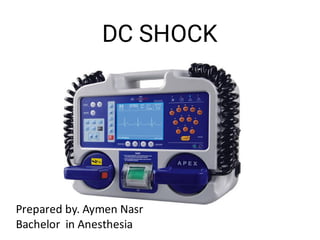
Dc shock
- 1. DC SHOCK Prepared by. Aymen Nasr Bachelor in Anesthesia
- 2. Types of shock 1 .defibrillation 2 cardioversion
- 3. Defibrillation • • • • is a common treatment for life-threatening cardiac dysrhythmias, ventricular fibrilla on and pulseless ventricular tachycardia Defibrilla on consists of delivering a therapeu c dose of electrical energy to the heart with a device called a defibrillator External depolariza on of the heart to stop Vfib or Vtach that has not responded to other maneuvers
- 4. Need for a defibrillator “ Defibrillation” – Definitive treatment of life threatening cardiac arrhythmias – VENTRICULAR FIBRILLATION PULSELESS VENTRICULAR TACHYCARDIA Ventricular fibrillation- Irregular contraction of muscle fibres Ineffec ve pumping of blood from le ventricle Steep fall in Cardiac output
- 6. Indications for Cardioversion a) Supraventricular Tachycardia b) Atrial fibrilla on c) Atrial flu er d) Ventricular Tachycardia with pulse
- 10. Types of defibrillators • • • Manual external defibrillator Automated external defibrillator (AED) Implantable cardiac defibrillator (ICD)
- 11. Automated external defibrillatorA unit based on computer technology and designed to analyze the heart rhythm itself, and then advise whether a shock is required or not. Designed to be used by lay persons, who require little training. Usually limited in the treatment of VF and VT rhythms. Usually take time ( around 5-10 secs) in diagnosing the rhythm Can be found in places like corporate and government offices, shopping centers, airports, restaurants, sports stadiums, schools and universi es, community centers, fitness centers and health
- 12. Automated external defibrillator Require self-adhesive electrodes(pads) instead of handheld paddles The ECG signal acquired from self adhesive electrodes usually contains less noise and has higher quality ⇒allows faster and more accurate analysis of the ECG ⇒be er shock decisions “Hands off” defibrilla on - safer procedure for the operator, especially if the operator has li le or no training
- 15. Implantable cardiac defibrillator An electronic device that constantly monitors heart rate and rhythm. When it detects a very fast, abnormal rhythm, it delivers energy to the heart muscle. This causes the heart to beat in a normal rhythm again. Used for cardioversion, defibrillation, anti-tachycardia pacing & bradycardia pacing. 2 parts : a)The leads b)The pulse generator
- 16. Manual external defibrillator DC defibrillator Clinician decides what charge has to be set, depending on prior knowledge and experience Shock will be delivered through paddles applied to the pa ent’s chest. Found in hospitals & ambulances
- 21. position • • • Anterior-lateral posi on ---- one – right of sternum below clavicle (2nd & 3rd ICS) other – le 4th or 5th ICS mid axillary line " Alterna vely anterior posterior may be used: one paddle is placed in the le infrascapular region while the other is placed in the le 5th- 6th intercoastal space anterior axillary line.
- 22. Paddle Size - Adult – large paddles 10-13 cm diameter - Pediatric – small paddles <1yr Infant <10kgs – 4.5cm Children >10kgs – 8cm
- 23. General Safety • Yourself, other staff – Dry surface area – Oxygen • Chest wall – GTN patch – Jewellery – Paddles / Pads not touching • Technique – One Person – Two Person – Adhesive Pads
- 24. Steps of Defibrillation Give 2min CPR before analysis. Power on ADE A ach electrode pad. Check rhythm. CLEAR. Give shock(120-200J) Resume CPR for 2mins before analysis cardiac rhythm again. Consider giving – vasopressors / an -arrhythmic‟s during subsequent shock
- 25. Steps of cardiovertion • • • • • • • • - Check environment at procedure site - Turn on defibrillator - Anaesthe c technique as required - Apply electrodes - Press SYNC control - Select applica onenergy level - „3 clear‟ shout & look - Deliver shock
- 26. How to DC shock Get Crash cart ready Turn on the machine and a ach adhesive electrodes (efficacy may be be er with anterior posterior electrodes) Choose the energy level. IV-O2 -Monitor - Get a clearly visible trace on the monitor - eg, using lead II. Hit the 'sync' bu on - usually a blip or dot appears on the monitor, marking each QRS complex. Higher star ng energy is associated with be er success and fewer shocks Broad complex tachycardia and AF: monophasic - begin with 200 J, or biphasic - 120-150 J. Atrial flu er and narrow complex tachycardia: monophasic - 100 J, or biphasic - 70-120 J.Charge.
