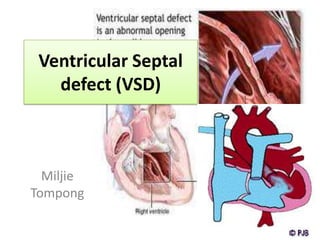
Ventricular septal defect (vsd)
- 1. Ventricular Septal defect (VSD) Miljie Tompong
- 2. Ventricular septal defect (VSD)? • a heart malformation present at birth. "congenital" condition • a type of congenital heart disease (CHD).
- 3. Anatomy and physiology • The heart with a VSD has a hole in the wall (the septum) between its two lower chambers (the ventricles).
- 5. How do VSDs cause problems?
- 6. How is a VSD diagnosed? • chest X-ray
- 7. • Echocardiogram (used to define the anatomy and evaluate the characteristics (amount and pressures) of the shunted blood)
- 8. Electrocardiogram • is a noninvasive test that is used to reflect underlying heart conditions by measuring the electrical activity of the heart.
- 9. What are the symptoms of a VSD? • A murmur is a sound generated by abnormally turbulent flow of blood through the heart. • symptomless at birth usually develop until later in the first week of life. • no signs of cyanosis.
- 10. • Small defects (less than 0.5 square cm) are common • small VSDs close spontaneously (on their own). • closure is due to the small VSD being located between heart fibers that increase in size in time
- 11. • large VSD (usually one greater than 1 cm2 • Infant will fail to thrive and become sweaty and tachypnoiec (breathe faster) with feeds • increase in the blood pressure of the lungs called "pulmonary hypertension.
- 12. Medical Management • Digoxin (LANOXIN) • works directly on the heart to increase the velocity of contraction and the force of the contraction. • FUROSEMIDE (LASIX) • Diuretics remove edema and act to lower blood pressure. This helps reduce the extra load on the pulmonary system.
- 13. Treatment • PA Banding a palliative treatment particularly reserved for those patients who are unable to withstand an open heart procedure for total correction.
- 14. Surgical Treatment • median sternotomy • Surgical access to the VSD depends upon it's location and the presence of other cardiac defects. • The right ventricle is often opened to gain access to perimembranous or inlet defects. • The pulmonary artery may be used to close outlet septum VSDs
- 15. • Large defects may be repaired using a pericardium patch sutured into place to occlude the space.
- 16. Preoperative and postoperative • prophylactic antibiotics are often required to prevent infectious endocarditis. • The child should be assessed postoperatively for dysrhythmia, since edema in the septum may interfere with conduction.
- 17. Nursing Diagnosis “Decrease in cardiac output associated with heart malformations” Objective: improve the heart Rainfall Outcome criteria: signs of improvement in cardiac output
- 18. Nursing Intervention : • Observation of the quality and strength of heart rate, peripheral pulse, skin color and warmth. • Set the degree of cyanosis (mucous membranes, clubbing) • Monitor signs of CHF (anxiety, tachycardia, tachipnea, cramped, tired while drinking milk, periorbital edema, and hepatomegaly Oliguria. • Collaboration for the administration of drugs (diuretics, to reduce after load) as indicated.
