IVMS-CV Pharmacology -Diuretic Agents
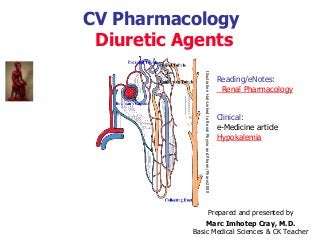
- 1. CV Pharmacology Diuretic Agents Reading/eNotes: Renal Pharmacology Clinical: e-Medicine article Hypokalemia IllustrationHot-LinkedtoRenalPhysioandPharm/Pharm2000 Prepared and presented by Marc Imhotep Cray, M.D. Basic Medical Sciences & CK Teacher
- 2. 2 Illustration shows where some types of diuretics act, and how
- 3. 3 Diuretic Agents Drugs that accelerate the rate of urine formation Result: removal of sodium and water
- 4. 4 Sodium As goes sodium so goes water 20 to 25% of all sodium is reabsorbed into the bloodstream in the loop of Henle 5 to 10% in the distal tubules, 3% in collecting ducts If not absorbed, it is excreted with the urine
- 5. 5 Diuretic Agents 1. Carbonic anhydrase inhibitors 2. Loop diuretics 3. Osmotic diuretics 4. Potassium-sparing diuretics 5. Thiazide and thiazide-like diuretics
- 6. 6 Carbonic Anhydrase Inhibitors (CAIs) 1. acetazolamide (Diamox) 2. methazolamide 3. Dichlorphenamide MOA: these agents block formation of H+ and HCO3- from CO2 and H2O. The end result is that bicarbonate is excreted in the urine. (see notes page for more)
- 7. 7 Carbonic Anhydrase Inhibitors: Mechanism of Action The enzyme carbonic anhydrase helps to make H+ ions available for exchange with sodium and water in the proximal tubules CAIs block the action of carbonic anhydrase, thus preventing the exchange of H+ ions with sodium and water
- 8. 8 Inhibition of carbonic anhydrase reduces H+ ion concentration in renal tubules As a result, there is increased excretion of bicarbonate, sodium, water, and potassium Reabsorption of water is decreased and urine volume is increased Carbonic Anhydrase Inhibitors: Mechanism of Action
- 9. 9 Carbonic Anhydrase Inhibitors: Therapeutic Uses Adjunct agents in the long-term management of open-angle glaucoma Used with miotics to lower intraocular pressure before ocular surgery in certain cases Also useful in the treatment of: Glaucoma Edema Epilepsy High-altitude sickness
- 10. 10 Acetazolamide is used in the management of edema secondary to CHF when other diuretics are not effective CAIs are less potent diuretics than loop diuretics or thiazides—metabolic acidosis they induce reduces their diuretic effect in 2 to 4 days Carbonic Anhydrase Inhibitors: Therapeutic Uses
- 11. 11 Carbonic Anhydrase Inhibitors: Side Effects hyperchloremic metabolic acidosis Drowsiness Anorexia Paresthesias Hematuria Urticaria Photosensitivity Melena
- 12. 12 Loop Diuretics bumetanide (Bumex) ethacrynic acid (Edecrin) furosemide (Lasix)
- 13. 13 Loop Diuretics: Mechanism of Action Act directly on the ascending limb of the loop of Henle to inhibit sodium and chloride reabsorption Increase renal prostaglandins, resulting in the dilation of blood vessels and reduced peripheral vascular resistance
- 14. 14 Loop Diuretics: Drug Effects Potent diuresis and subsequent loss of fluid Decreased fluid volume causes: Reduced BP Reduced pulmonary vascular resistance Reduced systemic vascular resistance Reduced central venous pressure Reduced left ventricular end-diastolic pressure Potassium depletion
- 15. 15 Loop Diuretics: Therapeutic Uses Edema associated with CHF or hepatic or renal disease Control of hypertension
- 16. 16 Loop Diuretics: Side Effects Body System Effect CNS Dizziness headache tinnitus blurred vision GI Nausea/vomiting, diarrhea
- 17. 17 Loop Diuretics: Side Effects Body System Effect Hematologic Agranulocytosis, neutropenia, thrombocytopenia Metabolic Hypokalemia, hyperglycemia, hyperuricemia
