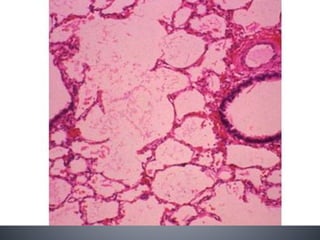
Ppt cyst lung
- 2. Pathology A cyst is a round circumscribed space surrounded by an epithelial or fibrous wall of variable thickness. Hansell DM, Bankier AA, MacMahon H, et al. Fleischner Society: Glossary of terms for thoracic imaging. Radiology 2008;246(3):697-722.
- 4. A cyst appears as a round parenchymal lucency or low attenuating area with a well defined interface with normal lung.The wall thickness is usually <4mm No associated pulmonary emphysema Usually contain air but may contain fluid or solid material Hansell DM, Bankier AA, MacMahon H, et al. Fleischner Society: Glossary of terms for thoracic imaging. Radiology 2008;246(3):697-722. Accessed via Pubmed.com
- 5. Also used to describe enlarged thin walled air spaces in lymphangioleiyomyomatosis and Langhan’s cell histiocytosis Thick walled honeycomb lungs seen in end stage fibrosis
- 6. Entity Imaging characteristics Lung cyst Well-circumscribed, rounded, thin-walled air-filled structure within the lung parenchyma. Wall thickness of ≤3mm. Cavity Air-filled space within the pulmonary parenchyma with thicker walls (>4 mm). Emphysema Polygonal-shaped lucent area without definable walls. Bronchiectasis Air-filled space within the lung parenchyma that branches and connects with the airway. Associated airway abnormalities including air trapping, bronchial wall thickening, and bronchiolar impactions. Honeycombing Clustered subpleural airspaces with variable size and wall thickness. Other signs of pulmonary fibrosis: architectural distortion, traction bronchiectasis, and reticular opacities.
- 7. They include bronchiolar check-valve mechanism, vascular occlusion or ischaemia necrosis, and dilation of the bronchioles Degradation of the connective matrix, especially by metalloproteinases, may play a further role particularly in LAM and PLCH 1. KuhlmanJE, Reyes BL, Hruban RH, et al. Abnormal air-filled spaces in the lung. Radiographics 1993; 13: 47–75. 2. IchikawaY, Kinoshita M, KogaT, et al. Lung cyst formation in lymphocytic interstitial pneumonia: CT features. J Comput AssistTomogr 1994; 18: 745– 748. 331. 3. Worthy SA, Brown MJ, Muller NL.Technical report: cystic air spaces in the lung: change in size on expiratory high-resolutionCT in 23 patients. Clin Radiol 1998; 53: 515–519. 332 4. Lee KN,Yoon SK, Choi SJ, et al. Cystic lung disease: a comparison of cystic size, as seen on expiratory and 5. inspiratory HRCT scans. Korean J Radiol 2000; 1: 84–90.
- 8. The valve mechanism had been defined by BROOKE as ‘‘one in which the entrance from a bronchus into a lung cavity become obstructed in a valve-like manner, presumably with a piece of necrotic tissue, and thus allows the ingress of air during inspiration but prevents the egress during expiration’’. Brooke B. Excessive spontaneous inflation of a lung cavity. Lancet 1931; 2: 240–241.
- 10. Focal or multifocal cystic lung disease Congenital Bronchogenic cysts Pulmonary sequestration Congenital cystic adenomatoid malformations (CCAM) Infectious Pulmonary tuberculosis Coccidioidomycosis Pneumocystis carinii pneumonia Echinococcus granulosus or E multilocularis Lymphocytic interstitial pneumonia (LIP) Desquamative interstitial pneumonia (DIP)
- 11. Diffuse cystic lung disease Pulmonary Langerhans’ cell histiocytosis (PLCH) Lymphangioleiomyomatosis (LAM) Honeycomb cystic lung disease Asbestosis Idiopathic pulmonary fibrosis Collagen vascular disease Hypersensitivity pneumonitis Sarcoidosis Miscellaneous Cystic lung disease in Down’s syndrome118 119 Birt-Hogg Dube syndrome120–122 Trauma
- 14. Bronchogenic cyst Pulmonary sequestration Congenital cystic adenomatoid malformation Lobar emphysema Bronchial atresia Lymphangiectasia Plueropulmonary blastoma
- 15. Pneumatocoele Others Lymphatic cysts Enteric cysts Mesothelial cysts Simple parenchymal cysts
- 16. Shanti and Klein (2008) studied a series of 236 patients undergoing pulmonary resection for cystic lung lesions. Bronchogenic cysts constituted 20% of this group. Of these 47 cases, 20 involved a lobar location, which required lobectomy, and 27 cases were extralobar and were treated with resection of the cyst. Shanti CM, Klein MD. Cystic lung disease. Semin PediatrSurg. Feb 2008;17(1):2-8.
- 17. Bronchogenic cysts are supernumery foregut buds disconnected and separated from the tracheobronchial tree to form a cystic mass during embryogenesis (between 4th - 6th weeks) Most common site is middle mediastinum (65- 90%) Remote locations, including the interatrial septum, neck, abdomen, and retroperitoneal space.
