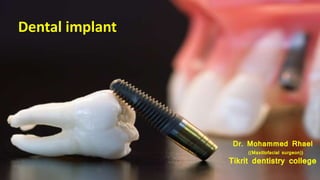
Dental implants
- 1. Dental implant Dr. Mohammed Rhael ((Maxillofacial surgeon)) Tikrit dentistry college
- 4. PROBLEMS ASSOCIATED WITH MISSING TEETH •The jaws may not “bite ”together properly, thus affecting the function of mastication/chewing •Pain na ot eud swaj/selcsum laicaf eht ni improper bite •Difficulty with speech •Aesthetically unpleasing yam selcsum laicaf eht sa‘ sag ’and gaps in the teeth might appear unsightly •Tilting : of neightbouring teeth •Supra-eruption : of opposing teeth •Food entrapment gnidael spag eht ni noitalumucca euqalp dna dna yaced erom ot gum disease •Last but not the least; your confidence gnitaeb a ekat thgim ni egnahc eht fo esuacebecnaraeppa
- 7. Stages of bone healing after tooth extraction Bleeding and clot formation Granulation tissue formation ( within 2-3 days ) Fibrin clot organization ( first 4 weeks) Woven ( immature ) bone formation (4-8)weeks Lamellar (mature ) bone development ( 8-12 weeks ) Bone stabilization (12 -16 weeks )
- 11. Factors influencing edentulous bone loss Mental health new studies show relation between depression and bone resorption. The link may be in part due to the hormones that are released in those with depression, which can break down bones. Hormones Particularly in women, estrogen plays a large role in bone density . When women begin menopause estrogen begins to drop , For good measure it is important to consume a calcium-rich diet and exercise in order to keep bones strong. Diet calcium is the key to healthy bones. Adult over the age of 50 recommended daily intake of calcium is 1,2 milligrams . salt, alcohol and caffeinated beverages can decrease bone density , Physical activity A lack of physical activity decrease bone density . When stress is added to bones it forces them to build new cells to make them stronger, thus building up bone density.
- 13. Bone remodeling
- 15. Methods for replacing missing teeth Fixed bridge ImplantsRemovable denture
- 16. dental implant : A prosthetic device made of alloplastic materials implanted into the oral tissues beneath the mucosa or within the bone to provide retention and support for removable and fixed dental prosthesis . Dental implant
- 17. •Dental implant surgery can offer a welcome alternative to dentures or bridgework that doesn't fit well and can offer an option when a lack of natural teeth roots don't allow building denture or bridgework tooth replacements.
- 21. Types of dental implants Endosseous implants Mucosal SUBPERIOSTEAL Transosseous
- 22. Mucosal implant
- 23. For more informations about mucosal implants please visit this web site : https://pocketdentistry.com/16- intramucosal-insert-surgery-and- prosthodontics/
- 24. SUBPERIOSTEAL :
- 26. Transosseous
- 28. Components of dental implant
- 29. fixture
- 33. Abutment
- 36. Gingival former
- 42. Analogue
- 44. osseointegration Time dependent healing process , where by clinically rigid fixation of alloplastic material is achieved and maintained during functional loading
- 45. Osseointegration is also a measure of implant stability two different stages: : primary and secondary Primary stability of an implant mainly comes from mechanical engagement with compact bone ,Secondary stability on other hand, offer biological stability through bone regeneration and remodeling. The former is a requirement for secondary stability
- 54. Measurment of oseointegration invasive/destructive methods Following methods were included: Histologic/histomorphologic analysis Tensional test Push-out/pull-out test Removal torque analysis. Histomorphometric analysis
- 56. For more informations about measurement of oseointegration , please visit this web site : https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4837777/
- 57. Clinical Assessments for Osseointegration Performing a clinical mobility test and finding that the implant is mobile is definite evidence that it is nonintegrated Radiographs demonstrating a apparently direct contact between bone and implant have been cited as evidence of osseointegration Radiolucent zones around the implant are a clear indication of its being anchored in fibrous tissue, Whereas the lack of such zones is not evidence for osseointegration. The use of a metal instrument to tap the implant and analyze the transmitted sound may, in theory, be used to indicate a proper osseointegration.
