Chronic bronchitis
•Download as DOC, PDF•
4 likes•5,053 views
COPD
Report
Share
Report
Share
Recommended
More Related Content
What's hot
What's hot (20)
Viewers also liked
Viewers also liked (20)
Chronic obstructive pulmonary disease (copd) power point

Chronic obstructive pulmonary disease (copd) power point
COPD (Chronic obstructive Pulmonary Disease) PowerPoint Presentation -aslam

COPD (Chronic obstructive Pulmonary Disease) PowerPoint Presentation -aslam
Similar to Chronic bronchitis
Similar to Chronic bronchitis (20)
COPD(Chronic Obstructive Pulmonary Disease)Ayurveda

COPD(Chronic Obstructive Pulmonary Disease)Ayurveda
Bronchitis afpa rdmc_06_dr meghanaben mehta_20180422

Bronchitis afpa rdmc_06_dr meghanaben mehta_20180422
Acute and Chronic Bronchitis and Homeopathy treatment 

Acute and Chronic Bronchitis and Homeopathy treatment
Chronic obstructive pulmonary disease, or COPD, refers to a group of diseases...

Chronic obstructive pulmonary disease, or COPD, refers to a group of diseases...
More from Arsenic Halcyon
More from Arsenic Halcyon (20)
Хөнгөвчилөх эмчилгээний өвчтөн хоолонд дургуй болох

Хөнгөвчилөх эмчилгээний өвчтөн хоолонд дургуй болох
Recently uploaded
Ahmedabad Call Girls Book Now 9630942363 Top Class Ahmedabad Escort Service Available
9630942363 Ahmedabad Escort Service Ahmedabad Call Girls Ahmedabad Escorts Service Ahmedabad Call Girl Russian 9630942363 Russian Ahmedabad Escort Service Vip Ahmedabad Escort Service Ahmedabad Call Girls Housewife Model College Girls Aunty Bhabhi Ahmedabad 9630942363 Genuine Ahmedabad Call Girl Escort ServiceAhmedabad Call Girls Book Now 9630942363 Top Class Ahmedabad Escort Service A...

Ahmedabad Call Girls Book Now 9630942363 Top Class Ahmedabad Escort Service A...GENUINE ESCORT AGENCY
PEMESANAN OBAT ASLI : +6287776558899
Cara Menggugurkan Kandungan usia 1 , 2 , bulan - obat penggugur janin - cara aborsi kandungan - obat penggugur kandungan 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 bulan - bagaimana cara menggugurkan kandungan - tips Cara aborsi kandungan - trik Cara menggugurkan janin - Cara aman bagi ibu menyusui menggugurkan kandungan - klinik apotek jual obat penggugur kandungan - jamu PENGGUGUR KANDUNGAN - WAJIB TAU CARA ABORSI JANIN - GUGURKAN KANDUNGAN AMAN TANPA KURET - CARA Menggugurkan Kandungan tanpa efek samping - rekomendasi dokter obat herbal penggugur kandungan - ABORSI JANIN - aborsi kandungan - jamu herbal Penggugur kandungan - cara Menggugurkan Kandungan yang cacat - tata cara Menggugurkan Kandungan - obat penggugur kandungan di apotik kimia Farma - obat telat datang bulan - obat penggugur kandungan tuntas - obat penggugur kandungan alami - klinik aborsi janin gugurkan kandungan - ©Cytotec ™misoprostol BPOM - OBAT PENGGUGUR KANDUNGAN ®CYTOTEC - aborsi janin dengan pil ©Cytotec - ®Cytotec misoprostol® BPOM 100% - penjual obat penggugur kandungan asli - klinik jual obat aborsi janin - obat penggugur kandungan di klinik k-24 || obat penggugur ™Cytotec di apotek umum || ®CYTOTEC ASLI || obat ©Cytotec yang asli 200mcg || obat penggugur ASLI || pil Cytotec© tablet || cara gugurin kandungan || jual ®Cytotec 200mcg || dokter gugurkan kandungan || cara menggugurkan kandungan dengan cepat selesai dalam 24 jam secara alami buah buahan || usia kandungan 1_2 3_4 5_6 7_8 bulan masih bisa di gugurkan || obat penggugur kandungan ®cytotec dan gastrul || cara gugurkan pembuahan janin secara alami dan cepat || gugurkan kandungan || gugurin janin || cara Menggugurkan janin di luar nikah || contoh aborsi janin yang benar || contoh obat penggugur kandungan asli || contoh cara Menggugurkan Kandungan yang benar || telat haid || obat telat haid || Cara Alami gugurkan kehamilan || obat telat menstruasi || cara Menggugurkan janin anak haram || cara aborsi menggugurkan janin yang tidak berkembang || gugurkan kandungan dengan obat ©Cytotec || obat penggugur kandungan ™Cytotec 100% original || HARGA obat penggugur kandungan || obat telat haid 1 bulan || obat telat menstruasi 1-2 3-4 5-6 7-8 BULAN || obat telat datang bulan || cara Menggugurkan janin 1 bulan || cara Menggugurkan Kandungan yang masih 2 bulan || cara Menggugurkan Kandungan yang masih hitungan Minggu || cara Menggugurkan Kandungan yang masih usia 3 bulan || cara Menggugurkan usia kandungan 4 bulan || cara Menggugurkan janin usia 5 bulan || cara Menggugurkan kehamilan 6 Bulan
________&&&_________&&&_____________&&&_________&&&&____________
Cara Menggugurkan Kandungan Usia Janin 1 | 7 | 8 Bulan Dengan Cepat Dalam Hitungan Jam Secara Alami, Kami Siap Meneriman Pesanan Ke Seluruh Indonesia, Melputi: Ambon, Banda Aceh, Bandung, Banjarbaru, Batam, Bau-Bau, Bengkulu, Binjai, Blitar, Bontang, Cilegon, Cirebon, Depok, Gorontalo, Jakarta, Jayapura, Kendari, Kota Mobagu, Kupang, LhokseumaweCara Menggugurkan Kandungan Dengan Cepat Selesai Dalam 24 Jam Secara Alami Bu...

