Fluoroquinolones
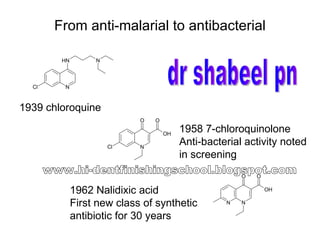
- 1. From anti-malarial to antibacterial 1939 chloroquine 1958 7-chloroquinolone Anti-bacterial activity noted in screening 1962 Nalidixic acid First new class of synthetic antibiotic for 30 years dr shabeel pn www.hi-dentfinishingschool.blogspot.com
- 2. Mechanism of action topo-isomerase relaxed supercoiled gyrase Inhibition of topoisomerases – a family of enzymes responsible for maintaining the topology of DNA
- 3. Quinolones form a Quaternary Complex between Protein, DNA and Neighbouring Quinolones
- 4. Accumulation of Covalent Complexes and Broken DNA is Lethal Target is gyrase (Gram-negative) and/or topisomerase IV (Gram-positive) Killing is rapid but reaches a plateau (60-120‘ for 10 4 -fold decrease in viable count) Killing antagonized by inhibitors of translation and at high FQ concentration „Eagle effect“) Anaerobic conditions inhibit action
- 5. Concentration Dependence of Killing Concentration dependence shows two phases of inhibition, separated by a plateau. The cultures in the plateau region give rise to first step resistant mutants. Mutants are not recovered above the onset of the second sharp drop. This limit is defined as the mutant preventing concentration (MPC). MPC
- 6. Early Quinolone Antibiotics Nalidixic Acid 1962 Sterling Winthrop Oxolinic Acid 1967 Werner Lambert Pipemidic Acid 1974 Roger Bellon Cinoxacin 1974 Lilly Flumequine 1973 Rikker Labs Rosoxacin 1976 Sterling Winthrop
- 7. Potential of Early Quinolone Antibiotics Nalidixic Acid Enterobacteriaceae Short half-life (not P. aeruginosa ) (1.5 hr) high protein binding Pipemidic Acid Broader Gram-negative Longer half-life spectrum (except Serratia ) Oxolinic Acid Weak but broad lower protein binding Gram-negative Flumequine Weak but broad Gram-negative
- 8. The First Fluoroquinolone Antibiotics Flumequine 1973 Rikker Labs Pipemidic Acid 1974 Roger Bellon Norfloxacin 1978 Kyorin Broad Gram-negative spectrum (F, morpholino grp) Less protein binding, 50% (quinolone not naphthyridine) Longer half life, 3h (morpholino group)
- 9. The First Generation of Fluoroquinolone Antibiotics Flumequine 1973 Rikker Labs Norfloxacin 1978 Kyorin Pefloxacin 1979 Dainippon Ofloxacin 1979 Daiichi Ciprofloxacin 1983 Bayer Fleroxacin 1987 Roche
- 10. Potential of the First Generation Fluoroquinolone Antibiotics Gram-negative spectrum t 1/2 (h) Flumequine Weak but broad Norfloxacin Strong 3 - 4 Pefloxacin Weak 11 Ofloxacin Strong 6 Ciprofloxcin Very strong 3 – 4 Levofloxacin Extremely strong 6 “ Also rans“ Amifloxacin 1984 Sterling Winthrop Fleroxacin 1987 Roche Lomefloxacin 1988 Searle
- 11. From Ofloxacin to Levofloxacin Ofloxacin 1979 Daiichi Racemic mixture Levofloxacin 1987 Daiichi Pure (-) S isomer Active component of ofloxacin 2-fold improved activity Extended patent life
- 12. The Later Fluoroquinolone Antibiotics Difloxacin 1986 Abbott Temafloxacin 1988 Abbott Sparfloxacin 1991 Rhone-Poulenc-Rorer (Dainippon 1985) Grepafloxacin 1995 Otskuda (1989) Gatifloxacin 1993 Kyorin (1988) Moxifloxacin 1994 Bayer
- 14. Later Naphthyridines Flumequine 1973 Rikker Labs Pipemidic Acid 1974 Roger Bellon Enoxacin 1984 Rhone-Poulenc Rorer Trovafloxacin 1993 Pfizer Temafloxacin 1988 Abbott Ciprofloxacin 1983 Bayer Gemifloxacin 1994 L G Chemicals
- 15. Later Naphthyridines Gram –ve Gram +ve Anaerobes ( E. coli ) ( S. pneumoniae ) ( B. fragilis ) Pipemidic Acid 0.025 – 16 4 – > 64 > 64 Enoxacin 0.025 – 16 1.6 - 16 Trovafloxacin 0.008 - 1 0.007 – 0.25 0.128 - 8 Gemifloxacin 0.5 - 64 Ciprofloxacin 0.125 – 0.5 0.5 - 2 2 - 128
- 16. Current Uses of Fluoroquinolones Ciprofloxacin: wide range of infections pneumonias, bone infections, diarrhea, skin infections and urinary tract infections. Not good for methicillin resistant Staphylococcus aureus Norfloxacin: better for UTI effective against Gram-negative (including Pseudomonas aeruginosa) and Gram-positive UTIs and prostatitis, but not in systemic infections Lomefloxacin and enoxacin -- UTIs and bronchitis caused by Haemophilus influenzae or Moraxella catarrhalis . Lomefloxacin not effective against pseudomonal bacteremia. Enoxacin recommended for STDs Moxifloxacin – overcomes the problems with S. pneumoniae Acute bacterial sinusitis; mild to moderate community-acquired pneumonia