- 58. Clinical assessment of patient need dental implant History Clinical examination Intra oral Extraoral Investigations Radiographical evaluation
- 59. Radiographical evaluation Conventional imaging Opg occlusal Periapical Cephalometric Cone beam ct scan
- 62. Cone beam ct scan
- 63. Cone beam ct scan
- 69. TWO sTAGE IMPLANT PLACEMENT Also known as the “submerged” or “delayed” approach The implant was inserted in a first surgery and submerged for three to six months to permit osseointegration. In a second surgical procedure, the implant was exposed, its cover screw removed, and the implant was then fitted with an abutment and the prosthetic phase of treatment was completed. The two-stage approach is sometimes uncomfortable for the patient but has a proven record of success over time It continues to be a valuable surgical option when primary stability cannot be achieved, or if extensive pre- surgical or concurrent bone augmentation is required
- 70. A mucoperiosteal (full-thickness) flap is reflected up to or slightly beyond the level of the mucogingival junction, exposing the alveolar ridge of the implant surgical sites. The bone at the implant site(s) must be thoroughly debrided of all granulation tissue. Once the flaps are reflected and the bone is prepared (i.e., all granulation tissue removed and knife-edge ridges flattened), the implant osteotomy site can be prepared. A series of drills are used to prepare the osteotomy site precisely and incrementally for an implant. A surgical guide or stent is inserted, checked for proper positioning, and used throughout the procedure to direct the proper implant placement. 0 Implant is inserted into the prepared osteotomy site with a handpiece or handheld driver 0 Tissue approximation to achieve primary flap closure without tension Implant site preparation
- 72. ONE-STAGE IMPLANT PLACEMENT When aesthetics are not of concern, the cover screw or healing cap of the dental implant may be left exposed during healing process and osseointegration period . though several prerequisites must guide proper patient selection for this approach: •The patient must have bone quality (ideally type I or II) and quantity sufficient to ensure primary stabilization (the initial engagement between the bone and implant), i.e., no GBR required.The ISQ system is essential to confirm stability in this instance. • An adequate circumferential zone of keratinized gingival tissue must be present. •The abutment must precisely fit the implant. •The abutment must be tightened to the proper torque value as dictated by the implant manufacturer.Torque values are measured in N/cm and are different for each dental implant system. Using the proper torque value is critical in order to prevent undue loosening. • Abutment height must not compromise occlusion, and absolutely no contact or loading with the opposing dentition.
- 74. keys for successful preparation Always begin with pilot drill Don’t miss anatomy Maintaine vitility of bone Slow drilling High colling Sharp drill
- 76. Complications of dental implant Intraoperative Poorly positioned implant Damaged to mucosa and adjacent teeth Damaged to bone (lateral perforation , alveolar or jaw bone fracture….) Perforation to maxillary sinus or nasal floor Damage to nerve Loose implant (poor primary stability) Hemorrhage during surgery Post operative Pain Swelling Bleeding ( secondary ) Infection ( peri-implantitis ) Late Mucosal recession Bone resorption Mobility Implant fracture
- 77. Criteria for success Implant not mobile when tested clinically A radiograph does not show any evidence of periimplant radiolucency Vertical bone loss is less than 0.2 mm annually after the first year of service of the implant Absence of persistent singns and symptoms as pain , infection,paresthesia Asuccessful rate of 85% at the end of a 5% years observation period and 80 % at the end of a 10 years period
- 78. Causes of implant failure Poor quality and quantity of bone and soft tissue Patient medical condition Unfavorable patient habits (bruxism , long term smoking ,poor oral hygiene,.) Inadequate surgical analysis and technique Inadequate surgical analysis and technique Suboptimal implant desin and surface characteristics Implant position or location Unknown factors
- 79. https://www.slideshare.net/mohamedrahilalhadithy?utm_campaign=profiletracking&utm_ medium=sssite&utm_source=ssslideview https://web.facebook.com/mohamedrahil.alhadithy https://www.instagram.com/mohamed_rhael/ https://twitter.com/DrMohamed_rahil For any questions or notes please contact me on these links …
- 80. Thank you for listening…
