Functions of the kidney in 40 characters
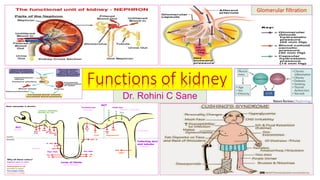
- 1. Functions of kidney Dr. Rohini C Sane Glomerular filtration
- 2. Nephron as the functional unit of kidney • Nephron is the functional unit of the kidney. • Each Kidney is composed of approximately one million nephrons. • Nephron is made of a renal capsule and renal tubule. • The renal capsule contains a thin walled sac-like structure called the Bowman's capsule into which the afferent arterioles from renal artery form a capillary network called glomerulus. • Each renal tubule consists of Proximal convoluted tubule (PCT) which dips into the renal medulla to form the Loop of Henle. The tubule reenters the renal cortex to form the Distal convoluted tubule (DCT). Several DCTs merge to form a Collecting duct. • Several Collecting tubules join and open into renal pelvis . The juxtaglomerular apparatus present between the DCT and afferent arterioles secretes renin.
- 3. Diagrammatic representation of Nephron The glomerulus has a semipermeable membrane through which substances (except cells and large molecular size plasma proteins) are filtered into Bowman ‘s capsule at a rate ( 120ml/minute).This is known as Glomerular filtration rate(GFR).
- 4. Functions of components of Nephron of kidney ❖Proximalconvolutedtubules(PCT):80%saltandwaterareabsorbedfromglomerular filtrateinproximalconvolutedtubule.Allfilteredglucoseandaminoacidsarereabsorbedin here.Lowmolecularweightproteins,urea,potassium,magnesiumandcalciumare reabsorbedtovaryingextent. ❖LoopofHenle: ▪ ThedescendingloopofHenleishighlypermeabletowater.Passivereabsorptionofwater occursleavinghighlyconcentratedurineatthebottomofloop. ▪ TheascendingloopofHenle(dilutingsegment)isrelativelyimpermeabletopassageof waterbutactivelyabsorbsNa+andCl- ions. ❖Distalconvolutedtubule(DCT):asmallfractionoffilteredsodium,chlorideandwateris reabsorbedinDCT, whichrespondstoADH,sothatitswaterpermeabilityishighinthe presenceofhormoneandlowinitsabsence. ❖Collectingtubule:ADHcontrolsthewaterpermeabilityofthecollectingtubulethroughout itslength.
- 6. Functions of kidney ❖Functions of kidney : 1. Excretion of metabolite waste products : the end products of protein and nucleic acid metabolism and metabolites of xenobiotics are eliminated from the body. (effect on blood pressure and heart) e.g. urea, creatinine, creatine , uric acid , sulphate and phosphates 2. Maintain fluid and electrolyte homoeostasis :the kidney is largely responsible for the regulation of water, electrolyte ,acid -base balance(maintenance of pH) in the body e.g. glucose , amino acids etc. 3. Endocrine Function: The kidneys also function as Endocrine organs by producing hormones: a) Renin b) Erythropoietin (effect on RBC synthesis) c) 1,25 Dihydroxycholecalciferol= Calcitriol (activation of Vitamin D –effects on bones) d) Prostaglandins (PGA 2 PGE 2 ,PGF 2 ) e) Bradykinin and Kallidin 4. Participates metabolism by retaining substances vital to body: The kidneys reabsorb and retain several substances of biochemical importance in the body . e.g. Glucose ,amino acids .
- 7. Structure and Functions of kidney
- 8. The Formation of urine • Three steps of formation of urine: 1. Glomerular filtration 2. Tubular reabsorption 3. Tubular secretion
- 9. Glomerular filtration: various ways Complete reabsorption Partial reabsorption by diffusion No reabsorption and no secretion Secretion Reference D.N. Baron Schematic diagram
- 10. The Formation of urine
- 11. Endocrine Functions of the kidney Renin: a proteolytic enzyme produced in the juxtaglomerular apparatus of the kidney . It stimulates the formation of Angiotensin II which in turn leads to Aldosterone production. Angiotensin II and Aldosterone are the hormones involved in the regulation of electrolyte balance . Angiotensin II is a powerful vasoconstrictor, that increases blood pressure and causes contraction of smooth muscles. Erythropoietin : a peptide hormone stimulates erythropoiesis in bone marrow (hemoglobin synthesis) . 1,25 Dihydroxycholecalciferol (Calcitriol ): 1-hydroxylation occurs in kidney to form the biochemically active form of vitamin D (Calcitriol). It regulates calcium absorption from the gut and homeostasis. Prostaglandins (PGA 2 PGE 2 ,PGF 2 ): are produced by renal medulla induce relaxation of smooth muscles, vasodilatation, decrease in renal pressure, increase in renal blood flow and excretion of sodium. Bradykinin and Kallidin: peptide hormones produced by the kidney. They are a powerful vasodilators that influence reabsorption of sodium and water. Bradykinin stimulates synthesis of renal Prostaglandins .Kinins also play a role in blood coagulation increase renal blood flow and exhibit antihypertensive effect . ❖Kidney possess receptors for hormones parathyroid hormone and ADH. ❖Kidney possess sites of inactivation of hormones such as insulin ,glucagon.
