On the Move: The Challenges of Providing Routine Immunization Services to Nomadic Populations in Ethiopia
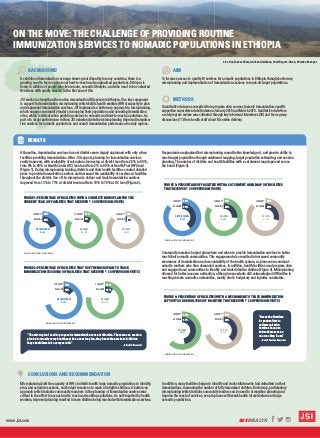
- 1. @JSIHEALTHwww.jsi.com ON THE MOVE: THE CHALLENGE OF PROVIDING ROUTINE IMMUNIZATION SERVICES TO NOMADIC POPULATIONS IN ETHIOPIA Lisa Oot, Zenaw Adam, Adriana Almiñana, Quail Rogers-Bloch, Natasha Kanagat 2% 90% At baseline, immunization services in most districts were largely unplanned with only a few facilities providing immunizations. After JSI support, planning for immunization services vastly improved, with availability of microplans increasing at district level from 20% to 89%, from 9% to 86% at Health Center (HC) level and from 2% to 90% at Health Post (HP) level (Figure 1). During microplanning training, districts and their health facilities created detailed plans to provide immunization services and increased the availability of services at facilities throughout the district. Use of the microplan to deliver and track immunization services improved from 13% to 71% at district level and from 10% to 78% at HC level (Figure 2). Respondents emphasized that microplanning meant better knowledge of, and greater ability to reach target populations through catchment mapping, target population estimating, and session planning. The number of districts and health facilities with a catchment map improved across the board (Figure 3). To increase access to quality RI services for nomadic populations in Ethiopia through bottom-up microplanning and implementation of immunization sessions to reach all target populations. “The micro-plan I used to prepare for immunization was not effective. There was no session plan but currently every health post has a session plan, they know the number of children they should immunize every month.” – District Office staff “It was the first time for pastoralists to get immunization services because before there was no one reaching them.” – Health Post health worker Quantitative data was compiled from program data sources (namely immunization-specific supportive supervision data) between January 2015 and March 2018. Qualitative data from a mid-program review was collected through key informant interviews (36) and focus group discussions (11) from health staff about RI service delivery. As childhood immunization coverage shows great disparity in many countries, there is a growing need to focus on the most hard-to-reach and marginalized populations. Ethiopia is home to millions of people who live remote, nomadic lifestyles, and who need to be contacted five times with quality vaccine in the first year of life. JSI works to strengthen the routine immunization (RI) system in Ethiopia. One key component is support for immunization microplanning which builds health workers (HWs) capacity to plan and implement immunization services. JSI implements a bottom-up approach to microplanning, which engages community leaders in mapping their populations and selecting immunization sites, which is critical when providing services to nomadic and hard-to-reach populations. As part of a larger performance review, JSI examined whether microplanning improved immuniza- tion services for nomadic populations and overall immunization performance in study regions. Microplanning built the capacity of HWs in districts with large nomadic populations to identify, plan, and schedule sessions, and budget resources to reach all eligible children. A bottom-up approach which includes community members in the planning of immunization services was critical in the effort to access hard to reach and mobile populations. As self-reported by health workers, improved planning resulted in more children being reached with immunization services. RESULTS In addition, many facilities began to identify and track children who had defaulted on their immunizations, increasing the number of fully immunized children. Bottom-up, participatory microplanning which includes community leaders can be used to strengthen planning and improve the reach of services, even in places with weak health infrastructure and large nomadic populations. DISTRICT LEVEL N = 45 FIGURE 1: PERCENTAGE OF FACILITIES WITH A COMPLETE MICROPLAN FOR THE CURRENT YEAR (OF FACILITIES THAT RECEIVED > 3 SUPERVISION VISITS) HC LEVEL N = 58 HP LEVEL N = 62 9% 86% 20% 89% 90% DISTRICT LEVEL N = 45 FIGURE 3: PERCENTAGE OF FACILITIES WITH A CATCHMENT AREA MAP (OF FACILITIES THAT RECEIVED > 3 SUPERVISION VISITS) HC LEVEL N = 58 HP LEVEL N = 62 26% 86% 40% 89% FIGURE 2: PERCENTAGE OF FACILITIES THAT USE THE MICROPLAN TO TRACK IMMUNIZATION SESSIONS (OF FACILITIES THAT RECEIVED > 3 SUPERVISION VISITS) DISTRICT LEVEL N = 45 HC LEVEL N = 58 10% 78% 13% 71% FIGURE 4: PERCENTAGE OF FACILITIES WITH A MECHANISM TO TRACK IMMUNIZATION LEFT-OUTS OR DEFAULTERS (OF FACILITIES THAT RECEIVED > 3 SUPERVISION VISITS) DISTRICT LEVEL N = 45 HC LEVEL N = 58 39% 71% 47% Community members helped plan where and when to provide immunization services to better reach their nomadic communities. This engagement also resulted in increased community awareness of immunization and accountability of the health system, as plans were communi- cated to mothers who then demanded services. In addition, health facilities used program data and engaged local communities to identify and track defaulter children (Figure 4). Microplanning allowed for better resource estimation, although respondents still acknowledged difficulties in reaching remote nomadic communities, mainly due to budgetary and logistics constraints. 62% 29% HC LEVEL N = 58 HP LEVEL N = 62 39% 71% 47% 62% BACKGROUND AIM METHODS CONCLUSIONS AND RECOMMENDATION CURRENT* CURRENT* BASELINE BASELINE CURRENT* BASELINE CURRENT* BASELINE CURRENT* BASELINE CURRENT* BASELINE CURRENT* BASELINE CURRENT* BASELINE CURRENT* BASELINE CURRENT* BASELINE *CURRENT = MOST RECENT SUPERVISION VISIT *CURRENT = MOST RECENT SUPERVISION VISIT *CURRENT = MOST RECENT SUPERVISION VISIT *CURRENT = MOST RECENT SUPERVISION VISIT