- 18. Most bronchogenic cysts are found incidentally. In infants- compression of the trachea or bronchi and esophagus-wheezing, stridor, dyspnea, and dysphagia. Intraparenchymal cysts may manifest with recurrent infection.
- 19. Thin walled spherical unilocular masses –fluid filled, air filled or with air fluid levels
- 21. Lined by secretory respiratory epithelium (cuboid or columnar ciliated epithelium) Wall-cartilage, elastic tissues, mucous glands and smooth muscle They do not usually communicate with the bronchial tree, and are therefore typically not air filled. Contain fluid (water), variable amounts of proteinaceous material, blood products, and calcium oxalate
- 24. MIMICS Enteric cyst Posterior mediastinum Gastric epithelium Oesophageal cyst Squamous lining Double muscle layer Pericardial cyst Unilocular, Mesothelial lining
- 25. Complications Fistula formation Ulceration of cyst wall Superimposed infection Haemorrhage
- 26. It is characterized by a portion of lung that does not connect to the tracheobronchial tree and has a systemic arterial supply,usually from the thoracic or abdominal aorta Newman B. Congenital bronchopulmonary foregut malformations: concepts and controversies. Pediatr Radiol 2006;36(8):773–791.
- 27. Two types of sequestration have been described: intralobar and extralobar. The extralobar form has its own pleural investment and systemic venous drainage, The intralobar form shares the pleural investment with the normal lung and usually (but not invariably) drains into the pulmonary venous system
- 29. Intralobar sequestration Early childhood or adolesence with recurrence lower lobe pneumonia Extralobar Usually asymptomatic May have cyanosis and feeding difficulties Associated with diaphragmatic hernias, cardiac malformations and foregut anomalies
- 32. Usually seen in the left lower lobe CT-homogenous soft tissue mass, cysts containing air or fluid, focal emphysema or hypervascular focus of lung parenchyma Lung tissue is poorly developed and cystically dilated Cysts lined by columnar to cuboidal epithelium
- 33. Pleura thickened with adhesions Parenchyma-cysts upto 5cm in dia with mucinous or purulent material and fibrosis.
- 35. Loose, spongy tissue with numerous small cystic spaces containing clear, mucoid fluid. Dilated bronchi with mucous or purulent material Alveoli filled with foamy macrophages Thick walled vessels reflecting systemic vascular drainage with elastic stains 1. DeParedes CG, Pierce WS, Johnson DG, Waldhausen JA. Pulmonary sequestration in infants and children: a 20-year experience and review of the literature. J Pediatr Surg. Apr 1970;5(2):136-47. 2. AFIP, Non neoplastic disorders of lower respiratory tract
- 38. A congenital pulmonary airways malformation (CPAM) (until recently described as a congenital cystic adenomatoid malformation (CCAM)) refers to a multi-cystic mass of segmental lung tissue with abnormal bronchial proliferation. It is considered part of the spectrum of bronchopulmonary foregut malformations BerrocalT, Madrid C, Novo S et-al. Congenital anomalies of the tracheobronchial tree, lung, and mediastinum: embryology, radiology, and pathology. Radiographics. 24 (1): e17.
- 40. Failure of normal broncho-alveolar development with hamartomatous proliferation of terminal respiratory units in a gland-like pattern (adenomatoid) without proper alveolar formation. These lesions have intracystic communications and, unlike bronchogenic cysts, can also have a connection to the tracheobronchial tree
- 41. The term congenital adenomatoid malformation of the lung was first used by Ch’in andTang in 1949 Incidence of about 1 in 25,000 live births Stocker described 3 types which were expanded to 5 types in 2005 Type 0 (Tracheobronchial) to type 4 (Alveolar)
- 42. CPAM, type 0, also known as acinar dysplasia or agenesis, is a rarely occurring and infrequently described malformation that is largely incompatible with life. It is seen in term and premature infants who are cyanotic at birth and survive only a few hours Associated with cardiovascular abnormalities and dermal hypoplasia
- 43. Bronchial type airways with cartilage, smooth muscle and glands separated by abundant loosely vascularised mesenchyme Ciliated pseudostratified cells with goblet cells Mucous cells and cartilage in all cases
- 45. CPAM, type 1, the large or predominant cyst type First week to month of life, can be seen in older children and even young adults. 65% of cases ,amenable to surgery with a good prognosis.