- 14. Glomerular filtration ❖Glomerular filtration: ➢Glomerular filtration is Passive process that results in the formation of ultrafiltrate of blood .This process occurs when blood is perfused through Bowman’s capsule . ➢Volume of blood passing through the kidneys = 1200ml/every minute(650ml plasma) : the renal flow blood . ➢Glomerular filtration rate (GFR ): 120 -125 ml blood (one tenth)filtered by the Glomerulus of kidneys every minute. ➢With normal Glomerular filtration rate (GFR)of 120 -125 ml/ minute , 175 -180 L of the Glomerular filtrate is formed per day in an adult ,out of which only 1.5 L is excreted as urine. Thus more than 99% of Glomerular filtrate is reabsorbed by the kidneys. ➢All the (unbound) constituents of plasma ,with molecular weight less than 68000 Dalton are passed into filtrate . Therefore the Glomerular filtrate is almost similar in composition to plasma . It is a protein free and cell free filtrate of whole blood but contains essential metabolites such as glucose and amino acids as well as waste products (urea , uric acid and creatinine). Albuminuria is considered as earliest manifestation of kidney dysfunction.
- 15. Factors affecting Glomerular filtration ❖ Factors affecting Glomerular filtration: A. Renal blood flow B. Passage of macromolecules is based on their Shape ,charge and size of molecules to be filtered : anionic derivatives ,globular molecules of molecular weight > 68000 Dalton are retained . The sieves of glomeruli are such that hemoglobin (molecular weight 67000) is filtered and passed into urine , while albumin is retained in the blood .Therefore ,the earliest manifestation of abnormal renal function is appearance of albumin in urine. C. Molecules less than 5KD such as glucose ,creatinine , urea and electrolytes are freely filtered by glomeruli. D. The low molecular weight proteins are freely filtered by glomeruli ,reabsorbed and catabolized by renal tubular cells. E. The normal urinary protein excretion < 150 mg /24 hr.(made up of mostly Tamm horsefall glycoprotein) .
- 16. Tests for measuring Glomerular filtration 1. Creatinine clearance Test 2. Urea clearance Tests
- 17. Glomerular filtration rate (GFR ) ❖A decease in the renal function is due to the loss of functional nephrons , rather than a decease in the function of individual nephron . ❖Glomerular filtration rate (GFR) : provides the most useful index for the assessment of the severity of renal damage. ❖Glomerular filtration rate (GFR) is the product of filtration rate in single nephron and number of nephrons in both kidneys . ❖Factors affecting Glomerular filtration rate (GFR): 1. Age( kidney function decline with age e.g. at 70 yr. of age , GFR < 60 ml/min in 25% elders) 2. Sex 3. body size 4. Protein intake 5. Pregnancy ❖Normal Glomerular filtration rate (GFR )= 120- 130ml/mt/1.73 M2 ❖Substantial kidney damage occurs before GFR is deceased .
- 18. Conditions associated with decreased Glomerular filtration rate (GFR ) ❖Decreased GFR observed in : a. Blood pressure < 60 mm b. Renal calculi* c. Enlarged prostrate * d. Old age *causes for obstruction to the renal flow
- 19. Estimated Glomerular filtration rate (eGFR )
- 20. Calculation of Estimated Glomerular filtration rate (eGFR ) Cockcroft–Gault equation for Estimated Glomerular filtration rate (eGFR ) : Ccr = (140 –age in years) x weight in kg /72 x serum creatinine ( x 0.85 in female) assuming that they have 15 % less muscle mass. ❖Estimated Glomerular filtration rate (eGFR )in ml /min / 1.73 m2 : 186 x (serum creatinine /88.4) – 1.154 x (age) – 0.203 x 0.742 (if female) ❖Estimated Glomerular filtration rate (using both equations) can be used for staging patients with chronic kidney disease neither in healthy individuals nor in children and obese . –Modification of Diet in Renal Disease –MDRD • Estimated Glomerular filtration rate (eGFR ) eliminates the need for timed urine collection. • It allows a technique of estimating creatinine clearance and thereby GFR using serum creatinine levels. • Accuracy of serum creatinine estimation is a major deciding factor in both equations.
