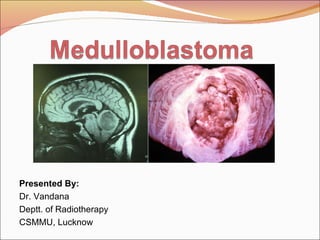
Diagnosis, Treatment & Management of Medulloblastoma
- 1. Presented By: Dr. Vandana Deptt. of Radiotherapy CSMMU, Lucknow
- 7. Adult vs. Paediatric Medulloblastoma Child Adult Usual age ~ 4 - 8 yrs Median age ~ 24 - 30 yrs Shorter clinical History (~ 3 months) Longer history ( ~ 5 months) Classical type predominates Desmoplastic type relatively commoner Median cerebellar syndrome predominates Lateral cerebellar syndrome seen Biologically more agressive Biologically less aggressive Poorer resectability - median location Greater resectability - lateral location Higher surgical morbidity and mortality Lower surgical morbidity and mortality - impact of location and age Poorer RT tolerance Better RT tolerance Poorer long term survival Better long term survival
- 8. Natural History Arising in the midline cerebellar vermis (roof of the 4 th ventricle) Grows into the 4 th ventricle Fills into the 4 th ventricle Spread around the 4 th ventricle Invasion of ventricular floor Invasion of brain stem Invasion of brachium pontis CSF Spread Extra neural spread :Y oung age, males and diffuse subarachnoid disease
- 13. Chang Surgical classification 1969 T1 Tumour < 3 cm in diameter and limited to classic position in vermis, roof of fourth ventricle, or cerebellar hemisphere T2 Tumour > 3 cm in diameter and further invading one adjacent structure or partially filling the fourth ventricle T3a Tumour further invading two adjacent structures or completely filling the fourth ventricle, with extensions into aqueduct or foramina of Magendie or Luschka with marked internal hydrocephalus T3b Tumour arising from the floor of fourth ventricle or brain stem and filling the fourth ventricle T4 Tumour penetrates aqueduct to involve third ventricle or midbrain or extends to cervical cord No N Stage M0 No metastases M1 Microscopic evidence of tumour cells in CSF. M2 Macroscopic metastases in cerebellar and/or cerebral subarachnoid space and/or supratentorial ventricular system M3 Macroscopic metastases to spinal subarachnoidal space M4 Metastases outside the central nervous system
- 20. Fig: ( B, ) non-contrast axial T1-weighted (C,) T2-weighted MR images; the solid portion of the tumor appears mildly hypointense on T1-weighting and mildly hyperintense on T2-weighting ( arrow ). Following intravenous gadolinium, an axial T1-weighted image ( D, ) demonstrates irregular patchy contrast enhancement of the solid areas of the tumor ( arrow ).
- 44. Collimator rotation : While treating cranial field rotate Collimator of lateral field so that its inferior border is parallel to divergence of sup. Aspect of spinal field . θ Collimator rotation allows cranial field to match spinal field divergence Coll θ = arc tan ( L1 /2 x SSD ) For Co 60 SSD = 80 Zone of overlap of spinal field if collimator rotation is not applied in cranial field SSD L1
- 46. COUCH ROTATION Couch θ = arc tan ( L2/2 x SAD ) For Co 60 SAD = 80 L2 ( Length of cranial field) Cranial field SAD Zone of overlap Spinal field Couch rotation during treatment of cranial field θ
- 49. Half Beam Blocking Actual Field Length Spinal field
Editor's Notes
- medulloblastoma 09/30/11 Csi
