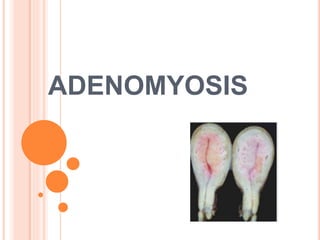
Adenomyosis
- 1. ADENOMYOSIS
- 2. Defination Etio_pathogenesis Clinical classification Symptoms and signs Diagnostic modalities Medical treatment Surgical treatment
- 3. INTRODUCTION: Rokitansky: first described the existence of ectopic endometrium in musculature of uterine wall in 1860 under the name adenomyoma. Von Recklinghausen in 1896: adenomyoma when extension is circumscribed lesion ,adenomyosis when extension is diffuse. Term adenomyosis …by Frankl in 1925
- 4. Defination by BIRD (1972): Benign invasion of endometrium into myometrium producing diffusely enlarged uterus,which microscopically exhibits ectopic,non- neoplastic,endometrial glands and stroma surrounded by hyperplastic and hypertrophic myometrium.
- 5. Some investigators define adenomyosis as presence of endometrial glands & stroma to depth of atleast one third of uterine wall thickness. GRADING OF ADENOMYOSIS : MOLITORS CRITERIA : According to depth of penetration : Grade I : inner 1/3 rd of myometrium. Grade II : middle 1/3 rd of myometrium. Grade III : outer 1/3 rd of myometrium. GRADING OF BIRD et al : Mild : 1-3 glands / LPF Moderate : 4-9 glands / LPF Severe : > 9 glands / LPF
- 6. PREVALENCE : 1% of all patients 5 – 8% to 40 – 70 % of all uterine specimens.(Azziz 1989). 8 – 62 % depending on criteria used for diagnosis & thoroughness with which excised uterine tissue is studied. ( Teeland). Souza et al detected discrete & diffuse pattern of adenomyosis in 54 % of young women with infertility,menorrhagia & dysmenorrhea
- 7. HISTOGENESIS: VON RECKLINGHAUSEN( 1896): Origin from mullerian duct . THOMAS S.CULLEN ( 1896): Most accepted theory Results from direct invasion or extension of basal endometrium into myometrium. It has been suggested that trauma of childbirth leads to breakdown of normal endo-myometrial border,subsequent reactive hyperplasia of basalis endometrium leads to an invasion of the myometrium & subsequent endometrium.
- 8. Endomyometrial trauma : Normal delivery Cesarean delivery MTP Myomectomy D&C Endometrial ablations. Uterine manipulations plays a crucial role in invasion of endometrial cell into myometrium. .. ref :
- 9. IVANOFF 1898: Adenomyosis occurs due to penetration of myometrium from serous coat after metaplasia. NEW HYPOTHESIS : Alteration of spiral arterioles angiogenesis has been put forward following the identification on MRI,of the JZ. The hypothesis postulates that ovulatory menstrual cycles during early reproductive life have an angiogenic priming effect that will permit successful deep penetration .
- 10. AGE: 30 and 45 years of age, RISK FACTORS Increasing parity Early menarche Short menstrual cycles. History of previous caesarean section , endometrial curettage or evacuation . Antidepressant drug use.(because of associated hyperprolactinemia) Tamoxifen …because of estrogen agonistic actionon endometrium
- 11. ASSOCIATED CONDITIONS : Leiomyoma ( 35 -55%) Pelvic endometriosis( 27-70%) Endometrial hyperplasia(7%) Endometrial carcinoma(1.4%) Endometrial polyps(2.3%) Association of adenomyosis with these conditions suggests a common underlying disorder like hyperestrogenemia.
- 12. PATHOLOGY : GROSS : uterus is uniformly enlarged in 60 – 80% cases. Asymetrically enlarged in focal adenomyosis. Usually does not exceed 12 -14 weeks. May exceed the size if associated fibroids. External surface :smooth ,regular. On palpation : uterus diffusely boggy or it may have nodular consistency. Serosa may have patchy pink colour suggesting hyperemia or congestion.