- 21. Normal composition of urine Constituents of urine Urinary Concentration Factors affecting urinary excretion Calcium 100-250mg/dl Chloride 170-250meq/dl Creatine 100 mg/dl Creatinine 0.8 -2 g /dl( 1-2g/day) GFR,tubularsecretion,age,sex,musclemass 17-ketosteroids (adult male) 8 -20 mg/dl 17 ketosteroids (adult female) 5 -15 mg/dl Oxalic acid 20 – 40 mg/dl Phosphorous 0.5 -1.5 g/dl Urea 15-40 g/dl (15-30 g/ day) Dietaryproteins,proteincatabolism,bloodflow Uric acid 200-500mg/dl(0.5-0.8g/day) Purine catabolism, tubular excretion
- 22. Normal daily excretion of solutes Compound Total daily urinary excretion under normal dietary intake Sodium 100–200mmols 2–4g Potassium 50–70mmols 1.5–2g Magnesium 4–8mmols 0.1–0.2g Calcium 1.2–3.7mmols 0.1–0.3g Phosphate 20–50mmols 0.7–1.6g Chloride 100–250mmols 110 -125 mEq Bicarbonate 0––50mmols Sulphate(inorganic) 40–120mequ 0.6–1.8g Sulphate(organic) 0.06–0.2g urea 15–30g 6–18g Creatinine 1–2g 0.3–0.8g Uricacid 0.5–0.8g 0.08–0.2g Ammonia 30–75mequ 0.04–1g Aminoacids 0.08–0.15g
- 23. Common Biochemical tests to assess kidney functions Compound Blood levels under normal dietary intake Factors affecting urinary excretion Sodium 135 –142 mmols/L State of hydration, dietary sodium , renal functions Potassium 3.5- 5.5 mmols/L Dietary potassium , acid base balance , renal functions Calcium 9-11 mg/dL Dietary Calcium ,Calcitonin ,PTH ,renal functions , vitamin D metabolism
- 24. Glomerular Dysfunctions of Kidney ❖In Glomerular Dysfunctions of Kidney 1. Urine volume decreases 2. Specific gravity increases 3. Blood Urea increases (urea clearance decreases) 4. Serum creatinine increases (creatinine clearance decreases) 5. Inulin clearance decreases 6. PDH clearance decreases 7. Proteinuria (positive test for Protein in urine) 8. Serum phosphate increases
- 25. Tubular functions of Kidney
- 26. Tubular functions of Kidney ❖When the glomerular filtrate is formed, it contains all the crystalloids of plasma . ❖Tubular functions of Kidney include Reabsorption or Secretion of solutes and Reabsorption of water from glomerular filtrate in the proximal convoluted tubule(PCT). ❖All filtered glucose and amino acids are absorbed in PCT. ❖The descending loop of Henle is highly permeable to water .Passive reabsorption of water occurs leaving highly concentrated urine at the bottom of loop. ❖The ascending loop of Henle (diluting segment) is relatively impermeable to passage of water but actively absorbs Na+ and Cl- ions. ❖Low molecular weight proteins ,urea ,potassium , magnesium and calcium are reabsorbed to varying extent.
- 27. Biochemical Tests measuring tubular functions 1. Determination of specific gravity ,concentrating and diluting ability of kidney 2. Determination of serum and urine osmolarity 3. Determination urine ammonia 4. Phenolsulphonaphthalein (PSP)Test
- 28. Renal Tubular reabsorption ❖Tubular reabsorption : is an active process. • The renal Tubules(Proximal convoluted tubule-PCT, Distal convoluted tubule - DCT , Collecting tubules) retain water and most of the soluble constituents of Glomerular filtrate by reabsorption(active or passive process) . • A small fraction of filtered sodium , chloride and water is reabsorbed in the distal tubule which responds to antidiuretics hormone (ADH) ,so that its water permeability is high in the presence of hormone and low in its absence. • ADH controls the water permeability of the collecting tubule throughout its length of collecting tubule. • The excreted urine has an entirely different composition compared to Glomerular filtrate from which it is derived .