- 46. CT scan shows multiple large cysts (>2cm) involving the lower lobe of left lung.The cysts are air-filled, expand the lower lobe, cause mediastinal shift and hypoplasia of right lung
- 49. Boundary between lesion and adjacent lobe sharply delineated Cysts(2-10cm in diameter) lined by pseudostratified cilated columnar epithelium interspersed with rows of mucous cells(in 1/3rd of cases) Polypoid or papillary appearance due to elastic tissue beneath the epithelium Interspersed alveolar ducts,saccules and alveolae Absent cartilage and inflammation
- 50. Type 1 congenital cystic adenomatoid malformation (CCAM), the most frequent malformation of the lung, is the only type to present intracystic mucinous cell clusters, which may form beyond the cysts, extracystic mucinous proliferation resembling mucinous bronchioloalveolar carcinomas (BACs). As mucinous BACs are increasingly described in the literature in young patients with CCAM, we hypothesized that type 1 CCAM mucinous cells could represent BAC precursors. Mucinous Cells inType 1 Pulmonary Congenital Cystic Adenomatoid Malformation as Mucinous Bronchioloalveolar Carcinoma Precursors Lantuejoul, Sylvie MD, PhD; Nicholson, Andrew G. MD†; Sartori, Giuliana PhD; Piolat, Christian MD; Danel, Claire MD, PhD∥; Brabencova, Eva MD; Goldstraw, Peter MD; Brambilla, Elisabeth MD, PhD*; Rossi, Giulio MD AJSP, June 2007 -Volume 31 - Issue 6 - pp 961-969 doi: 10.1097/01.pas.0000249444.90594.27
- 52. CCAM-Maturation defects at various points during organogenesis and maturation Focal atypical goblet cell hyperplasia in 33% Bronchioloalveolar carcinoma in 1%. Mean age -26 years All mucinous in character Sheffield et al described premalignant changes in type 1 CCAM Epithelial hyperplasia and malignant change in congenital lung cysts Clin pathol 1987;40.61-14
- 53. Mucous cell proliferation-hyperplasia Extension into adjacent alveoli- lepidic growth pattern-Brochioloalveolar cell carcinoma IHC:IL-3,IL4 and MUC-2 nuclear staining in atypical goblet cells and cytoplasmic and nuclear staining in adjacent epithelium Chromosomal aberrations in the mucous cells similar to those in adenocarcinoma in non smokers Good prognosis with exceptional metastasis
- 54. BAC in CCAM less aggressive disease than BAC in a structurally normal lung DouglasWest et al, Dept of histopathology and cardiothorasic surgery,Glasgow uk The society of thorasic surgeons
- 55. CPAM, type 2, the medium cyst type, accounts for 10% to 15% of cases. Seen within the first year of life Poorer outcome Grossly, cysts rarely more than 1.5 cm in diameter that tend to blend with the normal adjacent parenchyma.
- 56. Areas of low attenuation consist of clusters of multiple, small and evenly spaced air cysts
- 58. Multiple small cysts(0.5-2cm) Small relatively uniform cysts resembling bronchioles separated by normal alveoli. Cysts are lined by cuboid-to-columnar epithelium and have a thin fibromuscular wall. No mucous cells or cartilage Solid pale tumor-like tissue with striated muscle in 5%
- 62. First days to month of life Male predominance, and owing to its large size Maternal polyhydramnios and fetal anasarca, high mortality rate Grossly, the lesion is “noncystic” and appears more like dense pulmonary parenchyma
- 63. Grossly a solid mass without obvious cyst formation
- 65. Solid appearance Excess of bronchiolar structure separated by small air spaces, with cuboidal lining resembling late fetal lung Microscopic adenomatoid cysts
- 67. The peripheral acinar cyst type, appears to be a hamartomatous malformation of the distal acinus. This variant is seen equally in boys and girls, with an age range of newborn to 4 years and accounts for 10% to 15% of cases. type 4 lesions may present with mild respiratory distress, sudden respiratory distress from tension pneumothorax, pneumonia.
- 68. Grossly, large thin-walled cysts are present at the “periphery” of the lobe and appear to be lined by a smooth membrane.
- 69. Cysts(upto 10 cm) are lined by flattened epithelial cells (type I and II alveolar lining cells) over most of wall, with occasional low cuboidal epithelium seen. The wall of the cyst is composed of loose mesenchymal tissue with prominent arteries and arterioles. Loose mesenchyme must not be confused with similar features seen in the cystic type of PPB.
- 71. Focal stromal hypercellularity (50%) Focal immature cartilage Associated pleuropulmonary blastoma (bilateral type 4 CCAM with stromal cellularity)
- 72. Low-grade cystic PPB has been confused with large cyst type 1 CCAM/CPAM and type 4 CPAM, and likely accounts for many, if not all, reports of malignancy arising in large cyst CCAM. Low-grade cystic PPB can be distinguished histopathologically on the basis of the presence of a thin layer of primitive mesenchymal cells beneath the cyst wall Hill DA, Jarzembowski JA, Priest JR,Williams G, Schoettler P, Dehner LP.Type I pleuropulmonary blastoma: pathology and biology study of 51 cases from the international pleuropulmonary blastoma registry. Am J Surg Pathol 2008;32(2):282–295.
- 73. Type 2 CPAM has been noted in nearly 50% of cases of extralobar sequestrations.
