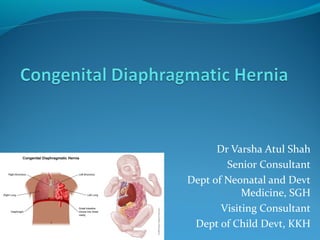
Congenital diaphragmatic hernia by Dr. Varsha Atul Shah
- 1. Dr Varsha Atul Shah Senior Consultant Dept of Neonatal and Devt Medicine, SGH Visiting Consultant Dept of Child Devt, KKH
- 2. Summary of presentation Overview - Background - Path physiology - Epidemiology - Mortality and Morbidity Clinical Presentation Differential diagnosis Investigations Treatment: Medical and surgical Follow up care
- 3. Overview appeared in the medical literature since its first description in the early 18th century18th century In 1946, Gross reported the first successful repair of a neonatal diaphragmatic hernia In the 1960s, Areechon and Reid observed that the high mortality rate of CDH was related to the degree of pulmonary hypoplasia at birth
- 4. Incidence 1 in 2000-3000 live births1 in 2000-3000 live births Accounts for 8% of all major congenital anomalies The risk of recurrence of isolated (ie, nonsyndromic) in future siblings is approximately 2% Familial is rare (< 2% of all cases) Both autosomal recessive and autosomal dominant patterns of inheritance is reported
- 5. Genetic anomalies-Syndrome Associated with genetic anomalies: Smith-Lemli-Opitz syndrome DiGeorge syndrome Chromosome 15,18,13 and 21 anomalies Fryns syndrome Pallister-Killian syndrome
- 6. Pathophysiology and cause Cause is unknown Failure of normal closure of the pleuroperitoneal canal in the developing embryo Abdominal contents herniate and compress the ipsilateral developing lung, causing pulmonary hypoplasia and hypertension
- 7. Path physiology of CDH Is associated with variable degree of pulmonary hypoplasiapulmonary hypoplasia due to decrease in cross-sectional area of the pulmonary vasculature and alterations of the surfactant systemalterations of the surfactant system The lungs have a small alveolar capillary membranesmall alveolar capillary membrane for gas exchange, which may be further decreased by surfactant dysfunction There is increased muscularizationincreased muscularization of the intraacinar pulmonary arteries In very severe cases, left ventricular hypoplasia is observed. Pulmonary capillary blood flow is decreasedPulmonary capillary blood flow is decreased because of the small cross-sectional area of the pulmonary vascular bed, and flow may be further decreased by abnormal pulmonary vasoconstriction.
- 8. Types of congenital diaphragmatic hernia Bochdalek hernia:Bochdalek hernia: Poster lateral (occurring at approximately 6 weeks' gestation) Morgagni hernia:Morgagni hernia: Anteriomedial The hiatus hernia
- 9. Left sided of CDH The left-sided Bochdalek hernia occurs in approximately 85% of cases85% of cases Allow herniation of both the small and large bowel and intra-abdominal solid organs (stomach, liver) into the thoracic cavity
- 10. Right sided CDH Occurs in (13% of cases) Only the liver and a portion of the large bowel tend to herniate Bilateral hernias are uncommon and are usually fatal.
- 11. Mortality/Morbidity Mortality has traditionally been difficult to determine This is partially because of the "hidden mortalityhidden mortality" for this condition who die in utero or shortly after birth, prior to transfer to a surgical site A population-based study from Western Australia indicated that only 61% of infants with congenital diaphragmatic hernia are live born Nearly 33% of pregnancies that involved a fetus were electively terminated Mortality is reported to range from 40-62%40-62%
- 12. Sex It occurs equallyequally in both sexes Age It is usually a disorder of the new-bornnew-born period 10% of patients may present after the new-born period and even during adulthood Outcome in patients with late presentation of congenital diaphragmatic hernia is extremely good, with low or no mortality
- 13. Clinical Presentation History Is diagnosed based on prenatal ultrasonographyprenatal ultrasonography findings in approximately one half of affected infants May have a prenatal history of polyhydramniospolyhydramnios The most commonly present with respiratory distress and cyanosis in the first minutes or hours of life The respiratory distress can be severe and may be associated with circulatory insufficiency, requiring aggressive resuscitative measures.