- 13. CUT SECTION : Myometrium shows diffuse hyperplasia. Posterior wall may be involved more. Trabecular or granular appearance on cut section Small ,dark cystic areas containing fluid or old blood ( burnt match stick appearance).
- 14. MICROSCOPY : Novak & Woodruff criteria: Presence of endometrial stroma and glands within myometrium, at least one high power field below basal endometrium. Bensen & Sneedens criteria : Presence of endometrial stroma and glands within myometrium, at least two low power field below basal endometrium.
- 15. Clinical classification : Diffuse adenomyosis : involving large portion of myometrium Focal adenomyosis : 1.Adenomyoma : restricted area of myometrium with clear border 2.Cystic adenomyosis (juvenile cystic adenomyosis) Age < 30 yrs ,cystic lesions < 1 cm,severe dysmenorrhea. Polypoid adenomyosis Endocervical adenomyosis Retroperitoneal adenomyosis. histologic spectrum of adenomyosis varies from solid to cystic.
- 16. Functional uterine zone: the junction between the endometrium and the inner myometrium It lacks a recognizable protective layer or membrane, a true submucosa. So endometrial glands lie in direct contact with the myometrium . Through MRI T2-weighted images, in the uterus of healthy women of reproductive age, three distinct layers can be displayed (i) the innermost zone with a high signal intensity, corresponding to the endometrial stripe; (ii) an intermediate inner low-signal-intensity area adjacent to the basal endometrium the JZ myometrium, or subendometrial layer, measuring 5 mm in thickness in healthy young women (iii) an outer medium-signal-intensity zone extending all the way to the serosal layer, or outer myometrium.
- 17. Cyclical changes in the thickness of the JZ maximum growth between days 8 and 16. In a more recent study by Hoad et al. (2005), the thickness of a normal JZ was found to be around 4 mm on average and can vary during the cycle by 0.9 mm on average Finally another recent MRI study did not find a significant difference in JZ thickness between the two phases of the menstrual cycle in 100 healthy women (Hauth et al., 2007). using MRI adenomyosis can be strongly suspected when the JZ thickness is 12 mm, although in approximately 20% of premenopausal women there is an absence of a definable JZ on imaging (Novellas et al., 2011). A diagnosis can be made even when thickness is <12 mm, if other signs (such as high-signal spots or an irregularly bounded JZ) are present (Reinhold et al., 1998)
- 18. SYMPTOMS : Most cases are asymptomatic (50 %). Ectopic glandular tissue tries to slough during menstruation ,however tissue & blood in ectopic glands cannot escape as there is no drainage. This trapping of blood & tissue causes dysmenorrhea. Dysmenorrhea (triple dysmenorrhea) ,congestive and spasmodic ,in premenstrual ,menstrual & post menstrual phases. ( 15-30%) AUB due to congestion. Premenstrual spotting. Dyspareunia in 20% cases due to associated endometriosis. Sub fertility Chronic pelvic pain ( 15-25 %)
- 19. Causes of sub fertility ? Impaired sperm transport: due to altered uterine peristaltic activity Impaired implantation : Implantation rate : JZ < 10mm - 45 % JZ 10- 12 mm -16% JZ >12mm - 5 % Impaired endometrial receptivity : Abnormal vascular proliferation Changes in endometrium :adverse molecular factors like VEGF. Changes in myometrium Gene dysregulation.
- 20. Altered decidualization Alteration in concentrations of intrauterine free radicals Altered implantation Altered gene regulation.
- 21. Uterine peristaltic activity : originates exclusively from the JZ, while the outer myometrium remains quiescent. During the follicular and periovulatory phases, contraction waves have a cervico-fundal orientation and their amplitude and frequency increase significantly towards the time of ovulation. Role of peristalitic waves : endometrial differentiation menstruation sperm transport implantation .
