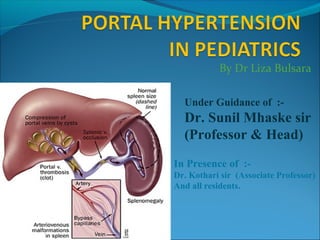
Portal hypertension paediatrics
- 1. By Dr Liza Bulsara Under Guidance of :- Dr. Sunil Mhaske sir (Professor & Head) In Presence of :- Dr. Kothari sir (Associate Professor) And all residents.
- 2. smalathi 2 S.GL.G Portal venous System
- 3. Portal Hypertension Normal range of portal venous pressure is 5 to 10 mm of Hg or 10-15 cm saline above the pressure present in the IVC. Portal hypertension is defined as elevation of this pressure gradient to values above 10 to 12 mm Hg. smalathi 3
- 4. Portal Hypertension Definition:PHT is a pathologic increase in portal pressure in which the pressure gradient between the portal vein and the IVC (Portal pressure gradient or PPG)is increased above the upper limit of 10 mm of Hg. PPG > 10 mmHg(varices) PPG > 12mmHg(variceal bleed,ascites) PPG > 6 to 10 mmHg(subclinical PHT) smalathi 4
- 5. Features Normal (mm hg) portal hypertensio n Portal venous pressure 7-10 >12 Intrasplenic pressure <17 >17 Wedge hepatic pressure <6 >6 smalathi 5
- 6. Classification of PHT Pre Sinusoidal:Extrahepatic(1) Intrahepatic(2) Sinusoidal(3) Post sinusoidal:intrahepatic(4) extrahepatic(5) smalathi 6 1 2 3 4 5
- 7. Pathophysiology of PH Cirrhosis results in scarring (perisinusoidal deposition of collagen) Scarring narrows and compresses hepatic sinusoids (fibrosis) Progressive increase in resistance to portal venous blood flow results in PH Portal vein thrombosis, or hepatic venous obstruction also cause PH by increasing the resistance to portal blood flow
- 8. Pathophysiology of PH As pressure increases, blood flow decreases and the pressure in the portal system is transmitted to its branches Results in dilation of venous tributaries Increased blood flow through collaterals and subsequently increased venous return cause an increase in cardiac output and total blood volume and a decrease in systemic vascular resistance With progression of disease, blood pressure usually falls
- 9. smalathi 9
- 10. Portal Vein CollateralsCoronary vein and short gastric veins -> veins of the lesser curve of the stomach and the esophagus, leading to the formation of varices Inferior mesenteric vein -> rectal branches which, when distended, form hemorrhoids Umbilical vein ->epigastric venous system around the umbilicus (caput medusae) Retroperitoneal collaterals ->gastrointestinal veins through the bare areas of the liver Posterior abdominal wall:veins of posterior abdominal wall,subdiaphragmatic veins,retroperitoneal veins. Splenorenal collaterals Splenoperitoneal collaterals.
- 11. Etiology of PH Causes of PH can be divided into 1. Pre-hepatic 2. Intra-hepatic 3. Post-hepatic
- 12. Pre-hepatic PH Caused by obstruction to blood flow at the level of portal vein Examples: congenital atresia, extrinsic compression, s, portal, superior mesenteric, or splenic vein thrombosis,cirrohsis.