- 74. Type I or purely cystic PPB is usually associated with larger cysts, more typical of type 4 CCAM. Controversy exists as to whether the tumor develops within a CCAM or whether the cystic lesion represents PPB from the onset In a report of 50 cases from the PPB registry, the authors propose that CCAM could be a precursor to PPB just as nephrogenic rests and nephroblastomatosis are toWilms tumor J.R. Priest, M.B. McDermott, S. Bhatia et al. Pleuropulmonary blastoma,A clinicopathologic study of 50 cases Cancer, 80 (1997), pp. 147–161 D.A. Hill, L.P. Dehner, L.V. Ackerman A cautionary note about congenital cystic adenomatoid malformation (CCAM) type 4 Am J Surg Pathol, 28 (2004), pp. 554–555
- 75. Pulmonary blastomas are a relatively rare group of primary lung neoplasms that are composed of immature malignant epithelial and/or mesenchymal tissues whose features may resemble early embryological lung tissues. First described by Barnard in 1952. Koss M,TravisW, Moran C. Pulmonary sarcomas, blastomas, carcinosarcomas andTeratomas. Spencer’s Histopathology of the Lung (5th edn). NewYork, NY: McGraw Hill, 1996:1092–100. BarnardWG. Embryoma of lung.Thorax 1952;7:299
- 76. Solid, mixed and cystic heterogeneous low attenuation, pleural effusion , contralateral mediastinal shift, and lack of chest wall invasion .
- 78. Type 1-Multicystic Cysts separated by fibrovascular septae lined with benign respiratory epithelium Stroma-small round to spindle cells condensing to form a continuous cambium layer beneath the epithelium Rhabdomyoblastic differentiation
- 82. Congenital lobar emphysema (CLE) refers to an over inflation of one or more lung lobes presumably due to various factors including a possible obstructive check valve mechanism at a bronchial level . BerrocalT, Madrid C, Novo S et-al. Congenital anomalies of the tracheobronchial tree, lung, and mediastinum: embryology, radiology, and pathology. Radiographics. 24 (1): e17.doi:10.1148/rg.e17
- 83. Neonatal period or infancy Males>females Left upper lobe and right middle lobe
- 84. Congenital lobar overinflation-Normal architecture with overdistention of the alveoli No true emphysematous changes Emphysema: Permanent distention of the airspaces distal to the terminal bronchiole with destruction of their walls
- 85. Etiology Not found in up to 50% Bronchial obstruction found in ~25% Allows collapse on exhalation (ball-valve mechanism) Air trapping leads to alveolar overinflation
- 86. 1. Intrinsic obstruction (more common) Intramural: Defect in the bronchial wall Defective quantity or quality of cartilage Intraluminal: Lesion in the lumen of the bronchus Redundant bronchial folds, mucous plugs 1. Extrinsic obstruction Compression of the bronchus from a lesion outside the bronchial wall Cardiovascular: PDA, vascular sling Mass: Lymph node, bronchogenic cyst, oncologic mass
- 87. Upper lobes are predominantly involved LUL: 42% RML: 35% RUL: 21% Lower lobes: <1% Bilateral involvement: ~20%
- 88. Symptoms (in order of decreasing frequency) 1. Moderate respiratory distress (most) 2. Cyanosis (half) 3. Mild respiratory distress (less than half) 4. Asymptomatic (infrequent) 5. Severe life-threatening distress (least common)
- 94. Massive distention of alveolar spaces, but no tissue destruction
- 96. It is necessary for pediatricians to evaluate associated anomalies because 14% of the cases of CLE have coexistent congenital heart disease
- 97. Bronchial atresia (BA) is a developmental anomaly characterised by focal obliteration of the proximal segment of a bronchus. The bronchi distal to the atresia become filled with mucus and may form a mucocoele The lung distal to the atretic bronchus develops normally but is overinflated due to collateral air drift with air trapping. Most commonly occurs at the apico-posterior segment of the left upper lobe
- 99. The bronchioles plugged by mucus and the surrounding alveoli are dilated. Many neutrophils and macrophages were found within the bronchi and surrounding lung parenchyma, indicating acute or chronic infection. Alveoli were enlarged, with a loss of alveolar walls.
- 100. Primary pulmonary lymphangiectasia (PPL) is a rare disorder of unknown aetiology characterised by dilatation of the pulmonary lymphatics Primary pulmonary lymphangiectasia in infancy and childhood P.M. Barker, C.R. Esther Jr, L.A. Fordha, S.J. Maygarden, W.K. Funkhouser European respiratory journal
- 101. Full term infants with respiratory distress, pleural effusion(chylous)/generalised oedema Pleural effusions with diffuse interstitial infiltrates
- 102. Diffuse thickening of the interstitium, both of the peribronchovascular interstitium and the septa surrounding the lobules
- 103. Dilated lymphatic spaces in the sub-pleural connective tissue, along thickened interlobar septa, and around bronchovascular axes
- 104. Developmental cysts Non-infectious: Blebs and bullae Pulmonary Langerhans’ cell histiocytosis (PLCH) Lymphangioleiomyomatosis (LAM) Honeycomb lung Infectious: Pneumatocoele Pneumocystis carinii pneumonia (PCP) Tuberculosis Hydatid cyst Coccidiodomycosis
- 105. Pleuropulmonary blastoma Cystic teratoma Multicystic mesothelioma Cystic mesenchymal hamartoma Metastases
- 106. Cystic bronchiectasis HartmanTE. CT of cystic diseases of the lung. Radiologic Clinics of North America. 2001;39(6):1231-43
- 107. Disease Findings Distribution Assoc. Findings IPF Honeycomb cysts Subpleural, basilar predominance Irregular lines of attenuation, ground- glass PLCH Thin-walled cysts Random, spares bases Nodules LAM Thin-walled cysts Random, diffuse Chylous effusion
- 108. TS Thin-walled cysts Random, diffuse Angiomyolipomas of kidneys and liver LIP Thin-walled cysts Basilar predominance Ground-glass attenuation Cystic Bronchiectasis Cystic structures contiguous with bronchial tre Diffuse or focal Signet ring sign: each cystic space has an attendant vessel Adapted from: HartmanTE. CT of cystic diseases of the lung. Radiologic Clinics of North America 2001;39(6):1231-43.