- 14. Antenatal Diagnosis: 59% antenatal detection with average age 24.2 weeks24.2 weeks Polyhydramnios Intrathoracic stomach or liver Lung-to-head ratio and lung/transverse thorax ratio. Usually at prenatal ultrasound (15 weeks).(15 weeks). Recently fetal MRI and fetal echocardiography, helpful to determine degree of pulmonary hypoplasia. (MRI lung volumetry, left ventricular mass and pulmonary artery diameter)
- 15. Clinical Presentation HistoryHistory Respiratory distress Tachypnea Cyanosis in the first minutes or hours of life The respiratory distress can be severe and may be associated with circulatory insufficiency, requiring aggressive resuscitative measures.
- 16. Three general presentations Severe respiratory distressSevere respiratory distress at the time of birth. ( Severe hypoplasia) Respiratory deterioration hours after delivery (honeymoon period). Benefit from correction of hypoxemia and pulmonary hypertension. Feeding difficulties, chronic respiratory disease, pneumonia, intestinal obstruction 24h after birth. (10- 20% of patients).Best prognosis
- 17. Physical Examination Scaphoid abdomen, barrel-shaped chest,Scaphoid abdomen, barrel-shaped chest, and signs of respiratory distress (retractions, cyanosis, grunting respirations) In left-sided posterolateral hernia, auscultation of the lungs reveals poor air entry on the left, peristalsis heard in chest, with a shift of cardiac sounds over the right chest In patients with severe defects, signs of pneumothorax (poor air entry, poor perfusion) may also be found Associated anomalies occur in a relatively high percentage of infants Dysmorphisms such as craniofacial, extremity abnormalities, or spinal dysraphism may suggest syndromic congenital diaphragmatic hernia
- 18. Differential Diagnoses Cystic Adenomatoid Malformation Bronchopulmonary sequestration Bronchogenic cyst Bronchial atresia Enteric cyst Teratoma Disorders of the Thoracic Cavity and Pleura Pneumothorax Primary Pulmonary Hypertension of New-born (PPHN)
- 19. Imagining study-Chest X-ray Placement of an orogastric tubePlacement of an orogastric tube prior to the study helps decompress the stomach and helps determine whether the tube is positioned above or below the diaphragm Typical findings in a left-sided posterolateral congenital diaphragmatic hernia include - Air-filled or fluid-filled loops of the bowel in the left hemithorax - Shift of the cardiac silhouette to the right - Look for evidence of pneumothoraxpneumothorax
- 20. Chest X-Ray
- 21. Imagining study-2D Echography 2DE2DE: To exclude Cardiac anomalies (25%) and degree of PPHN Assessing myocardial function and determining whether the left ventricular mass is significantly decreased Renal USGRenal USG: Genitourinary anomalies occur in 6-8% of infants Cranial USGCranial USG for CNS anomalies
- 22. Investigations-Lab studies ABG (pre-right radial and post ductal-left radial or posterior tibial artery) measurements to assess for pH, PaCO2, and PaO2 Note the sampling site because persistent pulmonary hypertension of the newborn (PPHN) with right-to- left ductal shunting often complicates CDH The PaO2 is often higher from a preductal (right- hand) sampling site Serum lactate may be helpful in assessing for circulatory insufficiency or severe hypoxemia associated with tissue hypoxia
- 23. Medical Care in the delivery room: ( if the infant is known or suspected to have congenital diaphragmatic hernia) Immediately place a vented orogastric tube and connect it to continuous suction to prevent bowel distension and further lung compression Avoid mask ventilation and immediately intubate the trachea Avoid high peak inspiratory pressures and be alert to the possibility of early pneumothorax if the infant does not stabilize
- 24. Investigations Serum electrolytes, ionized calcium, and glucose initially and frequently Maintaining glucose levels in the reference range and maintaining calcium homeostasis are particularly important
- 25. Pre and Post Pulse Oxymetry Continuous pulse oximetry is valuable in the diagnosis and management of PPHN Place oximeter probes at preductal (right-hand) and postductal (either foot) sites to assess for a right-to- left shunt at the ductus arteriosus level
- 26. Procedures UAC insertion: For frequent ABG monitoring and BP monitoring UVC insertion for infusion of inotropes, Calcium and for venous access Venoarterial or venovenous ECMO support is an adaptation of cardiopulmonary bypass and involves a surgical team
