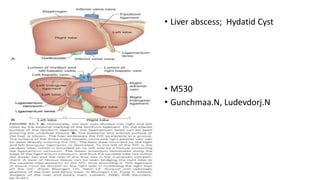
Liver Abscess and Hydatid Cyst, Surgery
- 1. • Liver abscess; Hydatid Cyst • M530 • Gunchmaa.N, Ludevdorj.N
- 5. Epidemiology • Patients in their 50s or 60s • Often related to biliary tract disease • Cryptogenic in nature (uncertain in origin)
- 6. Pathogenesis • An inoculum of bacteria exceeds the livers ability to clear it. • Tissue invasion • Neutrophil infiltration • Abscess formation
- 7. Biliary tree • Stone or malignant disease • Biliary obstruction • Bile stasis • Bacterial colonization • Ascends to liver • Ascending suppurative cholangitis
- 8. Portal vein • Ascending portal vein infection – pyelophlebitis • Diverticulitis, appendicitis, pancreatitis, IBD etc • Malignant disease
- 9. Hepatic artery • Any systemic infection • Altered immune response • Direct infection extension
- 10. Other causes • Necrotic liver: • Trauma • Hepatic artery embolization • Thermal ablative procedures
- 11. Pathology • 75% right hemiliver • 20% left hemiliver • 5% caudate lobe • Mostly solitary • 1 mm – 4 cm • Multiloculated or in single cavity
- 12. Microbiology • Either polymicrobial or single organism • Escherichia coli • Klebsiella pneumoniae • Staphylococcus aureus • Enterococcus sp.
- 13. Clinical features • Fever • Chills • Jaundice • RUQ pain • Tenderness to palpation • Hepatomegaly • Acute or chronic
- 14. Complication • If diaphragm is involved, cough or dyspnea • Peritonitis secondary to rupture • Rupture into pleural space or pericardium • Endogenous endophthalmitis (Klebsiella)
- 15. Lab findings • Leukocytosis • Anemia • LFT abnormality • ALP elevated /80%/ • Total bilirubin elevated /20-50%/ • Transaminases increase /60%/ • Hypoalbuminemia, increased PT
- 16. Radiology • Chest X-ray Atelectasis Right pleural effusion Elevated right hemidiaphragm • Plain abdominal X-ray - Air fluid levels - Portal venous gas
- 17. Radiology • Ultrasound – round or oval, less echogenic than surrounding liver • CT – lesions are of lower attenuation than surrounding liver, multiple small abscesses • Both are useful in diagnosing intra-abdominal diseases
- 19. Differential diagnosis • Amebic abscess • Echinococcal cyst
- 20. Treatment • Immediate broad spectrum IV antibiotics /2 weeks</ • Combination of ampicillin, aminoglycosides, metronidazole • Aspiration, send for culture. • Percutaneous catheter drainage • Contraindications: ascites, coagulopathy, proximity to vital structures • If larger than 5 cm, surgery is better • Liver resection if destruction is severe
- 21. Amebic Abscess
- 22. Epidemiology • Largely a disease in tropical or developing countries • Less than 50% are symptomatic • Mostly Hispanic men • 20-40 age • Socioeconomic status • Alcohol consumption • Immunosuppression • Travel history
- 23. Pathogenesis • E.histolytica is a protozoan that exists as trophozoite or cyst • Fecal-oral route • When ingested, cysts aren’t degraded in stomach • Trophozoite released • Invades colon mucosa • Enzymatic cellular hydrolysis
- 24. Pathogenesis • Localized necrosis • Cavity forms • It contains proteinaceous debris • Surrounded by rim of trophozoites • Rapid IgA release
- 25. Pathology • Cavity full of blood, liquefied liver tissue • The fluid is odorless • Glisson capsule resistant to hydrolysis • Early stage, ill-defined • Right hemiliver
- 26. Clinical features • Last from days to 4 weeks • Fever • Chills • RUQ pain and tenderness • Hepatomegaly • Constant, dull abdominal pain • Diarrhea • Anorexia • Jaundice
- 27. Clinical features • Acute <10 days • High fevers, chills, abdominal tenderness • Multiple lesions usually • Chronic > 2 weeks • Single right-sided lesion • Response is similar in both groups
- 28. Lab findings • Mild to moderate leukocytosis with no eosinophilia • Anemia • LFT abnormality • Elevated PT-INR • Enzyme immunoassay • Detection kit
- 29. Radiology • Plain chest x-ray: elevated right hemidiaphragm, pleural effusion, atelectasis • Ultrasound: Round lesions, liver capsule, without significant rim echoes. Contents are hypoechogenic, nonhomogenous • CT: more sensitive • Nuclear studies: to differentiate from pyogenic abscess. No leukocytes, does not light up
- 31. Differential diagnosis • Viral hepatitis • Echinococcal disease • Cholangitis • Cholecystitis • Appendicitis • Liver tumor • Pyogenic abscess
- 32. Treatment • Metronidazole 750 mg orally, three times daily, 10 days • Emetine hydrochloride • Chloroquine • After liver abscess is treated, iodoquinol, paromomycin, diloxanide furoate to treat carrier state • If failure of metronidazole in 3-5 days, diagnostic aspiration • Larger than 5 cm, in left side – aspiration • Radiologic resolution 3-9 months
- 33. Hydatid Cyst
- 34. • Hydatid disease or echinococcosis is a zoonosis that is common worldwide because the dog is a definitive host. • Human contract the disease from dogs, but there is no human to human transmission
- 35. • 3 species that cause hydatid cyst: • Echinococcus granulosus • Echinococcus multilocularis • Echinococcus ligartus • Humans are end stage to the parasite.