- 109. CT Scan:Thin walled cystic air space contiguous with the pleura Arbitrary distinction between bleb and a bulla is of little clinical significance Hansell DM, Bankier AA, MacMahon H, et al. Fleischner Society: Glossary of terms for thoracic imaging. Radiology 2008;246(3):697-722.
- 110. The term bleb usually connotes a subpleural collection of air within the layers of visceral pleura caused by a ruptured alveolus. The air dissects through the interstitial tissue into the thin, fibrous layer of visceral pleura where it accumulates to form a bleb. Rupture of a bleb is often associated with the development of a spontaneous pneumothorax Cystic and Bullous Lung Disease Robert R. Klingman, MD, Vito A. Angelillo, MD, andTom R. DeMeester, MD Departments of Surgery and Pulmonary Medicine, Creighton University School of Medicine, Omaha, Nebraska AnnTkorac Surg 1991;52:576-80)
- 111. An air filled space within the lung parenchyma resulting from deterioration of the alveolar tissue. These lesions have a fibrous wall , trabeculated by the remnants of alveolar septa. They can develop in a lung that is otherwise normal or in a lung in which the architecture has been destroyed by chronic obstructive disease.
- 112. Bullae can reach substantial size and occupy an entire lobe Usually seen in chronic obstructive pulmonary disease but also seen in normal young healthy individuals Chronic obstructive pulmonary disease- no lobar predilection for the bullae Asymptomatic patients, bullae - in the upper lobes and peripherally
- 113. Bullae are large dilated airspaces that bulge out from beneath the pleura
- 116. Bulla results from destruction of alveolar walls (paraseptal emphysema).The bleb results from rupture of alveolar air into the pleura
- 117. Bullae in the substance of the lung Blebs in the visceral pleura outside the inner elastic lamina
- 118. PLCH is typically a disease of young adults which predominately affects the lungs and bones Very strong association with smoking(90%) Interstitial lung disease Lung affected in isolation or in association with organ systems
- 119. Pulmonary disease in PLCH is characterized by peribronchiolar 1-10 mm nodules in the early stages In later stages of PLCH, the major pulmonary finding is cysts (present in 80% of patients) and there may be no nodules present Lung bases are relatively spared at all disease stages
- 120. The abnormalities are diffuse and symmetrical. The cysts in PLCH vary in size and shape, in contrast to the uniform appearance of cysts in lymphangioleiomyomatosis (LAM)
- 121. Characteristic combination of diffuse cysts and centrilobular micronodules
- 123. Cysts more pronounced later in the disease usually less than 10mm in diameter may measure up to 2 - 3 centimetres in size Thin-walled, but on occasion may be up to a few millimetres thick confluence of 2 or more cysts results in bizarre shapes : bilobed cloverleaf branching internal septations
- 125. The earliest histologic lesion of PLCH consists of proliferation of Langerhans’ cells along small airways These early cellular lesions expand to form nodules 1 to 5 mm in diameter. The characteristic lesion is composed of variable numbers of Langerhans’ cells,eosinophils,plasma cells, lymphocytes, fibroblasts, and pigmented alveolar macrophages, which form a loosely aggregated granulomas These granulomas are typically centered around distal bronchioles, where they infiltrate and destroy airway walls
- 129. It is postulated that as these cellular granulomas evolve, peripheral fibrosis forms resulting in traction on the central bronchiole which becomes cyst-like Evolution from nodule, through cavitating nodule and thick walled cysts, to the 'stable' thin-walled cysts Electron microscopy may reveal characteristic Birbeck granule
- 130. Lymphangioleiomyomatosis (LAM) is a disorder of smooth muscle proliferation. Primarily affects women of childbearing age. It also can present after menopause in women undergoing estrogen hormonal treatment. This condition is indistinguishable from pulmonary involvement in tuberous sclerosis, which can also occur in men
- 131. Characterized by the progressive proliferating and infiltrating smooth muscle like cells (lymphangioleiomyomatosis cells) Cystic destruction of the lung parenchyma; obstruction of airways, blood vessels, and lymphatics 2 main forms:tuberous sclerosis complex (TSC)– associated LAM and sporadic LAM (S-LAM). In tuberous sclerosis, type II pneumocytes form clusters termed multifocal micronodular pneumocyte hyperplasia that are unique toTSC and may occur in the absence of LAM in these patients
- 132. Two phases of proliferation in lymphangiomyomatosis. The early phase - proliferation of immature muscle cells which cover alveolar walls, bronchioles, pleura and vessels, including lymphatic routes. Late phase - development of cystic spaces and wider proliferation of muscle cells throughout the lung.