- 27. NICU admission/Critically care Minimal Handling/stimulation, and gentle suctioning Maintain temperature Continuous monitoring of oxygenation, transcutaneous PaO2, PaCO2, blood pressure, and perfusion Maintain glucose (reflo regime) and ionized calcium
- 28. Inotropes for BP Use volume expansion and inotropic support with dopamine, dobutamine, or milrinone , 2-20 mcg/kg/min Dobutamine and milrinone may be particularly helpful if myocardial dysfunction is present Epinephrine infusions may be necessary in severe cases; low-dose epinephrine (< 0.2 mcg/kg/min) may help to promote pulmonary blood flow and improve cardiac output
- 29. Maintain PaO2/PaCO2 PaO2 concentrations greater than 50 mm Hg Permissive mild hypercarbia is allowed Maintain PH, avoid acidosis Inhaled INO ( Nitric Oxide) as indicated Magnesium sulphate loading and infusion if no INO available ECMO if available Sedation is an important adjunctive therapy, but the use of paralytic agents remains highly controversial
- 30. Sedation Fentanyl 1 mcg/kg/hour or Morphine infusion Paralysis with Pancuronium, Vancuronium (Controversial)
- 31. Surgical Care- Antenatal Open fetal surgery:Open fetal surgery: remove the compression of the abdominal viscera. High risk for fetus and the mother. No survival advantage. (Harrison et al, J Ped Surg, 1997) Fetal tracheal occlusion:Fetal tracheal occlusion: stimulation of lung growth with accumulation of fluid. Result in larger but persistent abnormal lung. Steroids therapy weekly to improve lung function is controversial (risk of brain and body development
- 32. Surgical Care-Time of surgery Circulatory stability, respiratory mechanics, and gas exchange deteriorate after surgical repair The ideal time to repair a congenital diaphragmatic hernia is unknown Some suggest that repair 24 hours after24 hours after stabilizationstabilization is ideal, but delays of up to 7-10 days are typically well tolerated, and many surgeons now adopt this approach Some surgeons prefer to operate on these neonates when normal pulmonary artery pressure is maintained for at least 24-48 hours based on
- 33. Approaches for surgical repair Abdominal subcostal Thoracotomy Laparoscopic vs Thoracoscopic MIS (Minimal Invasive surgery) ideal for Morgagni hernias but can be challenging because the peumoperitoneum widens the defect. Laparoscopy for Bochdalek’s has a high failure rate and is associated with pCO2 and acidemia↑ Contraindicated if very high pCO2. Thoracoscopy is better approach for Bochdalek hernias with recurrence of 14%. Open approach 3-22%. Small defect can be repaired primarily Large defect will require abdominal or thoracic muscle flaps, or prosthetic patch (tension free)
- 34. Surgery Before Surgery After Surgery
- 35. Follow up care GERD Growth Failure (FTT) Foregut dysmotility Chronic lung disease Scoliosis Pectus excavatum Neurodevelopmental delay, Cognitive skills, LD, seizures, Hearing loss
- 36. Further Inpatient Care-Respiratory care Severely affected infants have chronic lung diseasechronic lung disease May require prolonged therapy with supplemental oxygen and diuretics, an approach similar to that for bronchopulmonary dysplasia The use of steroids, particularly high doses for prolonged periods, is controversial and may hinder appropriate lung and brain development Late pulmonary hypertensionLate pulmonary hypertension has been successfully treated with low-dose inhaled nitric oxide
- 37. Neurologic evaluation Neurologist or developmental pediatrician perform an examination that includes an evaluation for CNS injury using head CT scanning or MRI The incidence of hearing loss appears to be particularly high in patients with congenital diaphragmatic hernia (approximately 40% of infants40% of infants) An automated hearing test should be performed prior to discharge
- 38. Gastroesophageal reflux (GERD) GERD is very high in patients who survive congenital diaphragmatic hernia, and studies document an incidence of 45-85%.45-85%. Severe reflux may result in chronic aspiration and is, therefore, aggressively treated Although most infants can be medically treated with H2-blockers or proton pump inhibitors in combination with a motility agent such as Domperidone, surgical intervention is sometimes required.
