CSF Rhinorrhea
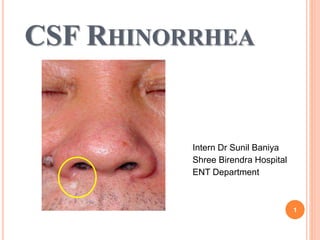
- 1. CSF RHINORRHEA Intern Dr Sunil Baniya Shree Birendra Hospital ENT Department 1
- 2. CASE The patient presented with clear nasal drips after an endoscopic nasal procedure. What is the diagnosis and subsequent management? 2
- 3. CONTENTS Definition Etiology Presentation to Hospital Physical Examinations Differential Diagnoses Laboratory Values Imaging Techniques Management Follow Up Complications Outcome & Prognosis 3
- 4. DEFINITION Leakage of CSF into the nose Clear fluid or fluid mixed with blood Rare but potentially devastating condition History: Dandy(1926): first surgical repair of CSF leak via frontal craniotomy approach Wigand (1981): use of endoscope for the first time to assist with repair of skull base defect [ 90-95% success rate with decreased associated morbidity – thus preferred] 4
- 5. 5
- 6. ETIOLOGY A. Congenital: Defective anterior neuropore closure Embryologic defect-patent fonticulus frontalis or foramen cecum B. Acquired: 1. Traumatic (9O%) 2. Iatrogenic 3. Idiopathic/ Spontaneous 4. Certain tumors 6
- 7. Traumatic CSF Rhinorrhea: 90% of CSF rhinorrhea Anterior > middle > posterior cranial fossa can be: Immediate (< 48 hours) - Motor Vehicle Accidents (MVA) Delayed (in 3 months) - proposed different theories Intact dural layer slowly herniated through bony defect Finally tearing & CSF leak Another Theory: Bony defect & dural tear +nt from the time of original injury Leakage once masking hematoma resolves 7
- 8. Iatrogenic CSF Rhinorrhea: Any surgical manipulation near skull base i. Neurosurgical: most commonly craniotomy & trans-sphenoidal pitutary resections ii. Otolaryngological: FESS (lateral lamella of cribriform plate, fovea ethmoidalis, posterior aspects of frontal recess) Septoplasty Present as: Simple cracks in bony architecture Large (>1 cm) defects Presents in within 1st week of insult 8
- 9. Idiopathic/ Spontaneous CSF Rhinorrhea: Without antecedent cause Site: anterior cranial fossa mostly subjected to wide variations of CSF pressure due to normal arterial and respiratory fluctuations Cause: secondary to raised ICP Idiopathic Intracranial Hypertension (IIH) Obstructive Sleep Apnea (OSA) Stressors: Valsalva like manoeuvers during nose blowing or straining Other causes: Focal atrophy, persistent embryonic olfactory lumen, rupture of arachnoid projections accompanying olfactory nerves 9
- 10. Congenital Tumors: 1. Locally aggressive: Inverted papilloma 2. Malignant neoplasms: eg. Glioma Erode bone of anterior cranial fossa Inflammation and potential violation of dura 10
- 11. PRESENTATION TO HOSPITAL Clear watery unilateral/ bilateral nasal discharge Anosmia- in some traumatic cases Congenital: Furstenberg sign: Meningoencephaloceles in child as intranasal/ extranasal mass Transilluminates and expands with crying (high index of suspicion with midline mass) No biopsy till complete imaging CSF otorhinorrhea: in some traumatic/ iatrogenic cases Idiopathic/ Spontaneous: headache 11
- 12. PHYSICAL EXAMINATIONS o Multimodality approach: o Reservoir sign: headache relieved due to CSF drainage externally intermittently from one of the accumulated paranasal sinuses with the change in head position Queckenstedt Stooky test: On endoscopy, CSF drainage is elicited by patient having perform Valsalva manoeuver or by compressing both jugular veins Double ring/ Halo sign: CSF detected from mixed blood when placed on filter paper with clinically detectable ring Rhinologic: Endoscopy Otologic Head and neck Neurologic evaluation 12
- 13. 13
