sutures can be placed in the quadrant closest to the teeth. If the flap elevation is substantial, the sutures should be placed in the central quadrants of the palate.
- 31. 7) The clinician may or may not use periodontal dressings. When the flaps are not apically displaced, it is not necessary to use dressings other than for patient comfort. L i g a t i o n 1) Interdental ligation Direct Loop Suture permits a better closure of the interdental papilla . should be performed when bone grafts are used or when close apposition of the scalloped incision is required. figure-eight suture there is thread between the two flaps. used when the flaps are not in close apposition because of apical flap position or non-scalloped incisions.
- 32. 2) Sling ligation The sling ligation can be used for a flap on one surface of a tooth that involves two interdental spaces. T y p e s O f S u t u r e s 1) Horizontal mattress suture often used for the interproximal areas of diastema or for wide interdental spaces to adapt the interproximal papilla properly against the bone. can be incorporated with the continuous, independent sling sutures.
- 33. 2) Continuous, independent sling suture is used when there is both a facial and a lingual flap involving many teeth. This type of suture does not pull on the lingual flap when this flap is sutured. is especially appropriate for the maxillary arch because the palatal gingiva is attached and fibrous 3) Anchor suture This suture closes the facial and lingual flaps and adapts them tightly against the tooth.
- 34. 4) Closed-Anchor Suture Another technique to close a flap located in an edentulous area mesial or distal to a tooth. Consists of tying a direct suture that closes the proximal flap, carrying one of the threads around the tooth to anchor the tissue against the tooth, and then tying the two threads. 5) Periosteal suture used to hold the apically displaced partial-thickness flaps on the periosteum. It is of two types- 1. holding suture 2. closing suture
- 35. FIG: Periosteal sutures for an apically displaced flap. Holding sutures, shown at the bottom, are done first, followed by the closing sutures, shown at the coronal edge of the flap. 1. The Holding Suture - is a horizontal mattress suture placed at the base of the displaced flap to secure it into the new position. 2. The Closing Suture- are used to secure the flap edges to the periosteum.
- 36. 1) Immediately after suturing ( up to 24 hours) A connection between the flap and the tooth or bone surface is established which contains fibrin reticulum with many PMN leukocytes, erythrocytes, debris of injured cells, & capillaries at the edge of the wound. 2) 1-3 days after flap surgery. The space between the flap & the tooth or bone is thinner & epithetlial cells migrate over the border of the flap, usually contacting the tooth at this time.
- 37. 3) One week after surgery. An epithelial attachment to the root has been established by means of hemidesmosomes & a basal lamina. Blood clot is replaced by granulation tissue derived from the gingival connective tissue, the bone marrow, & the PDL. 4) Two weeks after surgery. Collagen fibers begin to appear parallel to the tooth surface. Union of the flap to the tooth is still weak because of presence of immature collagen collagen fibers. 5) One month after surgery. A fully epithelialized gingival crevice with a well defined epithelial attachment is present. There is beginning of functional arrangement of supra crestal fibers.
- 38. Newman, Takei, Klokkevold, Fermin A Carranza. CLINICAL PERIODONTOLOGY, 11th edition, WB Saunders 2006.