- 133. An immunohistochemical study of metalloproteinases (MMP) and their inhibitors suggested that MMP-2 and MMP-9 (both of which can degrade elastin as well as the collagens) are responsible for the connective tissue destruction and cyst formation in LAM HayashiT, Fleming MV, Stetler-Stevenson WG, et al. Immunohistochemical study of matrix metalloproteinases (MMPs) and their tissue inhibitors (TIMPs) in pulmonary lymphangioleiomyomatosis (LAM). Hum Pathol 1997; 28: 1071–1078.
- 134. It shows thin-walled cysts of relatively uniform size diffusely distributed throughout all lung fields .The cysts may vary in size from 2 to 40 mm
- 137. Small clusters or nests at the edges of the cysts and along the alveolar walls, pulmonary blood vessels, lymphatics, and bronchioles . Mitotic figures are rarely seen. Loss of alveoli is associated with cyst formation
- 138. The proliferating LAM cells are morphologically heterogeneous and can be classified into 2 types: spindle-shaped cells and epithelioid cells. Spindle-shaped cells are centrally located, whereas the epithelioid cells exist in the peripheral regions of the LAM cell nodules
- 142. Lymphangioleiomyomatosis cells coexpress smooth muscle markers (such as smooth muscle actin and desmin) and melanocytic markers (such as HMB-45, Melan-A/MART- 1, and microphthalmia transcription factor) Coexpression of contractile proteins and melanocytic markers, LAM cells are suggested to be of perivascular epithelioid cell origin
- 143. Demonstration of the presence of estrogen receptor (ER) and progesterone receptor (PR) in the epithelioid LAM cells (50%) who never received hormone treatment. ER and PR are selectively expressed in epithelioid LAM cells and are down-regulated by hormone therapy Matsui K,Takeda K,Yu ZX, et al. Downregulation of estrogen and progesterone receptors in the abnormal smooth muscle cells in pulmonary lymphangioleiomyomatosis following therapy: an immunohistochemical study. Am J Respir Crit Care Med. 2000;161(3, pt 1):1002–1009.
- 144. Recently, CD1a and cathepsin K were found to be positive in both spindle shaped and epithelioid LAM cells Useful new markers for the diagnosis of pulmonary LAM and renal angioleiomyoma Chilosi M, Pea M, Martignoni G, et al. Cathepsin-K expression in pulmonar lymphangioleiomyomatosis. Mod Pathol. 2009;22(2):161–166 AdachiY, HorieY, KitamuraY, et al. CD1a expression in PEComas. Pathol Int. 2008;58(3):169–173
- 145. Pneumatocoeles are intrapulmonary air- filled cystic spaces that can have a variety of sizes and appearances. They may contain air-fluid levels and are usually the result of ventilator-inducted lung injury in neonates or post-pneumonic
- 146. Staphylococcus aureus: most common Pneumocystis carinii Streptococcus pneumoniae Haemophilus influenzae Escherichia coli Group A streptococci Klebsiella pneumoniae Adenovirus Primary tuberculosis
- 147. Smooth inner margins Contain little if any fluid Wall (if visible) is thin and regular Persist despite absence of symtpoms
- 148. Arise from necrotic foci that develop early in disease, initially have irregular shapes and thick walls. Exudate disappears, and walls thin. Necrotic material around the pneumatocele. Walls can contain organized inflammatory cells with focal collections of multinucleated giant cells. In 1972, Boisset reported the presence of air corridors between the bronchiolar lumen and the interstitial space Boisset GF. Subpleural emphysema complicating staphylococcal and other pneumonias.J Pediatr. Aug 1972;81(2):259-66.
- 149. True infectious cysts that persist despite resolution of the primary infection may occur with Pneumocystis carinii pneumonia or Echinococcosis (hydatid disease).
- 150. Cysts vary in size, shape, number, wall thickness – Thin-walled (<3mm), usually air-filled – Usually multiple, bilateral – May be intraparenchymal or subpleural – upper lobe predominance Cystic disease now occurs in 10-34% PCP cases Cysts in HIV patient are highly suggestive of PCP Boiselle, PM, Crans, CA and Kaplan, MA. The Changing Face of Pneumocystis carinii P in AIDS Patients. AJR 1999; 172: 1301- 1309.
- 151. Lung cysts are usually multiple, thin walled and bilateral, but range in size, shape and distribution
- 152. Alveoli which are distended with honey- combed, foamy, brightly eosinophilic material .There is a scanty inflammatory infiltrate composed mainly of monocyte, occasional plasma cells and histiocytes.
- 153. Grocott's silver stain shows black cysts in alveolar wall & exudates. It looks as round or indented (“new-moon” shape). )
- 154. Tuberculosis may present with atypical manifestations in one-third of the cases, and multiple thin-walled cysts are one such rare manifestations of tuberculosis Lee JY, Lee KS, Jung KJ et al. Pulmonary tuberculosis: CT and pathologic correlation. J Comput AssistTomogr 2000; 24:691-8.