- 13. Intrahepatic: Infections:cirrohsis due to hepatitis B,C. Metabolic disorders: wilson’s diseases. Congenitial hepatic fibrosis Chronic active hepatitis Chronic myeloid luekemia Lymphoma Sarcoidosis Luekemic infiltration Toxins:arsenic,vinyl chloride,hyperviayminosis A. smalathi 13
- 14. Post-hepatic Caused by obstruction to blood flow at the level of hepatic vein Examples: Budd-Chiari syndrome, chronic heart failure, constrictive pericarditis, vena cava webs
- 15. Budd-Chiari Syndrome Caused by hepatic venous obstruction At the level of the inferior vena cava, the hepatic veins, or the central veins within the liver itself result of congenital webs , acute or chronic thrombosis and malignancy
- 16. Budd-Chiari Syndrome Acute symptoms include hepatomegaly, RUQ abdominal pain, nausea, vomiting, ascites Chronic form present with the sequelae of cirrhosis and portal hypertension, including variceal bleeding, ascites, spontaneous bacterial peritonitis, fatigue, and encephalopathy Diagnosis is most often made by US evaluation of the liver and its vasculature Cross-sectional imaging using contrast-enhanced CT or MRI
- 17. Budd-Chiari Syndrome Gold standard for the diagnosis has been angiography Management has traditionally been surgical intervention (surgical decompression with a side- to-side portosystemic shunt) Minimally invasive treatment using TIPS may be first-line therapy now Response rates to medical therapy are poor
- 18. Portal Vein Thrombosis Most common cause in children (fewer than 10% of adult pts.) Normal liver function and not as susceptible to the development of complications, such as encephalopathy Diagnosis by sonography, CT and MRI Often, the initial manifestation of portal vein thrombosis is variceal bleeding in a noncirrhotic patient with normal liver function
- 19. Portal Vein Thrombosis - Causes Umbilical vein infection (the most common cause in children) Coagulopathies (protein C and antithrombin III deficiency), Hepatic malignancy, myeloproliferative disorders Inflammatory bowel disease pancreatitis trauma Most cases in adults are idiopathic
- 20. Portal Vein Thrombosis Therapeutic options are esophageal variceal ligation and sclerotherapy Distal splenorenal shunt Rex shunt in patients whose intrahepatic portal vein is patent (most commonly children)
- 21. Splenic Vein Thrombosis Most often caused by disorders of the pancreas (acute and chronic pancreatitis, trauma, pancreatic malignancy, and pseudocysts) Related to the location of the splenic vein Gastric varices are present in 80% of patients Occurs in the setting of normal liver function Readily cured with splenectomy (variceal hemorrhage), although observation for asymptomatic patients is acceptable.
- 22. Clinical Evaluation • Splenomegaly • Abdominal veins •Ascites • Varices
- 24. Pot belly & smiling umbilicus: smalathi 24
- 26. smalathi 26 • Splenomegaly • Ascites • PS Collaterals – abd. veins & varices • Hyper dynamic circulation • Porto Systemic Encephalopathy I Evaluation of PHT: type and consequences of PHT
- 27. II Evaluate: Physical signs of chronic liver disease
- 28. smalathi 28 III Evaluate: Presence of PSE •Neuropsychological tests •Asterixis •Foetor Hepaticus
- 29. smalathi 29 • An enlarged spleen is the single most important diagnostic sign of PHT •Does not correlate with height of portal pressure, size of varices or age of pt. •Correlates with type of PHT (* NCPF 12cm, * * EHPVO 6cm) •Spleen may not be palpable soon after a bleed Splenomegaly
- 30. smalathi 30 Dilated Abdominal Veins • Presence supports the diagnosis of PHT (Cirrhosis, BCS) • Absence does not exclude PHT (EHPVO) • Periumbilical veins indicate intrahep PHT, (murmur – Cruvellier Baumgarten) • Back veins – indicates HVOO (Classical BCS/IVC)
- 31. smalathi 31 Jean cruhveiller & paul caumen von baumgarten:
- 33. smalathi 33 Ascites • Presence of ascites supports diag of PHT • Present in sinusoidal/post-sinusoidal • Sudden accumulation of ascites – HVOO • “Frog belly” – IVC obstruction • Ascites in EHPVO (0-36%), NCPF (5-10%) transient
- 34. smalathi 34 • Consistency more significant than size • Size correlates poorly with height of pp. • Normal, soft or small liver EHPVO • Firm, nodular ,↓ vertical span or enlarged,L .lobe palpable- cirrhosis • Left lobe liver enlarged - CHF • Firm liver – NCPF (10-15% nodular) Liver Size & Consistency
- 35. smalathi 35 Presentation:GI Bleed • GI Bleed usually is the first presentation in EHPVO/NCPF. • Bleeds well tolerated in presinusoidal PHT. • Bleeds occur night / morning (Peaks at 10 P.M, 9A.M). • Mortality following variceal bleed in cirrhosis 20% to 30%.
- 36. smalathi 36 Porto Systemic Hepatic Encephalopathy • Minimal Encephalopathy (>50%) • Recurrent • Persistent • Acute All 4 forms seen in cirrhosis. In NCPF / EHPVO, this may follow GI bleed but majority recover
- 37. smalathi 37 • Hypersplenism • Thrombocytopenia - NCPF > EHPVO > Cirrhosis • Anemia • Anemia could also be secondary to GI Bleed Hematological changes
- 38. smalathi 38 Clinical Features • Growth Retardation – Resistance to the action of growth hormone (EHPVO) • Portopulmonary hypertension – non- embolic pulmonary vasoconstriction in the presence of PHT. (4% of cirrhosis, 9% of NCPF)) . • Hepatorenal syndrome – renal insufficiency in patients with severe liver failure in the absence of any other cause of renal pathology (cirrhosis).