- 29. Renal threshold substances • Renal threshold substances : there are certain substances in the blood whose excretion in urine is dependent on their blood concentration. Such substances are referred as Renal threshold substances. • At normal concentration in the blood , they are completely reabsorbed by kidneys, with a result that their excretion in urine is almost negligible. • But when the blood levels are elevated ,the tubular reabsorption capacity is saturated ,so that excess will be excreted in urine. • High threshold substances : they are reabsorbed efficiently by kidneys (e.g . Glucose, Amino acids) • Low threshold substances : they are not reabsorbed or reabsorbed slightly by kidneys (e.g. Creatinine, Urea , Uric acid) .
- 30. Threshold value-Plasma levels of common substances excreted in urine Substance Threshold value plasma levels Glucose 180mg/dl Lactate 60 mg/dl Bicarbonate 28 mequ /L Calcium 10mg/dl The Renal Threshold of substance is the Plasma levels above which compound is excreted in urine.
- 31. Role of proximal convoluted tubule (PCT) in Renal Tubular functions Reabsorption in proximal convoluted tubule of 99 % water ( obligatory ) Uric acid (obligatory) Sodium -Na ⁺ (85% reabsorption) Chloride- Cl- (85% reabsorption) Bicarbonates (85% reabsorption) Potassium- K ⁺ (100% reabsorption) Glucose (100% reabsorption) Amino acids (100% reabsorption) Urea/phosphates - PO ⁻⁴ / Calcium Ca 2+ : are partially absorbed Secretion in proximal convoluted tubule of : H⁺ ,acids , bases, NH4⁺ , Diodrast, PAH
- 32. Role of loop of Henle in Tubular functions of kidney Reabsorption of ions in loop of Henle include : Sodium -Na ⁺ Chloride- Cl- Calcium – Ca2+ Magnesium - Mg2+
- 33. Role of distal convoluted tubule (DCT) in Tubular functions Reabsorption in distal convoluted tubule include: water (facultative) Sodium -Na ⁺ Chloride- Cl- Secretion in proximal convoluted tubule of : H⁺ , Potassium- K ⁺ , NH4⁺ , Uric acid
- 34. Tubular reabsorption Function of kidney ❖Reabsorption of water: • More than 99 % of water (187.5 liters/day) is reabsorbed by counter current multiplication or counter current exchange . • Reabsorption of water from distal convoluted tubule (DCT) and collecting ducts is facilitated by the pituitary hormone ADH. ❖Reabsorption of sodium: by symport and antiport system. ❖Reabsorption of potassium: occurs in the proximal convoluted tubule (PCT). • Reabsorption of urates: occurs in the proximal convoluted tubule (PCT) by both active and passive transport.
- 35. Tubular Functions of kidney
- 36. Renal Tubular reabsorption of water • More than 99% of water entering in Renal Tubules is reabsorbed . ❖Reabsorption of water in the PCT : 1. About 80% of water is reabsorbed . 2. Water is reabsorbed by passive transport as a solvent for actively reabsorbed sodium, chloride , bicarbonate ions and glucose (obligatory Reabsorption –water has to move along with solutes to maintain osmalality). 3. Tubular filtrate is isosmotic with plasma. ❖Reabsorption of water in the descending limb : 1. Tubular filtrate is hyperosmotic with plasma. 2. Water without solute is lost . This is termed as counter current multiplication . 3. Counter current multiplication : a. Functions in absence of antidiuretic hormone( ADH) b. is an active process that creates high medullary osmality in the Renal medulla and produces dilute urine . ❖Reabsorption of water in the ascending limb : a. sodium chloride is lost without water . b. Tubular filtrate is hypoosmotic with plasma.
- 37. Flow rates of Renal Tubular reabsorption of water Water reaches Flow rate Osmolarity Proximal convoluted tubules 125 ml /min sodium, chloride , bicarbonate ions and glucose are absorbed. Water has to move along with solutes to maintain osmality- obligatory Reabsorption Loop of Henle 25 ml/min Sodium is reabsorbed, Water reabsorption is less. Urine is hypotonic. Distal tubules 16 ml/min Water reabsorbed under influence of ADH –facultative reabsorption Collecting tubules 1 ml/min Urine is hypertonic.