- 155. Marked caseating necrosis of the bronchial walls cystic bronchiectasis Granulomatous involvement of the bronchioles may lead to a check-valve mechanism leading to cyst formation In isolated cases, isoniazid has been implicated
- 156. Multiple large cysts (bilateral), thin walled, and involving all zones of the lung
- 157. Hydatid cysts may be solitary or multiple, the number depending mainly on the amount of ova ingested and the number of embryos filtered through the liver and lungs. A centrally located cyst is said to be usually round, but may become oval or polycyclic
- 158. Inferior lobes most commonly affected Intact:ruptured::3:1 The cysts may change shape on maximum inspiration and expiration, which is known as the Escudero- Nimerov sign, but which is true also of any thin-walled water filled cyst
- 159. Calcified unilocular hydatid cyst. Contrast material- enhanced CT scan shows a round lesion with water attenuation and a ringlike pattern of calcification (arrows).This pattern represents calcification of the pericyst and strongly suggests a diagnosis of hydatid cyst
- 161. Outer acellular laminated membrane Germinal membrane Protoscolices, attached and budding from the membrane
- 163. When acute, cavities can be thick-walled or surrounded by dense consolidation. Thin walled grape skin cysts can also be seen with acute infection or as a result of healing of the thick walled lesions
- 165. large (up to 80 micron) spherules/sporangia, as shown in this case.These are filled with numerous spherical endospores.The sporangia and endospores can be within giant cells or extracellularly.
- 166. The original usage was a gross pathological term employed at autopsy to describe lungs with a wormeaten or honeycomb appearance II. HEPPLESTON,A. G. Pathology of honeycomb `lung. Thorax, 1956, II, 77-94.
- 167. Honeycombing represents destroyed and fibrotic lung parenchyma with numerous cystic airspaces with thick fibrous walls representing the late stages of lung diseases with complete loss of acinar architecture. Variable wall thickness and lined by metaplastic bronchiolar epithelium Hansell DM, Bankier AA, MacMahon H, et al. Fleischner Society: Glossary of terms for thoracic imaging. Radiology. 2008;246(3):697- 722.
- 168. Essential change is the obliteration of bronchioles by fibrosis or granulomata and compensatory dilatation of neighboring bronchioles, which forms the honeycomb appearance Heppleston AG.The pathology of honeycomb lung.Thorax 1956; 11:77–93
- 169. “Clustered cystic air spaces, typically of comparable diameters on the order of 3–10 mm but occasionally as large as 2.5 Cm. Usually subpleural and characterized by welldefined walls” However, “the cystic air spaces of honeycomb lung tend to share walls” Hansell DM, Bankier AA, MacMahon H, McLoud TC, Muller NL, Remy J. Fleischner Society: glossary of terms for thoracic imaging. Radiology 2008; 246:697–722 WebbWR, Muller NL, Naidich DP. Standardized terms for high- resolution computed tomography of the lung: a proposed glossary. JThorac Imaging 1993; 8:167–175
- 171. Honeycombing was identified in 41–100% of UIP, depending on the reported series . Nonspecific interstitial pneumonia (NSIP) and desquamative interstitial pneumonia (DIP), which are the chronic interstitial pneumonias of IIP show honeycombing in 0–30% and 4.3– 39%, respectively . In acute interstitial pneumonia, the frequency is lower, ranging from 6% to 14%
- 172. Honeycomb cysts are a feature of idiopathic pulmonary fibrosis (IPF) and typically have a subpleural location Walls of the cysts are clearly defined and thickened – a sign of fibrosis Predominant in posterior and lower lobes This characteristic distribution distinguishes UIP from other diseases with honeycomb lung.
- 174. Diffuse ground glass opacities with cysts (arrow). (B) A high resolution CT scan from the same patient more clearly shows cysts within ground glass opacities.Traction bronchiectasis is also present, suggesting that the ground glass opacities are secondary to fibrosis rather than an inflammatory process.
- 175. Multiple thin-walled cysts occupying most of lobe. Note that some cysts contain mucous material
- 176. Idiopathic pulmonary fibrosis showing traction bronchiectasis (white arrows).The adjacent bronchi and vasculature differentiates these structures from true cysts. End-stage lung fibrosis is evident with diffuse honeycombing (black arrow), reticulation and traction bronchiectasis.
- 177. Patchwork pattern, which is characterized by alternating zones of abnormal and normal lung side by side without transition zones Small islands of residual normal or nearly normal lung interspersed among extensively scarred parenchyma Combination of areas of honeycomb change and scars that replace normal alveoli Honeycomb areas are characterized by enlarged airspaces lined by bronchiolar epithelium and often filled by mucin and variable numbers of inflammatory cells. Small areas of active fibrosis (fibroblast foci) are present in the background of collagen deposition
- 179. It is a disease that is seen almost exclusively in current or former smokers Accumulation of pigmented macrophages within the airspaces with a homogenous appearance and limited mononuclear infiltrate within the interstitium.