- 39. Further Outpatient Care- Failure To Thrive (FTT) Possible causes include increased caloric requirements due to chronic lung disease, oral aversion after prolonged intubation, poor oral feeding due to neurologic delays, and gastroesophageal reflux. More than 50% of patients are below the 25th50% of patients are below the 25th percentilepercentile for height and weight during the first year of life In one study, one third of infants required gastrostomy tube placement to improve caloric intake
- 40. Developmental Assessment Because of the risk for CNS insult and sensorineural hearing loss, infants should be closely monitored for the first 3 years of life, preferably in a specialty follow- up clinic These risks are particularly high in infants who are discharged home on supplemental oxygen Reassess hearing at age 6 months (and later if indicated) because late sensorineural hearing loss occurs in approximately 40% of patients40% of patients
- 41. School age Even if a child has no major neurodevelopmental delays, he or she should be evaluated prior to entering school to determine if any subtle deficits may predispose the child to learning disabilities.
- 42. Nursing related pointers Delivery room-Do not bag and Mask, early intubation Insert nasogastric tube to decompress stomach and gut Sat O2 monitor on right palm and left palm(pre and post) Thermoregulation maintain temp 36.7-37.3°C by control of ambient and/or skin temperature Minimal stimulation/HandlingMinimal stimulation/Handling, XR,suction and noise Strict input output UAC/UVC or IA line monitoring, perfusion chart
- 43. Nursing related pointers HFOV, ETT position, mechanical ventilation charting, prevent nosocomial pneumonia and infection control Educate use and connection for INO NOXBOX Avoid hypoxia, hypercarbia, acidosis Sedation, pain management Inline suctioning, Chest PT Developmental care- avoid noise, bright light etc Feeding, Expressing breast milk, Weight chart, wound care Positioning and posture: - Supportive positioning (Position infant with affected side down toPosition infant with affected side down to aid ventilation of the “good” lung)aid ventilation of the “good” lung) - Also position infant in a nesting position to decrease agitation Parent Education and support
- 44. Parent education Parents receiving the diagnosis of Congenital Diaphragmatic Hernia initially experience emotional distress, which has been shown to impair optimum learning Studies of prospective parents of an infant with a fetal anomaly revealed their inability to assimilate all the information given to them in one session Parents have indicated that both visual and auditory learning is important and have suggested that written material and drawings would be useful in helping parents retain and review information.
- 45. Parent education Description of Congenital Diaphragmatic Hernia Explanation of what to expect in the delivery room Tour of neonatal unit Explanation of what to expect upon admission to NICU and first day of life including intubation, ventilation, antibiotics, umbilical venous/arterial lines, IV therapy, gastric decompression and cardiac monitoring. Education upon admission to NICU: Reinforce information given prenatally as noted above Discuss plan of care given to the parents prenatally:
- 46. Parent Education Pre-Op: Update parents to plans for surgery and what to expect post-operatively Post-operative Education: Update parents about infant’s status post-operatively and review any new equipment, medication, or therapies that have been added to infant’s care. Discharge Education: General Infant Care Car seat Safety Care for the infant with reflux (as appropriate) Care for the infant on oxygen therapy (as appropriate)
- 47. Conclusion CDH is a congenital anomaly with a high mortality Usually associated with pulmonary hypoplasia and hypertension Surgical repair is only treatment Delayed surgery until the patient is stable is associated with better outcomes Congenital cardiac and renal diseases, hypoxemia and hypercapnia increases mortality HFOV, ECMO, iNO has improved the survival of CDH Permissive hypercapnia with acceptable pO2 has shown to improve survival Long term follow up is necessary to detect complications Tracheal occlusion in utero, keeps lung expanded but is a abnormal lung Primary repair if small defect, patch if large defect, to prevent tension