- 14. DIFFERENTIAL DIAGNOSES Allergic Rhinitis Vasomotor Rhinitis Differences between CSF Rhinorrhea & Nasal secretions: Features CSF Rhinorrhea Nasal secretions History Trauma/ Surgery/ Tumor Sneezing, stuffinesss Flow Drops/ stream, not sniffed back Continuous, sniffed back Character Clear, watery Slimy Taste Sweet Salty Sugar +nt >30 mg/dl <10 mg/dl Beta2 transferrin Always present Always absent 14
- 15. LABORATORY VALUES Rapid but highly unreliable Not for screening or confirmation False +ve: d/t reducing substance in nasolacrimal secretions False –ve: acute meningitis 92% sensitive, 100% specific PG-D synthase Production: Arachnoid cells, oligodendrocytes & choroid plexus Altered by:renal failure, multiple sclerosis, cerebral infarction, CNS tumors Glucose Content Beta-trace protein Beta-2 transferrin Highly sensitive & specific Rapid, Non-invasive Currently single best lab test to identify +nce of CSF in sinonasal fluid Produced by neuraminidase activity Present in CSF + Perilymph + Aqueous humor 15
- 16. IMAGING TECHNIQUES 1. CT-Scan: o HRCT imaging of choice Axial plane with <1 mm thickness & reformatted into coronal and sagittal plane Congenital defects- best diagnosed with 3-D reconstruction o CT-cisternography: intrathecal contrast to identify leak easily 2. MRI: less diagnostic 3. Nuclear Medicine Studies (Serial scanning/ Scintiphotography): using DTPA, Radioactive Iodine-131 16
- 17. 17
- 18. MANAGEMENT Conservative Management: 1. 15-30˚ bed inclination: decrease CSF pressure @ basal cisterns 2. Avoid: sneezing, coughing, nose blowing & heavy lifting 3. Stool softner: to decrease straining 4. Subarachnoid lumbar drain: 5-10 ml/hr, intermittent, in small defects 5. Antibiotics: prophylactic 6. Diuretics (Acetazolamide): in spontaneous type 18
- 19. Surgical Management: o Neurosurgical intracranial approach: o Frontal craniotomy o Middle/Posterior craniotomy o Repair techniques: Free or pedicled periosteal or dural flaps Muscle plugs Mobilized portions of falx cerebri Fascia graft Flaps + fibrin glue 19
- 20. 20
- 21. Extracranial approach: • Leakage from sphenoidal sinus • Osteoplastic flap for defects >2 cm above floor & lateral to lamina papyracea Transnasal approach: External ethmoidectomy Transethmoidal sphenoidectomy Transseptal sphenoidotomy Transantral approach- Caldwell- Luc procedure 21
- 22. Endoscopic technique: Most widely used General concepts: Decongestion to maximize visualization (1:1000 epinephrine or 4% cocaine solution) Specific endoscopic approach: Designed to gain access to the area of interest in most efficient fashion Approaches: Transfrontal Transcribriform Transplanum Transsellar Transclival Transpterygoid 22
- 23. FOLLOW UP Non absorbable packing: removed on day 7-10 of operation Regular endoscopic examination & minimal debridement of surgical site to r/o recurrence of encephalocele/ CSF leak Close f/u in raised ICP Acetazolamide use: Close electrolyte monitoring Ventriculoperitoneal shunt if intolerable S/Es 23
- 24. COMPLICATIONS 1. Meningitis: most feared & severe i. Bacterial: S. pneumoniae, H. influenzae In first 3 weeks with trauma (10%) & non-trauma(40%) ii. Aseptic: Meningeal irritation due to manipulation during surgical repair 2. Anosmia OUTCOME & PROGNOSIS: Recurrence type Average time from repair Most leak 2 years Spontaneous leak 7 months Traumatic leak 4 months (50% in 2 weeks) 24
- 25. REFERENCES 1. Image-Based Case Studies in ENT and Head & Neck Surgery by Rahmat Omar & Prepageran Narayanan 2. Diseases of Ear, Nose & Throat by PL Dhingra & Shruti Dhingra 6th Edition 3. An illustrated text book Ear, Nose & Throat and Head & Neck Surgery by Rakesh Prasad Shrivastav 2nd Edition 25
- 26. THANK YOU 26