- 36. • In the human duodenum, the parasitic embryo releases an oncosphere containing hooklets that penetrate the mucosa, allowing access to the bloodstream. • In the blood, it can reaches the liver or lungs, where the parasite develops its larval stage
- 37. • 3 weeks after infection, a visible hydatid cyst develops, which then slowly grows in a spherical manner.
- 38. • The cyst wall itself has 2 layers, an outer gelatinous membrane (ectocyst) and an inner germinal membrane (endocyst). • Brood capsules are small, intracystic cellular masses in which future worm heads develop into scoleces. In a definitive host, the scoleces develops into an adult tapeworm.
- 39. Hydatid cysts can die with: • degeneration of the membranes • Development of cystic vacuoles • Calcification of the wall • Calcification of a hydatid cyst, however, doesn’t always imply that the cyst is dead
- 40. • Hydatic cysts are diagnosed in equal numbers of en and woman at an average age of about 45 years. • Approximately 75% of hydatid cysts are located in the right liver and are solitary
- 41. • The clinical presentation of a hydatid cyst is largely asymptomatic until complications occur. • Dyspepsia • Abdominal pain • Vomiting • Hepatomegaly are the most common symptoms.
- 42. • Jaundice and fever are each present in approximately 8% of patients. • Bacterial super infection of a hydatid cyst can occur and be manifested like a pyogenic abscess
- 43. • Rupture of the cyst into the biliary tree or bronchial tree or free rupture into the peritoneal , pleural, or pericardial cavities can occur.
- 44. Diagnosis • Serologic tests are available to evaluate antibody response, but all are plagued by low sensitivity and specifity • Ultrasound is more common, but it depends on the stage of the cyst at the time of examination
- 45. • Simple hydatid cyst is well circumscribed with budding signs on the cyst membrane • May contain free floating hyperechogenic hydatid sand • A rosette appearance is seen when daughter cysts are present
- 46. • Cyst can be filled with an amorphous mass, which can be diagnostically misleading • Calcification in the wall of the cyst is highly suggestive of hydatid disease
- 48. • Similar findings are seen on CT or MRI scans • In patients with suspected biliary involvement, ERCP or percutaneous transhepatic cholangiography may neccesary
- 49. Treatment • Primarily surgical • Most cyst should be treated • But in older patients with small, asymptomatic, densely calcified cysts, conservative management ( drainage nad evacuation) is appropriate.
- 50. • Epinephrine and steroids taken by anesthesiologist • Packing off the abdomen is important because rupture can result in anaphylaxis and diffuse seeding
- 51. • Then cyst ih aspirated through a closed suctionsystem and flushed with a scolicidal agent (hypertonic saline)
- 52. • The cyst is then unroofed which can then be followed by a number of possibilities, including • excision ( or pericystectomy) • Marsupialization procedures • Leaving the cyst open • Drainage of the cyst • Omentoplasty • Partial hepatectomy
- 53. • Pericystectomy or formal partial hepatectomy can also be performed without entering thy cyst.
- 54. • Simple suture repair is often sufficient, but major biliary repairs, approaches through the common bile duct, or postoperative ERCP may be neccesary • Recurrence rates after surgical treatment is generally 5% or less
- 55. • Preoperative treatment my decrease the risk of spillage. • Albendazole or mebendazole is effective with E.granulosus infection, but cyst appearance occurs 50% of patients • Medical treatment without resection or drainage should be considered only for widely diseminated disese or poor surgical candidate
- 56. Thank you!
Editor's Notes
- No significant difference in age, gender and ethnicity.
- Poly – cholangitis, pyelophlebitis. Single – systemic infections
- Important because of difference in treatment.
- Advantage is avoidance of general anesthesia, laparotomy, simple.
- Human contact with carrier, contaminated water food. Lyses through cell adhesion, release of enzymes, resulting in necrosis
- Can calcify
- Typically less than 10 days. Can compress biliary tree
- LFT – albumin, PT- INR, ALP, AST, bilirubin