- 38. Countercurrentmechanismof RenalTubularreabsorptionofwater ❖Reabsorption of water in the DCT and the collecting duct : 1. Water without solute is reabsorbed along the gradient created by counter current multiplication . 2. This is termed as counter current exchange . 3. Counter current exchange : a. is facilitated by antidiuretic hormone(ADH). ADH secretion in turn, is controlled by hypothalamic osmoreceptors. The osmolality of plasma is the stimulus for modulating ADH secretion. b. concentrates the urine.
- 39. Factors influencing ADH secretion ❖Factors influencing ADH secretion include : • Osmotic pressure of the blood: Osmoreceptors in the hypothalamus that are sensitive to changes in the Osmotic pressure of the blood influence the synthesis and secretion of ADH. • Blood volume: volume receptors in the carotid sinus and left atrium influence ADH secretion. • An increase in Osmotic pressure of the blood or decrease in blood volume stimulates ADH secretion.
- 40. Osmoreceptors in the hypothalamus Osmoreceptors in the hypothalamus that are sensitive to changes in the Osmotic pressure of the blood influence the synthesis and secretion of ADH.
- 41. Renal Tubular reabsorption of sodium • Tubular reabsorption of sodium occurs in Proximal convoluted tubule-PCT by two types of cotransport systems. ❖Symport system :which involves cotransport of sodium along with other substances such as glucose ,amino acids and phosphates .It is catalyzed by Na+ _ K + ATP ase present in basolateral plasma membrane of the epithelial cells . • This creates sodium gradient that accomplishes active transport of sodium out of the cell while potassium enters the cell. • There is passive transport of equivalent amount of chloride to maintain electrical neutrality. • The net effect is the reabsorption of sodium chloride along with glucose and amino acids etc. ❖Antiport system : involve exchange of sodium (reabsorbed) for another cation such as H + as in Na+ -H +. This also achieves a net reabsorption of bicarbonate. When hydrogen ions are to be conserved ,sodium to potassium exchange occurs .
- 42. Symport system for Renal Tubular reabsorption of sodium Symportsystem:whichinvolvescotransportofsodiumalongwithothersubstancessuchasglucose,amino acidsandphosphates.Itis iscatalyzedbyNa+ –K+ ATPase presentinbasolateralplasmamembraneofthe epithelialcells.
- 43. Renal Tubular reabsorption of Glucose • Normally Glucose is reabsorbed completely . • The maximum rate at which Glucose is reabsorbed , referred as the Tubular maximum for glucose(TmG)= 350 mg/min. • When blood Glucose exceeds renal threshold for Glucose which is 10mmols/L or (180mg/dl) , glucose spills over into the urine (glycosuria) . • Water is excreted as a solvent for glucose (osmotic diuresis).
- 44. Renal Tubular reabsorption of Calcium ❖Tubular reabsorption of Calcium : • About 90% of Calcium is reabsorbed from the glomerular filtrate. • Regulation of calcium balance is achieved at the distal convoluted tubule . • Factors regulating calcium reabsorption: parathyroid hormone and vitamin D.
- 45. Renal Tubular reabsorption of Uric Acid • Uric Acid is completely reabsorbed in Proximal convoluted tubule-PCT, by both active and passive mediated process . • There is an active secretion of Uric Acid in the tubules . About 85% of the excreted Uric Acid is derived by tubular secretion. • The drug ,probenecid is secreted by the tubules and competes with Uric Acid for reabsorption . Since probenecid increases Uric Acid excretion ,it is uricosuric.
- 46. Renal Tubular reabsorption of Urea • Urea is freely filtered by the glomerulus ,but about the 40% is reabsorbed actively by the tubules. • Rate of reabsorption of Urea varies inversely with tubular flow and accounts for the elevation of blood urea when renal function is low. • Concentration of Urea in urine = 70x concentration of Urea in plasma • Urea forms 80% of total urinary solutes . • Urine is roughly a 2 % solution of Urea.
- 47. Renal Tubular reabsorption of Potassium • 70% of potassium in glomerular filtrate is reabsorbed by Proximal convoluted tubule-PCT. • Net secretion of potassium at the distal tubules ,in exchange for sodium reabsorption , under the effect of aldosterone. • However when H + concertation is increased, H + ions are exchanged for sodium instead of potassium.