- 18. 18 Osmotic Diuretics mannitol (Resectisol, Osmitrol)
- 19. 19 Osmotic Diuretics: Mechanism of Action Work in the proximal tubule Nonabsorbable, producing an osmotic effect Pull water into the blood vessels and nephrons from the surrounding tissues
- 20. 20 Osmotic Diuretics: Drug Effects Reduced cellular edema Increased urine production, causing diuresis Rapid excretion of water, sodium, and other electrolytes, as well as excretion of toxic substances from the kidney Reduces excessive intraocular pressure
- 21. 21 Osmotic Diuretics: Therapeutic Uses Used in the treatment of patients in the early, oliguric phase of ARF To promote the excretion of toxic substances Reduction of intracranial pressure Treatment of cerebral edema
- 22. 22 Osmotic Diuretics: Side Effects Convulsions Thrombophlebitis Pulmonary congestion Also headaches, chest pains, tachycardia, blurred vision, chills, and fever
- 23. 23 Potassium-Sparing Diuretics Do not share any obvious chemical similarities, except for steroid-structure, of the aldosterone antagonists Those in clinical use include: Epithelial sodium channel blockers: Amiloride Triamterene Aldosterone antagonists: Spironolactone Eplerenone
- 24. 24 Potassium-Sparing Diuretics: Mechanism of Action Work in collecting ducts and distal convoluted tubules Interfere with sodium-potassium exchange Competitively bind to aldosterone receptors Block the reabsorption of sodium and water usually induced by aldosterone
- 25. 25 Potassium-Sparing Diuretics: Drug Effects Prevent potassium from being pumped into tubule, thus preventing its secretion Competitively block aldosterone receptors and inhibit its action Excretion of sodium and water is promoted
- 26. 26 Potassium-Sparing Diuretics: Therapeutic Uses spironolactone and triamterene Hyperaldosteronism Hypertension Reversing potassium loss caused by potassium-losing drugs amiloride Treatment of CHF
- 27. 27 Potassium-Sparing Diuretics: Side Effects Body System Effect CNS Dizziness, headache GI Cramps, nausea, vomiting, diarrhea Other Urinary frequency, weakness **hyperkalemia
- 28. 28 Potassium-Sparing Diuretics: Side Effects spironolactone gynecomastia, amenorrhea, irregular menses
- 29. 29 Thiazide and Thiazide-Like Diuretics hydrochlorothiazide (Esidrix, HydroDIURIL) chlorothiazide (Diuril) trichlormethiazide (Metahydrin) chlorthalidone (Hygroton) metolazone (Mykrox, Zaroxolyn)
- 30. 30 Thiazide and Thiazide-Like Diuretics: Mechanism of Action Inhibit tubular resorption of sodium and chloride ions Action primarily in the ascending loop of Henle and early distal tubule Result: water, sodium, and chloride are excreted Potassium is also excreted to a lesser extent Dilate the arterioles by direct relaxation
- 31. 31 Thiazide and Thiazide-Like Diuretics: Drug Effects Lowered peripheral vascular resistance Depletion of sodium and water
- 32. 32 Thiazide and Thiazide-Like Diuretics: Therapeutic Uses Hypertension (one of most prescribed group of agents) Edematous states Idiopathic hypercalciuria Diabetes insipidus Adjunct agents in treatment of CHF, hepatic cirrhosis
- 33. 33 Thiazide and Thiazide-Like Diuretics: Side Effects Body System Effect CNS Dizziness, headache, blurred vision, paresthesias, decreased libido GI Anorexia, nausea, vomiting, diarrhea
- 34. 34 Thiazide and Thiazide-Like Diuretics: Side Effects Body System Effect GU Impotence Integumentary Urticaria, photosensitivity Metabolic Hypokalemia, glycosuria, hyperglycemia
- 35. 35 Additional Resources Drug Monitor - Diuretics Diagram at cvpharmacology.com Renal Physiology And Disease