- 17. Frequent Side Effects of Quinolones Chelation of cations (Fe 3+ , Al 3+ , Mg 2+ , Ca 2+ ) incompatibility with antacids Phototoxicity Drug interactions (inhibition of cytochrome P 450 ) Ciprofloxacin and enoxacin interfere with hepatic biotransformation -- may cause toxicity due to excess of e.g. theophylline, warfarin CNS toxicity (GABA receptor antagonist) all quinolones contraindicated in patients with history of convulsions Gastro-intestinal discomfort nausea or vomiting, abdominal or stomach pain Cartilage and musculosqueletal pathogenicity have caused arthralgias and joint swelling in children Achilles tendinitis and tendon rupture 2 - 42 days after start of therapy Bacterial SOS response to DNA and other damage caused by FQ may induce toxins . (E. coli, S. typhimurium, B. anthracis)
- 18. Rare Side Effects of Quinolones Nephrotoxicity crystalluria, hematuria, interstitial nephritis, acute renal failure Cardiac toxicity inhibition of hERG channel leads to QT prolongation & torsades de pointe Hepatotoxicity temafloxacin syndrome, trovafloxacin syndrome
- 19. Frequent Side Effects of Quinolones Cation complexation all quinolones Photoxicity: especially F fleroxacin, lomefloxacin, sparfloxacin Inhibition of CyP 450 ciprofloxacin, gemifloxacin CyP 450 inhibition GABA receptor binding& CNS penetration
- 20. Nephrotoxicity crystalluria, hematuria, interstitial nephritis, acute renal failure Poor solubility can lead to crystallization of the FQ in concentrated urea. Needle-like crystals form that can cause mechanical damage
- 21. Cardiac Toxicity Torsades de pointe : paroxysm of ventricular tachycardia in which the electrocardiogem shows a steady undulation in the QRS axis in runs of 5 to 20 beats with progessive changes in direction. It is a most severe type of arythmia and can result in death. It is most often associated with and preceeded by a prolongation of the QT interval. Population at risk QT greater than 20 ms Moxifloxacin 7 ms, grepafloxacin 10 ms, sparfloxacin 15 ms
- 22. Hepatotoxicity Temafloxacin syndrome Hemolytic uraemic anemia discoloured urine fever jaundice nausea, vomiting coagulopathy hepatic dysfunction renal dysfunction 0.56% incidence 2 deaths Withdrawn June 1992 Trovafloxacin syndrome Serious hepatic events laboratory abnormalities encephalopathies nectrotic inflammation 0.0056 % incidence 5 transplants 6 deaths Withdrawn/limited in June 1999
- 23. Resistance to Quinolones Point mutations in the gyrase A gene cluster in region around tyrosine 122, site of covalent attachment of DNA Point mutations in the regulatory regions of transport proteins porins of Gram-negative bacteria efflux systems of P. aeruginosa (mex systems) Enterobacteriaceae (Acr system + porin mutation) S. aureus (norA system) S. pneumoniae (pmrA system, patAB system) No transferable resistances recorded until 1994: wild type susceptible genes tend to be dominant plasmid conjugation is inhibited by quinolones plasmids can be eliminated from bacteria at sub-lethal quinolone concentrations The new plasmid pMG255 encodes a putative quinolone binding protein.
- 25. Acr System of Enterobacteriaceae Multi-drug resistance efflux system. System. Pumps a broad range of antibiotics out of the cell. Part of a multicomponent system that spans cytoplasmic and outer membrane of Gram-negative bacteria. Cytoplasmic membrane component acts as energy transducer (pmf) as well As substrate recognition module
- 26. Acr System of Enterobacteriaceae
- 27. Modelled Structure of Mex/OprM Efflux Pump MexA,B-OprM exports quinolones, tetracycline, chloramphenicol and other antibiotics MexC,D-OprJ MexX,Y-OprM exports aminoglycoside antibiotics (amikacin, tobramycin) and quinolones Efflux pump inhibitors developed by Essential Therapeutics are in clinical trials as combination partner for levofloxacin
- 29. The NorA protein is an efflux transporter similar to the well-known tetracycline resistance systems It uses the proton-motive force to drive out the antibiotic against its concentration gradient by proton-coupled antiport. FQ FQ FQ H + H + H + Intrinsic FQ resistance in streptococci reported to be due to a homologue the PmrA protein Efflux-mediated Resistance in Streptoocci
- 30. Major Facilitator Family Permeases
- 31. ABC transporters Implicated in fluoroquinolone resistance in streptococci (PatA, PatB) Multi-drug resistance in many Gram-positive organisms
- 34. Induction of patA and patB : microarray data patA patB M4 M22 After 10 mins exposure to ciprofloxacin
- 35. Effect of inactivating patB Recent data with M22 patA and patB inactivated with magellen2 revealed full reversal of MDR. MICs in the presence of reserpine in brackets 16 ( 1 ) 32 ( 4 ) 4 ( 1 ) 20 ( 16 ) M22 patB :: cat 12 ( 1 ) 2 ( 0.5 ) CIP 16 ( 2 ) 32 ( 4 ) 32 ( 16 ) M22 4 ( 1 ) 2 ( 0.5 ) 4 ( 2 ) M4 ACR EtBr NOR