- 180. The alveolar septa are thickened by a sparse inflammatory infiltrate that often includes plasma cells and occasional eosinophils, and they are lined by plump cuboidal pneumocytes.The intraluminal macrophages in DIP frequently contain dusty brown pigment .
- 181. Cellular non-specific interstitial pneumonia (NSIP) pattern. On higher power, the septal widening is due to a mild to moderate infiltrate of lymphocytes with scattered plasma cells, with minimal associated fibrosis.
- 182. Marked thickening of the alveolar septa due to interstitial edema, inflammatory cell infiltration, fibroblast proliferation (within the interstitium and airspaces), and type II cell hyperplasia, Hyaline membranes in focal areas along alveolar septa,Thrombi in small arteries
- 185. Honeycomb cystic lung disease Asbestosis Collagen vascular disease Hypersensitivity pneumonitis Sarcoidosis
- 186. Bronchiectasis, or the dilatation and distortion of bronchi and bronchioles, may be mistaken for cystic airspace disease when a dilated airway is viewed ‘‘en face’’ Bronchiectasis may be the result of either a chronic suppurative process or accompany lung fibrosis, when it is then referred to as traction bronchiectasis Challenges in pulmonary fibrosis ? 3: Cystic lung disease Gregory P Cosgrove, Stephen K Frankel, Kevin K Brown Thorax 2007;62:820–829. doi: 10.1136/thx.2004.031013
- 187. Cystic bronchiectasis can be differentiated from true cystic lung disease by the continuous relationship of the cystic structure to bronchial tree Approximately uniform, medium-sized cavities are typical of cystic bronchiectasis. Valsalva and Mueller maneuvers produce rapid change in the size of cysts, which freely communicate with the airways; this change distinguishes cystic bronchiectasis from other conditions.
- 188. Differentiated from cystic lung disease by the presence of an adjacent blood vessel suggesting a bronchovascular unit rather than a cystic air space.
- 192. Mesenchymal cystic hamartoma (MHC) of the lung is a very rare disease with an indolent clinical course and might be easily misdiagnosed as pleuropulmonary blastoma and other uncommon cystic lung lesions
- 194. Bilateral multifocal cysts lined by normal or metaplastic respiratory epithelium resting on a cambium layer of mesenchymal cells ● Lesion is initially solid, but becomes cystic when approximately 1 cm in diameter ● Slow growing
- 195. Cysts were lined with normal respiratory epithelium. Beneath the epithelium were band-like layers of cells composed of primitive mesenchymal- like cells with dark oval nuclei, scanty cytoplasm, and very rare mitoses . Scattered or clustered mature fat cells were present in some areas of the cysts and nodules
- 196. Rarely described in the pleura Single or multiple thin walled cysts Multiloculated cyst lined by attenuated or cuboidal cells with atypia
- 198. Intrapulmonary teratomas typically range from 2.8 to 3 cm in diameter, and are cystic and multiloculated but may rarely be predominantly solid In 42% of the cases, the cysts are in continuity with bronchi, and have an endobronchial component resulting in hemoptysis or expectoration of hair or sebum
- 199. Radiographically, lesions are typically cystic masses often with focal calcification. Microscopically, mesodermal, ectodermal and endodermal elements are seen in varying proportions. Pulmonary teratomas are mostly composed of mature, cystic somatic tissue Mature elements often take the form of squamous lined cysts. Thymic or pancreatic elements may be seen in mature teratomas
- 200. The appearance of cystic lesions in the lung in malignancy is rare and predisposes to spontaneous pneumothoraces. Multiple cystic lesions occur commonly in bronchus carcinoma and also sarcoma, bladder cancer and, less commonly, lymphoma Both chemotherapy and immune suppression can induce cavitation in malignant lesions. Tumour necrosis and tumour infiltration of air- containing spaces with a check-valve mechanism are postulated for causing these cystic lesions
- 201. Spontaneous pneumothorax complicating sarcoma is associated with most cell types, recurrent in nearly half of the patients The main cell types consisted of angiosarcoma (39%), leiomyosarcoma (15%) and osteosarcoma (15%) Hoag JB, Sherman M, FasihuddinQ, et al. A comprehensive review of spontaneous pneumothorax complicating sarcoma. Chest 2010; 138: 510–518
- 202. Metastases from the head and neck tended to cavitate when small and to have thin walls, whereas metastases from squamous cell carcinomas of the bladder and genitalia generally cavitated when they were larger and had thickened walls. Seminoma, Ewing sarcoma, myxosarcoma, Wilms tumor, osteogenic sarcoma, angiosarcoma, transitional cell carcinoma, teratocarcinoma Multiple,Thin-Walled Cystic Lesions of the Lung J. David Godwin,w. RichardWebb, Charles J. Savoca Gordon Gamsu, Philip C. Goodman AJR 135:593-604, September 1980 0361 -803X/80/1 353-0593
- 203. Pulmonary thromboembolism Neurofibromatosis Follicular bronchitis Pulmonary spread of laryngeal papillomatosis Hodgkin’s lymphoma Rheumatoid arthritis with necrobiotic nodules Birt Hogg syndrome Down’s syndrome