- 48. Mechanism of action of diuretics :1 Diuretics Mechanism of action of diuretics Site of action Mannitol Osmotic diuretics act by interfering with reabsorption of solutes so that more water is obligatory excreted along with the solutes . PCT Acetazolamide A carbonic anhydrase inhibitor-the dissociation of H2CO3 to H2O and CO2 is inhibited →decreased reabsorption of bicarbonate ,sodium and water . PCT Thiazide decreased reabsorption of sodium and more water is excreted obligatorily . DCT Frusemide Inhibits reabsorption of chloride , sodium and water (chances for potassium depletion) . Ascending limp of loop of Henle Spironolactone (K+ sparing ) Aldosterone antagonist DCT
- 49. Mechanism of action of diuretics:2
- 50. Mechanism of action of diuretics:3
- 51. Reabsorption ,secretion and excretion of substances by kidney Parameter Reabsorption Secretion Excretion/relative concentration Creatinine Nil Nil GF = URINE Uric acid 70 % by proximal convoluted tubules (PCT) by distal convoluted tubules( DCT) GF URINE Urea 40 % by PCT Nil GF > URINE Sodium ( Na ⁺) Partial Nil GF > URINE Glucose Complete Nil GF >> URINE Amino acids Complete Nil GF >> URINE
- 52. Tubular maximum • Tubular maximum (Tm): is used to indicate maximum capacity of kidneys to absorb a particular substance . • e.g. Tubular maximum for glucose (TmG) : 350 mg/min
- 53. Defects in Renal Tubular reabsorption • Renal glycosuria in which glucose appears in urine despite of normal plasma glucose levels . • Vitamin D resistant rickets : in which phosphates reabsorption is defective . • De Toni Fanconi syndrome: is associated with glycosuria, phosphaturia and Renal Tubular acidosis. • Renal Amino aciduria : as in Fanconi syndrome and cystinosis .
- 55. Tubular secretion in kidney ❖Tubular secretion in kidney : ❖substances actively secreted by renal tubular cells include: a) Endogenous substances( e.g. hippuric acid ,bile salts ,urates) b) Exogenous substances( e.g. diuretics , salicylates ,p- amino Hippurate, penicillin ) ❖ Creatinine : is secreted when plasma levels increase above normal levels . ❖Potassium : is secreted in the DCT in exchange for sodium reabsorbed. ❖Aldosterone favors sodium reabsorption and excretion of Potassium. ❖Primary aldosteronism (excessive Aldosterone) : there is excessive excretion of Potassium and retention of sodium. ❖Addison’s disease (deficiency of Aldosterone) : sodium excreted and Potassium retained in excess .
- 56. Addison’s disease and Cushing's syndrome Addison’sdisease(deficiencyofAldosterone) :sodiumexcretedandPotassiumretainedin excess. Primaryaldosteronism(excessive Aldosterone): thereisexcessiveexcretionof Potassiumandretentionofsodium.
- 57. Addison’s disease-bronze pigmentation Addison’s disease (deficiency of Aldosterone) : sodium excreted and Potassium retained in excess .
- 58. Tubular secretory mass in kidney • Tubular secretory mass : mass of functioning Tubular mass can be assessed by measuring the tubular maximum for PAH(Tm PAH). Tm = UV/P X GFR For PAH ,the Tm is 76 mg/minute.
- 59. Tubular Dysfunctions of Kidney ❖In Tubular Dysfunctions of Kidney: 1. Urine volume increases 2. Urine concentration decreases 3. Specific gravity decreases 4. Serum uric acid increases (uric acid excretion decreases) 5. Acidification of urine decreases 6. Amino aciduria present 7. Serum phosphate decreases 8. Urine dilution test abnormal
- 60. SummaryofkidneyfunctiontestsinGlomerularandtubulardysfunction Glomerular dysfunction observation Tubular dysfunction observation Serum urea Increased Urine concentration decreased Serum creatinine Increased Dilution test Abnormal Serum phosphate decreased Serum phosphate decreased Inulin clearance decreased Uric acid excretion decreased Creatinine clearance decreased Blood Uric acid Increased Urea clearance decreased Acidification of urine Decreased PAH clearance decreased Proteinuria Present Aminoaciduria Present Urine volume Decreased Urine volume Increased Specific gravity Increased Specific gravity decreased
- 61. Biochemical parameters based on renal functions Renal function Biochemical Parameters Excretory function NPN –plasma levels of Urea ,Creatinine, Uric acid Endocrine function Hemoglobin ,Serum calcium , Serum Phosphorus Homeostasis (acid -base balance) Blood pH , Serum Electrolytes ( Sodium, Potassium ,chlorides) Serum Bicarbonate, Serum Calcium and Inorganic phosphorous , Blood gases ( PO2 , PCO2)