- 27. How to DC shock - Ensure all is clear around the bed including Oxygen Discharge or shock - there may be a 1- to 2-second delay as the machine ensures synchronisa on -Check rhythm a er the shock - if sinus rhythm, then stop; if not, then you may need to deliver another shock at higher energy levels. Look for burns a erwards and obtain a 12-lead ECG. Sync may not be successful in tachycardias where the QRS complex has a variable morphology.
- 28. Post Procedure Monitoring • • • • • • • • Monitor that pa ent stay in converted rhythm. Keep pa ent well oxygenated.(SPO2 >98%) Check serum K+ & Mg+ levels. Maintain acid base balance. Get 12 lead ECG a er procedure. Check for chest pain & access. Get CPK & Troponin done. Access pa ents skin.
- 29. Post Procedure Monitoring • • • • • - Record delivery energy & result - If successful response check for peripheral pulses, BP, Airway patency - Inspect skin under the padds - If not successful, check & reassess
- 30. Complications Most common- Harmless arhhythmias like atrial/ventricular premature beats. Serious complications : a) ventricular fibrilla on b) Thrombo-embolisa on c) Myocardial necrosis d) Myocardial stunning e) Pulmonary edema f) Painful skin burns
- 31. Contra-indications • • • • Any arrhythmia with enhanced automaticity like Catecholamine induced tachycardia Digitalis toxicity induced arrhythmias Multi focal atrial tachycardia
- 32. Daily low energy test Step 1 : Put the defibrillator on Battery mode and ensure machine is disconnected from the AC power supply . Turn the selector switch to ON and select Manual mode Select leads to PADDLES/PADS Step 2 : Ensure the universal cable is connected to the paddles Place paddles in paddle wells Step 3 : Select the ENERGY to 30 J Step 4 : Press the CHARGE button Step 5 : The unit charges to 30J, then the red LED charge indicator illuminates and the charge tone sounds
- 33. Daily low energy test • • • • • • Step 6 : Ensure DEFIB 30J READY displays on screen Step 7 : Press and hold both paddles SHOCK buttons Step 8 : The unit discharges. The TEST OK message displays and the red LED turns off Step 9 : The above TEST OK message conforms that low energy circuits are in proper working condi on
- 34. Thank you so much.
- 35. Synchronized cardioversion • is a LOW ENERGY SHOCK that uses a sensor to deliver electricity that is synchronized with the peak of the QRS complex (the highest point of the R- wave). When the “sync” op on is engaged on a defibrillator and the shock bu on pushed, there will be a delay in the shock. During this delay, the machine reads and synchronizes with the pa ents ECG rhythm. This occurs so that the shock can be delivered with or just a er the peak of the R-wave in the pa ents QRS complex.
- 36. • Synchroniza on avoids the delivery of a LOW ENERGY shock during cardiac repolariza on (t-wave) . If the shock occurs on the t-wave (during repolariza on), there is a high likelihood that the shock can precipitate VF (Ventricular Fibrilla on).
- 37. indications for synchronized • The most common indica ons for synchronized cardioversion are unstable atrial fibrilla on, atrial flu er, atrial tachycardia, and supraventricular tachycardias. If medica ons fail in the stable pa ent with the before men oned arrhythmias, synchronized cardioversion will most likely be indicated.
- 38. Unsynchronized cardioversion • (defibrilla on) is a HIGH ENERGY shock which is delivered as soon as the shock bu on is pushed on a defibrillator. This means that the shock may fall randomly anywhere within the cardiac cycle (QRS complex). Unsynchronized cardioversion (defibrilla on) is used when there is no coordinated intrinsic electrical ac vity in the heart (pulseless VT/ VF) or the defibrillator fails to synchronize in an unstable pa ent.
- 39. • For cases where electrical shock is needed, if the pa ent is unstable, and you can see a QRS-t complex use (LOW ENERGY) synchronized cardioversion. If the pa ent is pulseless, or if the pa ent is unstable and the defibrillator will not synchronize, use (HIGH ENERGY) unsynchronized cardioversion (defibrilla on).
- 40. Defibrillator Wave forms • • • • • • Monophasic wave form : Energy is delivered through the patient’s chest in a “single direc on” Biphasic wave form : Energy is delivered through the patient’s chest in two direc ons. Low-energy biphasic shocks may be as effective as higher-energy monophasic shocks
- 43. References ACC/AHA Guidelines 2015 for adult advanced cardiac life support David J Williams, Fiona J Mc Gill. Physical principles of defibrillator, Anesthesia and intensive care medicine; 2003. LL Bossaert. Fibrillation and defibrillation of heart : British journal of anesthesia 1997 ;79:203-213 Kundra P, Vishnu Prasad PS, Padmavathi V, Siva T. Defibrillator maintenance policy. Indian J Anaesth 2015;59:685-7. drvenugopalpp@gmail.comwww.drvenu.blogspot.com91 9847054747