- 22. Subsequently, Kunz et al. (1996), using technetium labelled inert albumin microspheres placed in the cervix during late follicular phase, showed that myometrial contractions can quickly transport and preferentially direct these microspheres towards the tubal ostium on the side of the dominant follicle. Then, during the luteal phase, uterine activity decreases under the influence of progesterone and myometrial contraction waves become short and asymmetrical, often running in opposing directions. This reduced activity may help the blastocyst to implant near the fundus and perhaps facilitates local supply of nutrients and oxygen (Ijland et al., 1997).
- 23. In addition, in humans, interstitial and intravascular trophoblast invasion goes beyond the endometrium and involves the JZ, but not the outer myometrium Finally, MRI during a conception cycle shows, 7 days post-ovulation (a time coinciding with embryo implantation), focal disruption of the JZ signal intensity These physiological phenomena are altered in the presence of adenomyosis, and therefore it seems logical to assume that the condition may cause hypo- or infertility in affected women.
- 24. Signs: Uterus is typically diffusely enlarged Usually less than 14 weeks in size. Pv during menstruation :Uterus soft,boggy and tender ( Halbans sign),estrogens may also give same effect. Mobility not restricted.
- 25. ADENOMYOSIS & PREGNANCY : Pregnancy promotes invagination of basal endometrium into myometrium especially just after delivery . Adenomyosis is frequent finding in pregnancy but is rarerly associated with obstetric or surgical problems. Haydon suggested increased risk of uterine rupture,uterine atony & PPH.
- 26. Why uterine atony & PPH ? Atony of uterine muscle could be caused by decidual transformation of adenomyotic field, atrophy of muscle fascicles, edema of the stroma, mesenchymal transformation, and fibrosis. This leads to a decrease in myometrial contractions, and prolonged postpartal bleeding.
- 27. Rarely adenocarcinoma of uterus.
- 28. INVESTIGATIONS : USG HSG SSG Myometrial biopsy CA-125 MRI
- 30. ULTRASOUND Sonographic features of adenomyosis are variable and may be absent. The reported sensitivity and specificity of trans- abdominal ultrasound are 32-63% and 95-97% respectively 7. The spectrum of findings includes: Normal appearing uterus Focal or diffuse myometrial bulkiness, typically of the posterior wall . Thickening of the transition zone can sometimes be visualised as a hypoechoic halo surrounding the endometrial layer of ≥12 mm thickness
- 31. Normal uterus
- 38. Subendometrial echogenic linear striations Subendometrial echogenic nodules (specific sign) Small myometrial cysts / sub endometrial cysts (specific sign) Heterogeneous echogenicity (heterogenous myometrial echotexture) hyperechoic: islands of endometrial glands hypoechoic: associated muscle hypertrophy a "Venetian blind" appearance may be seen due to subendometrial echogenic linear striations and acoustic shadowing where endometrial tissues cause a hyperplastic reaction
- 39. HSG: Characteristic findings are multiple spicules 1 -4 mm extending from endometrium into myometrium & ending in small sacs. Honey coomb appearance in myometrium due to communication between endometrium & myometrium. Non specific as they can occur due to lymphatic & vascular extravasation also. Seen in 25% of cases only.
- 40. ROLE OF COLOUR DOPPLER : To differentiate Leiomyomas & Adenomyosis. Leiomyoma : Peripheral scattered feeding vessels or outer feeding vessels were noted. Adenomyosis : vessels traverse the hypertrophic myometrium between cystic spaces.