- 39. smalathi 39 Clinical Features •Hepato pulmonary syndrome – triad of PHT, intrapulmonary vascular dilatation and arterial hypoxemia (PaO2 < 70mm of Hg) In the absence of primary cardio pulmonary disease. (17.5% cirrhotics, 13.3% NCPF, 10% EHPVO) Anand A C IJ Gastro 2001. •Foetor Hepaticus – results from porto systemic shunting of blood, allows mercaptans to pass directly to the lungs. •Portal Biliopathy
- 40. smalathi 40 Evaluation of various forms of portal hypertension Parameter EHPVO NCPF Cirrhosis HVOO Mean age (years) Children & occ. adults 18-25 All ages All ages GI Bleed ++ Well tolerated ++ Well tolerated + + / - Ascites 5% - 10% 5% - 10% + + + + + Pedal oedema - - ++ +++ Encephalopathy - - + + / - Spleen + + + ++ + + Liver Normal or Small volume Firm Decreased vol / firm / nodular Enlarged / firm / nodular
- 41. Anterior Abdomin al Veins - / few veins on lumbar region + / - ++ + + + Back vein T. Protein A/G ratio Normal Normal T.P decreased Glob increased T P decreased Glob increased (Chronic) US PV thrombosis Cavernoma Collaterals Splenomegaly Patent dilated PV splenomegaly collaterals Liver coarse echoes Collaterals dilated PV ascites Splenomegaly Liver enlarged Hepatic vein thrombosis or IVC obstruction Liver biopsy Normal Normal / Peri Portal fibrosis Necrosis, nodules fibrosis Centrilobular necrosis, fibrosis Reversed lobulation Features EHPVO NCPF CIRRHOSIS HVOO
- 42. Diagnosis of PHT Clinical Upper GI Endoscopy Ultrasound/Doppler smalathi 42
- 43. Complications of PH GI bleeding due to gastric and esophageal varices Ascites Hepatic encephalopathy
- 44. Varices Most life threatening complication is bleeding from esophageal varices Distal 5 cm of esophagus Usually the portal vein-hepatic vein pressure gradient >12 mm Hg Bleeding occurs in 25-35% of pts. With varices and risk is highest in 1st yr.
- 45. Prevention of Varices Primary prophylaxis: prevent 1st episode of bleeding Secondary prophylaxis: prevent recurrent episodes of bleeding Include control of underlying cause of cirrhosis and pharmacological, surgical interventions to lower portal pressure
- 46. Prevention of Varices Beta blockade: Beta blockade (Nadolol, Propranolol) Nitrates:Organic nitrates Surgery: No longer performed* Endoscopy: Sclerotherapy (no longer used* ) and variceal ligation * Refers to primary prophylaxis
- 47. Treatment of Varices Initial Management: 1. Airway control 2. Hemodynamic monitoring 3. Placement of large bore IV lines 4. Full lab investigation (Hct, Coags, LFTs,) 5. Administration of blood products 6. ICU monitoring
- 48. Pharmacologic Treatment of Varices Decreases the rate of bleeding Enhances the endoscopic ability to visualize the site of bleeding Vasopressin - potent splanchnic vasoconstrictor; decreases portal venous blood flow and pressure Somatostatin: decrease splanchnic blood flow indirectly; fewer side effects Octreotide: Initial drug of choice for acute variceal bleeding
- 49. Endoscopic Therapy for Varices Endoscopic Sclerotherapy: complications occur in 10- 30% and include fever, retrosternal chest pain, dysphagia, perforation Endoscopic variceal ligation: becoming the initial intervention of choice; success rates range from 80- 100%
- 50. Balloon Tamponade Sengstaken-Blakemore tube Minnesota tube Alternative therapy for pts. who fail pharmacologic or endoscopic therapy Complications: aspiration, perforation, necrosis Limited to 24 hrs; works in 70-80%
- 51. TIPS Transjugular intrahepatic portasystemic shunt 1st line treatment for bleeding esophageal varices when earlier-mentioned methods fail Success rates 90-100% Significant complication is hepatic encephalopathy
- 52. Surgical Intervention Liver transplantation: only definitive procedure for PH caused by cirrhosis Shunts Totally diverting (end-side portacaval) Partially diverting (side-side portacaval) Selective (distal splenorenal shunt) Devascularization