Cara Menggugurkan Kandungan Dengan Cepat Selesai Dalam 24 Jam Secara Alami Bu...Cara Menggugurkan Kandungan 087776558899
Recently uploaded (20)
Dehradun Call Girl Service ❤️🍑 8854095900 👄🫦Independent Escort Service Dehradun

Dehradun Call Girl Service ❤️🍑 8854095900 👄🫦Independent Escort Service Dehradun
Race Course Road } Book Call Girls in Bangalore | Whatsapp No 6378878445 VIP ...

Race Course Road } Book Call Girls in Bangalore | Whatsapp No 6378878445 VIP ...
❤️Amritsar Escorts Service☎️9815674956☎️ Call Girl service in Amritsar☎️ Amri...

❤️Amritsar Escorts Service☎️9815674956☎️ Call Girl service in Amritsar☎️ Amri...
Call Girls Mussoorie Just Call 8854095900 Top Class Call Girl Service Available

Call Girls Mussoorie Just Call 8854095900 Top Class Call Girl Service Available
Most Beautiful Call Girl in Chennai 7427069034 Contact on WhatsApp

Most Beautiful Call Girl in Chennai 7427069034 Contact on WhatsApp
Bhawanipatna Call Girls 📞9332606886 Call Girls in Bhawanipatna Escorts servic...

Bhawanipatna Call Girls 📞9332606886 Call Girls in Bhawanipatna Escorts servic...
Cardiac Output, Venous Return, and Their Regulation

Cardiac Output, Venous Return, and Their Regulation
Bandra East [ best call girls in Mumbai Get 50% Off On VIP Escorts Service 90...

Bandra East [ best call girls in Mumbai Get 50% Off On VIP Escorts Service 90...
Ahmedabad Call Girls Book Now 9630942363 Top Class Ahmedabad Escort Service A...

Ahmedabad Call Girls Book Now 9630942363 Top Class Ahmedabad Escort Service A...
Chandigarh Call Girls Service ❤️🍑 9809698092 👄🫦Independent Escort Service Cha...

Chandigarh Call Girls Service ❤️🍑 9809698092 👄🫦Independent Escort Service Cha...
Cara Menggugurkan Kandungan Dengan Cepat Selesai Dalam 24 Jam Secara Alami Bu...

Cara Menggugurkan Kandungan Dengan Cepat Selesai Dalam 24 Jam Secara Alami Bu...
VIP Hyderabad Call Girls KPHB 7877925207 ₹5000 To 25K With AC Room 💚😋

VIP Hyderabad Call Girls KPHB 7877925207 ₹5000 To 25K With AC Room 💚😋
Call Girls Bangalore - 450+ Call Girl Cash Payment 💯Call Us 🔝 6378878445 🔝 💃 ...

Call Girls Bangalore - 450+ Call Girl Cash Payment 💯Call Us 🔝 6378878445 🔝 💃 ...
Pune Call Girl Service 📞9xx000xx09📞Just Call Divya📲 Call Girl In Pune No💰Adva...

Pune Call Girl Service 📞9xx000xx09📞Just Call Divya📲 Call Girl In Pune No💰Adva...
💚Chandigarh Call Girls 💯Riya 📲🔝8868886958🔝Call Girls In Chandigarh No💰Advance...

💚Chandigarh Call Girls 💯Riya 📲🔝8868886958🔝Call Girls In Chandigarh No💰Advance...
Jaipur Call Girl Service 📞9xx000xx09📞Just Call Divya📲 Call Girl In Jaipur No💰...

Jaipur Call Girl Service 📞9xx000xx09📞Just Call Divya📲 Call Girl In Jaipur No💰...
Kolkata Call Girls Shobhabazar 💯Call Us 🔝 8005736733 🔝 💃 Top Class Call Gir...

Kolkata Call Girls Shobhabazar 💯Call Us 🔝 8005736733 🔝 💃 Top Class Call Gir...
💚Chandigarh Call Girls Service 💯Piya 📲🔝8868886958🔝Call Girls In Chandigarh No...