- 41. MRI : Accurate & superior to USG. Homogenous JZ thickness > 12mm with hemorrhagic high signal myometrial spots is highly predictive . On T2-weighted MRI, focal adenomyosis are seen in areas of abnormal low signal intensity within the myometrium in approximately 50% of patients. These foci correspond to islands of heterotopic endometrial tissue, cystic dilatation of heterotopic glands, or hemorrhagic foci. On T2-weighted MRI, diffuse adenomyosis usually manifested as diffuse thickening of the junctional zone with homogeneous low signal intensity . T2-weighted imaging provided significantly better lesion detection than unenhanced or contrast material–enhanced T1-weighted imaging
- 43. Classification for adenomyosis based on MRI uterine JZ: (i) simple JZ hyperplasia (zone thickness 8 mm but <12 mm on T2-weighted images, in women aged 35 years or less); (ii) partial or diffuse adenomyosis (thickness 12 mm; high-signal-intensity myometrial foci; involvement of the outer myometrium: <1/3, <2/3, >2/3); and (iii) adenomyoma (myometrial mass with indistinct margins of primarily low-signal intensit on all MRI sequences).
- 44. MYOMETRIAL BIOPSY LAPAROSCOPICALLY OR SONOGRAPHICALLY GUIDED: Larger study by Popp et al. In that study biopsies are taken immediately at the time of laparoscopy as well as transvaginally under ultrasound guidance . A single myometrial biopsy picked up only 8% to 19% of women with adenomyosis. The sensitivity of random needle biopsy is therefore too low for clinical practice. CA 125 : Raised but not specific.
- 45. MANAGEMENT : Conservative treatment Medical treatment Hysterectomy Uterine sparing procedures.
- 46. CONSERVATIVE MANAGEMENT : For young symptomtomatic patient. Observation & NSAIDS. MEDICAL MANAGEMENT : Progestins OCPills. Estrogen receptors are more consistently present than progesterone receptors.( absent in 50% of cases ) They are of little aid in treatment. However low dose OCPills can be used for menorrhagia & dysmenorrhea.
- 47. GnRH agonist : leuprolide acetate 3.75 mg/IM/month for 6 months. 0.5 mg daily SC for 6 months. Recurrence is common after discontinuation of treatment. Pre & post operative use of GnRH agonist therapy : Role of combination approach..not clear Hypothesized to have synergistic effect. Response of remaining adenomyotic tissue to GnRH enhanced after surgery. Advantages of pre- op use : reduction of uterine vascularity correction of anemia reductionof intraoperative bleeding.
- 48. Disadvantages of pre-op use : recognition of adenomyotic tissue is difficult dermarcation of adenomyosis & normal myometrium difficult risk of endometrial perforation increased removing large amount of adenomyomotic tissue difficult. LNG IUS : Growing evidence indicates its use for menorrhagia & dysmenorrhea. Danazol: Loaded 300-400 mg IUD
- 49. Based on these results, the researchers concluded that: Among patients resistant to oral danazol therapy and nasal GnRH agonist therapy, a danazol-loaded IUD treatment can be very effective and is much more conservative than a hysterectomy The subjective and objective signs and symptoms of adenomyoma were reduced or eliminated in the majority of participants in a minimal amount of time Conception can occur after removal of the IUD Systemic side effects do not occur because the danazol remains concentrated in the uterine area
- 50. In view of the accumulating evidence that endometriosis is an epigenetic disease our encouraging pilot results on the off-label use of VPA for treatment of adenomyosis should be greeted with guarded enthusiasm. Obviously, whether VPA or other HDACIs may be truly efficacious in treating adenomyosis and/or endometriosis should await future controlled randomized clinical trials that have optimal treatment duration, sufficient sample sizes, and more objective quantification. If proven efficacious, VPA may be a much cheaper alternative to GnRH agonist therapy, and possibly more efficacious and potent as a result of its potential to rectify epigenetic aberrations, yet with fewer and milder side effects.
- 51. Conservative surgery has not become the standard treatment for adenomyosis ? This is mainly because adenomyotic tissue invades the uterine muscle layer in a way that make the borders of the lesion unclear, so complete excision of the affected area remains inaccurate . Moreover, the excision of adenomyotic tissue is always accompanied by excision of myometrium, so it is partly destructive for the uterine wall: Advantages of removing an affected area must be balanced against disadvantages of leaving a possibly defective uterine wall. Hence, there is a recognized difficulty in establishing the state-of-art of conservative surgical technique for uterine-sparing management of adenomyosis,& operative options include nonstandardized cytoreductive approaches .
- 53. UTERUS SPARING METHODS: Complete excision of adenomyosis. Adenomyomectomy. Preferably used in cases of localized adenomyosis (adenomyoma) Selected cases of diffuse adenomyosis with reconstruction of the uterine wall. This includes the complete removal of all clinically recognizable non-microscopic lesions. The integrity of uterine wall is maintained
- 54. CLASSIC TECHNIQUE: Open or laparotomy. Recognition of lesion location by inspection /palpation Longitudinal incision of uterine wall along adenomyoma. Sharp & blunt dissection of lesion . Suturing of uterine wall in one/two /more seromuscular layers Suturing of endometrial cavity if necessary USG can be used if required.
- 55. U SHAPED WALL SUTURING : after excision of adenomyoma cave like wound is approximated by U shape sutures at muscle layer. Seromuscular layer by figure of eight sutures OVER LAPPING FLAP METHOD : Transverse incision Excision of lesion with monopolar needle Seromuscular layers re overlapped & sutured to counteract the lost muscle layer of uterus.
- 56. TRIPLE-FLAP METHOD:(OSADA et al) Laparotomy technique. Bisection of uterus in midline & in sagittal plane with scalpel until uterine cavity is reached. Opening of endometrial cavity to permit introduction of index finger to guide during excision. Myometrial thickness of 1cm from serosa above & endometrium below is left Closure of flaps of endometrium with 3-0 vicryl Closure of flaps of uterine wall Approximating myometrium & serosa of one side of bisected uterus in AP plane with interuppted 2-0 vicryl While C/L side is brought over reconstructed first side in such away to cover it.
- 58. RESULTS : In 9 studies,469 patients Mean age …37.5 years Mean follow up..25 months Reduction of pain…82% Reduction of bleeding..68% In Studies where fertility preservaion was main…341 patients : Pregnancy rate :60.5 % Delivery rate :83.1 %
- 59. Cystectomy: Used in cases of cystic focal adenomyosis, including the entire removal of the adenomyotic cyst Cytoreductive surgery/partial adenomyomectomy: Done in diffuse adenomyosis, the partial removal of the clinically recognizable non- microscopic lesions because complete removal of the lesion would lead to the concomitant excision of critical amount of healthy myometrium, which could lead to ‘‘functional’’ hysterectomy. Laparoscopically assisted vaginal excision can also be done.
- 60. PREGNANCY ISSUES : INTERVENTION TO CONCEPTION TIME : At least 3 months after conception . IMPLICATIONS TO ART METHODS : ART increased pregnancy rates after operative intervention when compared to natural cycles. Single embryo transfer .
- 61. Complications : Uterine rupture Wang etal…1 in 8 after cyto reductive surgery Atonic PPH
- 62. NON EXCISIONAL TECHNIQUES : UAE : Success rate 25 -90% Minimally invasive angiographic interventional procedure which delivers embolic materials into both uterine arteries & leads to ischemia & necrosis of adenomyotic tissue. PVA pellets of 500-710 um or triacryl gelatin microspheres are used. Procedure : Done by interventional radiologist. SA/EA Under digital flouroscopic control Via femoral artery ,percutaneous catheter is passed to IIA & then passed to UA.Embolic materials are then injected. Procedure is repeated on other side. Duration : 45-60 min.
- 64. procedure dysmenorrhea menorrhagia Conception rate Delivery rate Complete excision 82 % 66 % 60% 83% cystectomy 86 % 84% Partial excision 81 % 50% 46% 73% Non excisional method 54 % 73% 55% 50%