💚Chandigarh Call Girls Service 💯Piya 📲🔝8868886958🔝Call Girls In Chandigarh No...
Chronic bronchitis
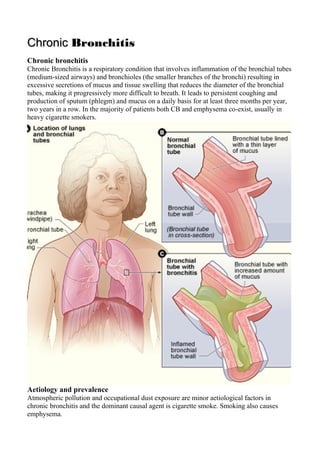
- 1. CChhrroonniicc Bronchitis Chronic bronchitis Chronic Bronchitis is a respiratory condition that involves inflammation of the bronchial tubes (medium-sized airways) and bronchioles (the smaller branches of the bronchi) resulting in excessive secretions of mucus and tissue swelling that reduces the diameter of the bronchial tubes, making it progressively more difficult to breath. It leads to persistent coughing and production of sputum (phlegm) and mucus on a daily basis for at least three months per year, two years in a row. In the majority of patients both CB and emphysema co-exist, usually in heavy cigarette smokers. Aetiology and prevalence Atmospheric pollution and occupational dust exposure are minor aetiological factors in chronic bronchitis and the dominant causal agent is cigarette smoke. Smoking also causes emphysema.
- 2. Mechanism of airflow obstruction In chronic bronchitis the fundamental cause of reduced ventilatory capacity and breathlessness is the limitation of expiratory airflow. The disease is caused by an interaction between noxious inhaled agents and host factors, such as genetic predisposition or respiratory infections which cause injury or irritation to the respiratory epithelium of the walls and lumen of the bronchi and bronchioles. Chronic inflammation, edema, temporary bronchospasm, and increased production of mucus by goblet cells are the result. As a consequence, airflow into and out of the lungs is reduced, sometimes to a dramatic degree.
- 3. Clinical features Chronic bronchitis develops over many years and patients are rarely symptomatic before middle age. Symptoms are initially minor, perhaps a morning cough productive of a little sputum. The sputum may be clear, yellowish, or greenish depending on bacterial infection, and sometimes tinged with blood if small blood vessels are ruptured due to constant coughing. Initially breathlessness is on exertion but exercise capacity progressively and slowly deteriorates and eventually patients become respiratory cripples distressed even at rest. Patients with predominant bronchitis are prone to periodic infections. Eventually patients with chronic bronchitis develop severe hypoxia and other complications.
- 4. CChhrroonniicc BBrroonncchhiittiiss Management Restoration of normal function is not possible in chronic bronchitis. The aim of therapy must therefore be to reduce disability by tackling the interrelated problems of airways obstruction, recurrent infections, breathlessness, hypoxia and poor exercise tolerance. Factors aggravating chronic bronchitis, particularly cigarette smoking, must be withdrawn. Oxygen therapy During acute exacerbation of chronic bronchitis, O2 therapy is necessary to avoid death from hypoxia. Studies suggest that long-term controlled O2 therapy can benefit patients with severe airways obstruction who have severe hypoxia and who refrain from smoking cigarettes. It is necessary to administer O2 virtually continuously, including during sleep. The administration of continuous O2 presents considerable practical and financial difficulties. Cessation of cigarette smoking Tobacco smoke damages the bronchial tree and produces airflow limitation by a number of different actions. Smoke impairs mucociliary clearance and causes bronchial smooth muscle to contract by stimulating receptors and provoking the release of inflammatory mediators. In addition, smoke increases mucus production and causes mucous gland hypertrophy. Smokers are predisposed to bronchial infection and consequent inflammation. It is therefore not surprising that chronic bronchitis and emphysema are found in 15% of middle-aged males who smoke moderately or heavily but are rare in non-smokers, and that deaths from bronchitis increase with the amount smoked. If patients with chronic bronchitis and emphysema stop smoking, the rate of decline in pulmonary function is reduced to that of non-smokers. If patients stop smoking early in their disease there is improvement in pulmonary function. Diagnosing Chronic Bronchitis Physicians diagnose chronic bronchitis by using a combination of medical history, physical exam, and diagnostic tests. A history of a daily cough that lasts at least three months, especially if has occurred two years in a row, fits the criteria for a clinical diagnosis of chronic bronchitis. A history of smoking and/or working with noxious chemicals is also very relevant. The physical examination usually includes listening for wheezing, determining if there is a prolongation of exhalation, and looking for evidence of cyanosis, which are all signs of airflow obstruction. A sputum sample showing neutrophil granulocytes (inflammatory white blood cells) and a positive culture for pathogenic microorganisms such as Streptococcal species are also indications that the patient might have chronic bronchitis. However, for expectorated sputum samples to be considered valid, conventional wisdom is that there should be fewer than 10 squamous cells and more than 25 white blood cells per high-power microscopic field. A chest X-ray is often taken if bronchitis is suspected to help rule out other lung conditions such as pneumonia, tuberculosis, or bronchial obstructions.
